
What is Type 1 Diabetes?
Type 1 diabetes is an autoimmune condition in which your immune system attacks the insulin-producing beta cells in your pancreas.
The primary effect of type 1 diabetes is that it dramatically reduces the ability of your body to produce insulin, the master hormone responsible for promoting glucose uptake into cells in many tissues.
Without enough endogenous (self-made) insulin, people with type 1 diabetes require exogenous insulin, injected as needed via a syringe, pen, or insulin pump.
Inhaled insulin is also an option, albeit far less common.
Type 1 diabetes typically occurs in individuals under the age of 30, and if not treated can lead to a condition called diabetic ketoacidosis (DKA).
DKA is characterized by extremely high blood glucose levels (above 300 mg/dL) which result in excessive thirst, excessive hunger, unexplained weight loss, frequent urination, muscle cramping, and low energy.
The incidence of type 1 diabetes, along with all other forms of diabetes, has rapidly increased over the past 25 years for reasons that are still being studied.
Currently, estimates are that up to 10% of the US population lives with diabetes (34.2 million), with about 5% of that overall number living with type 1 diabetes (1.5-2 million people).
Researchers have been unable to isolate one specific cause of type 1 diabetes, but increasing evidence shows that there may be a number of different environmental triggers including specific proteins found in food, as well as viruses and bacteria.
This article will focus on some common symptoms of type 1 diabetes, the difference between type 1 and type 2 diabetes, and whether or not genetics affect your likelihood of getting type 1 diabetes.
We'll also discuss treatment options for type 1 diabetes, and how a plant-based, whole food diet may dramatically improve your quality of life if you’re currently living with type 1 diabetes.
Symptoms of Type 1 Diabetes

Most, but not all, cases of type 1 diabetes are diagnosed before age 30. However, there are exceptions to this rule, like Regina, who was diagnosed at age 44.
No matter when type 1 diabetes is diagnosed, the initial symptoms include, but are not limited to:
It’s important to understand that type 1 diabetes is a serious condition, and can dramatically increase your risk for other chronic diseases in the long term if your blood sugar remains uncontrolled.
Aside from the symptoms mentioned above, research suggests that 65% of people living with type 1 diabetes for more than 20 years will die of heart disease, as a result of high blood pressure, high blood glucose, and other complications.
This same research demonstrates that more than 50% of people living with type 1 diabetes for more than 30 years will die of kidney failure.
Fortunately, there are well-tested, evidence-based methods to manage type 1 diabetes, which we’ll cover below.
What's the Difference Between Type 1 and Type 2 Diabetes?
The main difference between type 1 and type 2 diabetes is simple. Type 1 diabetes is an autoimmune condition in which your body’s immune system mistakenly targets insulin-producing beta cells for destruction.
The process of autoimmunity begins with molecular mimicry, a sneaky tactic used by various bacteria and viruses in which pathogenic proteins attempt to evade detection by the human immune system by “disguising” themselves as mammalian proteins.
In both young children and adults, microscopic holes in the gut lining allow pathogenic proteins to pass directly from your digestive system into your blood before they have been sufficiently broken down by digestive enzymes.
Once these pathogenic proteins are present in your blood, your immune system recognizes them as foreign proteins and mounts an immune response that targets them for destruction.
But because these pathogenic proteins contain specific regions that mimic proteins found in your body, your immune system can mistakenly target proteins on human cells in tissues all over your body for destruction, setting the stage for an autoimmune reaction.
Think of type 1 diabetes as a form of biological “friendly fire” in which your immune system is hijacked by a pathogenic protein that tricks it into destroying critical human cells containing proteins with a similar structure on the surface of insulin-producing beta cells.
Type 2 diabetes, on the other hand, is not an autoimmune condition.
The majority of people with type 2 diabetes are able to produce sufficient insulin, but suffer from insulin resistance – a condition in which cells in your muscle and liver can’t respond to insulin effectively.
High levels of insulin resistance not only causes prediabetes and type 2 diabetes, it increases your risk for many chronic diseases like coronary artery disease, atherosclerosis, cancer, polycystic ovary syndrome (PCOS), peripheral neuropathy, Alzheimer’s disease, chronic kidney disease, and fatty liver disease (NAFLD).
