Are you struggling with low energy, weight gain, high cholesterol, high blood pressure or type 2 diabetes?
Are you confused about what to eat to control your blood glucose levels well and reverse chronic disease in your body?
Are you tired of reading conflicting information on the internet in your quest to find a permanent solution to your ailing health?
If so, you’ve come to the right place.
In this article, I’ll explain in grave detail about the exact foods to eat to reverse insulin resistance, high blood pressure, high cholesterol, type 2 diabetes and many other chronic diseases, backed by almost 100 years of evidence-based research.
How I Increased My Insulin Sensitivity by More Than 600%

My name is Robby, and I was diagnosed with type 1 diabetes on January 26th, 2000. At the time I was diagnosed, I was 12 years old and I ate a Standard American Diet (SAD).
As a teenager I experienced many health issues including allergies, cystic acne, warts on my feet, and plantar fasciitis.
In 2002, I began using multivitamins and other miscellaneous supplements. I was influenced by my dad who was selling them through a network marketing company. This was the beginning of me thinking about nutrition and food as something that impacted my health.
In 2003, I began experimenting with other dietary approaches because I had read about the negative effects of eating a Standard American Diet (SAD), and wanted to make conscious decisions about what I ate.
One of my first experiments was to eat a Weston A. Price diet, which contained a considerable amount of grass-fed beef and raw milk.
Even though my wellbeing marginally improved by eliminating processed foods entirely, I didn’t experience any significant improvements in my diabetes health, and my insulin requirements remained unchanged.
In early 2006, I stumbled across a book that changed my life forever called Natural Cures They Don’t Want You to Know About by Kevin Trudeau. I remember walking away with the belief that I can and will reverse type 1 diabetes, and that one day I will no longer need insulin to manage my blood glucose.
Reading this book marked the beginning my desire to learn about autoimmunity and how stem cells could promote new beta cell growth. I was committed to doing everything in my power to reverse type 1 diabetes.
*Note: Kevin Trudeau has since been imprisoned for misleading health claims and fraudulent advice. I do not condone his advice, it was merely a book that planted a seed to learn more about evidence-based lifestyle change.
In September of 2006, I saw an inspiring movie called Raw for 30 Days and began eating a plant-based, ketogenic diet immediately. I had heard that eating a plant-based ketogenic diet was an avenue to eliminate insulin injections entirely, and I loved that idea.
By eating this plant-based, high-fat diet, I derived the bulk of my calories from oil, nuts, and seeds, and I also ate a substantial amount of green leafy vegetables.
I ate about 30 grams of total carbohydrate per day and injected the smallest amount of insulin I’ve ever injected – about total 10 units per day (including basal and bolus). My carbohydrate-to-insulin ratio (a simple measurement of insulin sensitivity) was 3 grams/unit, meaning that for every 3 grams of carbohydrate that entered my mouth, I required 1 unit of insulin.
Insulin sensitivity can be calculated in many ways using sophisticated laboratory equipment and costly procedures. A simple and highly effective measure that we use is the ratio of total carbohydrate intake to total insulin use in a 24-hour period (including basal and bolus insulin) when you maintain your blood glucose in an acceptable range (70-180 mg/dL) for 70-100% of the day. The calculation is shown here:
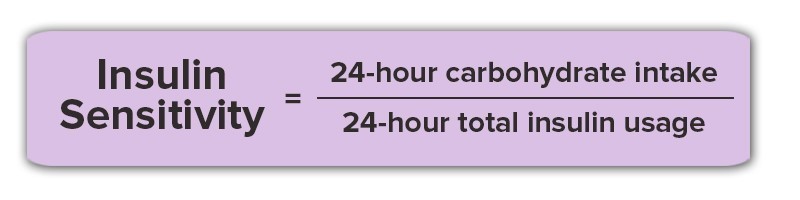
I stopped eating the ketogenic plant-based diet because I had no energy and almost passed out several times on my college campus. I was scared and unsure if eating a plant-based ketogenic diet was safe for someone living with type 1 diabetes
Note: Dr. Cousens is no longer see patients with type 1 diabetes or accepts them at his retreat facility.