According to the most recent research, 5-10% of people with diabetes have type 1 diabetes (about 1.5-2 million people) while between 90-95% of people with diabetes have type 2 diabetes (about 32 million).
Type 1 Diabetes and Insulin Resistance
Type 1 diabetes and insulin resistance are rarely referenced in the same context, since insulin resistance is the cause of type 2 diabetes.
However, insulin resistance is the underlying condition that causes high blood glucose and significant long-term tissue damage in people with type 1 diabetes.
This matters because insulin resistance is actually exacerbated by a high-fat, low-carbohydrate diet in people with type 1 diabetes, just like in people living with type 2 diabetes.
An animal-based ketogenic diet, a plant-based ketogenic diet, and a Paleo diet are all high-fat diets that are commonly prescribed for those with type 1 diabetes.
Because of this, it’s extremely important to be aware that even though severely reducing the grams of carbohydrates you consume by following a high-fat diet may help you control your blood glucose in the short-term, this may increase your chronic disease risk in the long-term.

Is Type 1 Diabetes Genetic?
Genetics likely play a role in the development of type 1 diabetes, but the research is currently unclear on the exact molecular mechanisms.
As mentioned above, the risk of developing type 1 diabetes is strongly associated with cow’s milk protein, enteroviruses, and mycobacterium avium paratuberculosis (MAP).
Scientists have been unable to isolate the exact mechanisms by which specific genes can influence your risk for type 1 diabetes, even though a genetic connection does exist.
According to the NIH, “A predisposition to develop type 1 diabetes is passed through generations in families, but the inheritance pattern is unknown.”
Fortunately, in almost all cases, you can effectively manage type 1 diabetes through healthy eating using a low-fat, plant-based, whole-food diet.
How is Type 1 Diabetes Treated?
In general, the treatment methodology for type 1 diabetes centers around monitoring blood glucose levels using a blood glucose monitor. Based on your blood glucose levels, the typical treatment model then prescribes a specific insulin dose, which is injected by an insulin pump, syringe, or pen.
Think of these insulin injections as a supplement to the insulin produced by your body (if any at all), in order to maintain your blood glucose within range.
The ‘Typical’ Treatment Model
Recently, many doctors have begun to follow a treatment methodology utilizing strategic lifestyle changes to improve blood glucose control.
Some of these recommendations, like increased physical activity, and reducing or eliminating refined sugars and other refined ingredients, can dramatically improve blood glucose control and reduce your risk for long-term complications.
However, there are also some major problems with this treatment model, which often focuses on carbohydrate counting, and high-fat, low carbohydrate diets.
Though these diets (Keto, Paleo, Atkins) can provide short-term results, over time they can actually result in increased insulin use, increased oral medication use, and increased A1c over time.
This may sound very different from what you’ve heard, and we know that can be surprising! Keep reading and we’ll explain why high-fat, low-carbohydrate diets are not ideal for people living with type 1 diabetes.
The Problem with High-Fat, Low-Carbohydrate Diets
The main issue with the current low-carbohydrate diets is that they ignore the underlying causes of high blood glucose levels (insulin resistance), and instead prescribe a ‘quick fix’.
In many cases, the high-fat, low carbohydrate intake approach results in low A1c values, reduced insulin requirements, weight loss, reduced fasting insulin, reduced fasting glucose, reduced triglycerides, and increased HDL cholesterol in the short-term.
However, a high-fat, low carbohydrate diet actually increases insulin resistance over time, and can cause long-term negative effects including:
If you’d like to read more about exactly why carb counting and a low carbohydrate diet isn’t right for you, you can dive even deeper into the science in this article debunking 7 misleading statements about ketosis and ketogenic diets.
The Low-Fat, Plant-Based, Whole-Food Nutrition to Maximize Insulin Sensitivity
For a long term solution, the research instead points to a low-fat, plant-based, whole-food diet that’s high in whole carbohydrates. This healthy diet results in dramatically increased insulin sensitivity, which also results in:
Is Type 1 Diabetes Reversible?
The idea that type 1 diabetes can be reversed is misleading. Though much research is being done on type 1 diabetes, at the moment type 1 diabetes has no known cure.
However, type 1 diabetes can be effectively managed, so that the risk of developing long-term complications is minimized.
Currently, the most effective way to manage the underlying causes and risks of type 1 diabetes are through a low-fat, plant-based, whole-food diet as described below.
Diabetes Management Through Diet: Guidelines
Red Light, Green Light, Yellow Light Foods
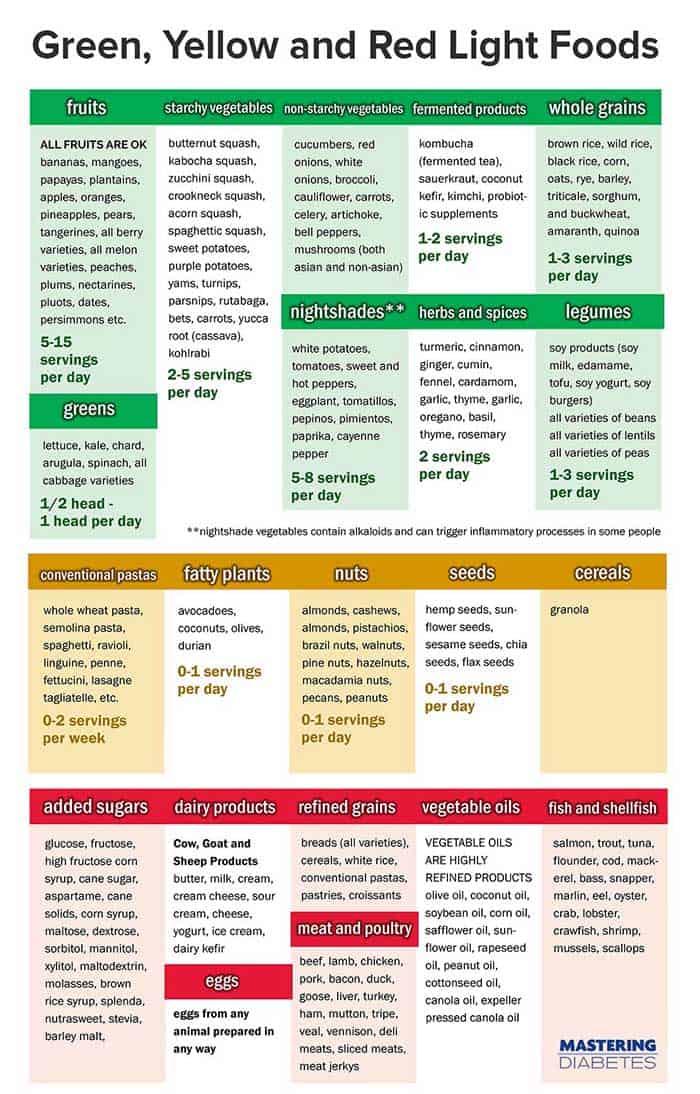
The diet guidelines for managing your blood glucose levels while living with type 1 diabetes are actually very simple, following a clear “green light, yellow light, red light,” categorization for foods.
“Green light” foods include all fruits (except avocado, durian, and dates), starchy and non-starchy vegetables, all legumes (except soybeans), intact whole grains (minimally processed), and herbs and spices.
Green light foods are foods that you can eat as much as you want, as these are unrefined whole foods low in fat with a high nutrient density that have been demonstrated to reverse insulin resistance.
“Yellow light” foods include whole grain or bean pastas, whole grain cereals, refined grains, whole grain bread and tortillas, avocados, nuts, seeds, coconut meat, soybeans, and soy products.
Yellow light foods are foods okay to include in small quantities, because they are slightly processed or have higher fat content. They shouldn’t be daily staples, but are still considered a “healthy” choice.
“Red light” foods include all red meats, all white meats, all seafood, eggs (of any kind), dairy products, refined oils, and refined sugars (simple carbohydrates).
Red light foods are foods that we recommend removing from your cabinet, your fridge, and your plate.
These foods are documented by evidence-based research to cause insulin resistance, increase your blood glucose (fasting and post-meal), and promote chronic diseases in individuals with type 1 diabetes.
Compared to What You’ve Heard
The major difference between the low-fat, plant-based, whole food diet, a low-carbohydrate diet, or other methods like the glycemic index becomes apparent in the long-term.
Low-carb diets provide quick results, but as we mentioned above, they can drastically increase insulin resistance and therefore increase your risk for many chronic diseases in the long term.
The glycemic index also focuses on the short term effects of specific foods, rather than increasing the nutrient density of your overall diet.
Meanwhile, the low-fat, plant-based, whole food diet provides excellent short-term results and dramatically reduces your risk for chronic diseases like coronary artery disease, atherosclerosis, cancer, obesity, polycystic ovary syndrome (PCOS), peripheral neuropathy, Alzheimer’s disease, chronic kidney disease, and fatty liver disease in the future.
The Results
One of the largest communities surrounding low-fat, plant-based, whole-food diets is right here at Mastering Diabetes, where thousands of people have already regained control of their blood glucose, lost weight, and improved their energy and overall health just by changing their diet.
For example, Jack was able to regain control of his life after 75 years of living with type 1 diabetes and found freedom.
After following the low-carbohydrate diet to the T and exercising frequently, Regina was still gaining weight and had an A1c over 12.0%.
After switching to a low-fat, plant-based, whole-food diet, Regina cut her A1c by more than a half by her next doctor’s visit.
We’ve got a helpful, comprehensive guide for your food choices below.
Type 1 Diabetes Diet: Foods to Eat and Avoid
Example Type 1 Diabetes Meal Plan
One of the biggest challenges people face when switching to a low-fat, plant-based, whole-food diet is the feeling like they’re giving up some of their favorite foods.
The reason: almost all of the red light foods are rich in saturated fat, refined sugars, protein, or synthetic texturizers and fillers, and many are manufactured in a laboratory to taste good.
To help overcome this challenge, we have two recommendations.
Recommendation #1: For best results when transitioning to a low-fat, plant-based, whole-food diet, transition gradually.
To help with the feeling that you’re giving something up, we recommend changing one of your meals each week, starting first with breakfast, then breakfast and lunch, until finally all three meals of the day are fully optimized.
Recommendation #2: Eat a wide variety of foods from our recipe database, which is full of suggestions for breakfast, lunch, dinner, desserts, and snacks that taste great, are great for you, and are 100% low-fat, plant-based, and whole-food approved. We created the chart below to assist you with meal planning.
*Note: Even in meals that have ‘no change’, we recommend replacing one red light food with a yellow light or green light food, or even trying to eat yellow and green light foods exclusively. Even one change of ingredients can have significant positive benefits for your diabetes health.
Week 1 Meal Plan
Header | Breakfast | Lunch | Dinner |
|---|---|---|---|
Day 1 | No Change* | No Change* | |
Day 2 | No Change* | No Change* | |
Day 3 | No Change* | No Change* | |
Day 4 | No Change* | No Change* | |
Day 5 | No Change* | No Change* | |
Day 6 | No Change* | No Change* | |
Day 7 | No Change* | No Change* |
Week 2 Meal Plan
Header | Breakfast | Lunch | Dinner |
|---|---|---|---|
Day 1 | No Change* | ||
Day 2 | No Change* | ||
Day 3 | No Change* | ||
Day 4 | No Change* | ||
Day 5 | No Change* | ||
Day 6 | No Change* | ||
Day 7 | No Change* |
Week 3 Meal Plan
Header | Breakfast | Lunch | Dinner |
|---|---|---|---|
Day 1 | |||
Day 2 | |||
Day 3 | |||
Day 4 | |||
Day 5 | |||
Day 6 | |||
Day 7 |
If you would like personal guidance, recommended recipes, or advice in making the transition or adjusting your diabetes nutrition to fit your personal needs, you can work with our coaches in the Mastering Diabetes Coaching Program.
Other Articles You Might Like...
Lower Your A1c and Fasting Blood Sugar... Guaranteed

Your results are guaranteed. Join more than 10,000 ecstatic members today
Personalized coaching puts you in immediate control of your diabetes health, helps you gain energy, improves your quality of life, and reduces or eliminates your meds.