Around October 2006, I heard a podcast where Doug Graham, DC, was explaining the benefits of eating a diet consisting of mainly fruits and leafy greens. Everything he said made a lot of sense to me, so I decided to begin down the path of increasing my consumption of carbohydrate-rich foods to see what added benefits I may experience.
I experienced a rapid increase in my own insulin sensitivity in only a few weeks. At the beginning my carbohydrate-to-insulin ratio was 3:1 grams/unit, and within a few weeks it climbed to 24:1 grams/unit, as you can see in the graph below.
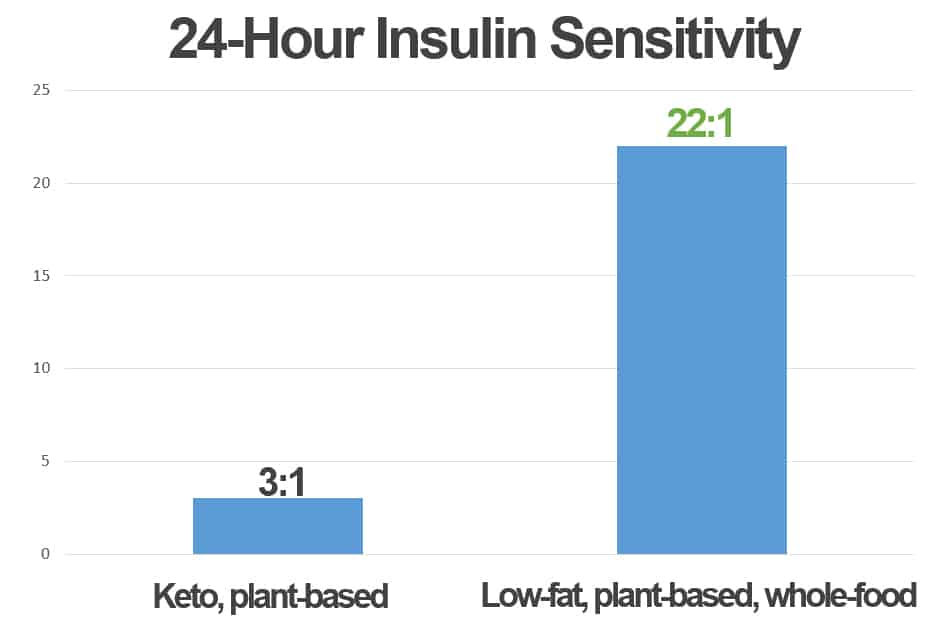
There are days where I’ll eat approximately 750 grams of total carbohydrate and use approximately 34 units of total insulin, which means that my 24-hour insulin sensitivity is 22 grams/unit. As compared with when I ate a plant-based, ketogenic diet, an insulin sensitivity of 22 grams/unit is 600% higher than 3 grams/unit.
And to be frank, there are days where my insulin sensitivity is even higher. If you follow me on Instagram (@mindfuldiabeticrobby) you will see me share my daily food consumption, insulin use and also my time in range shown by a Dexcom G6 CGM that I wear.
It’s important to understand that even though my total insulin use increased, the amount of insulin I now use is proportional to what my pancreas would normally secrete if my beta cells were functioning properly
The reason I know this to be true is because the average non-diabetic pancreas secretes between 30-50 units of insulin per day
In the early stages of my transition to a low-fat, plant-based, whole-food diet, my energy levels soared to new heights, I began eating new fruits that I’d never heard of before, including mamey sapote, sapodilla, persimmons, and black sapote to name a few.
Now, 13 years later, I continue to eat the same diet because it makes me feel incredible and maximizes my insulin sensitivity. I have become a master of consistency, and by being consistent I’m able to control my blood glucose with precision.
Today, I feel the best I have ever felt in my life. My skin is clear, I am no longer plagued by seasonal allergies, I no longer suffer from plantar fasciitis, and most importantly my insulin sensitivity is at an all-time high
Unfortunately, I don’t have the answer for reversing type 1 diabetes yet, but there is one thing I can promise you: my change insulin sensitivity is not atypical – my rapid increase in insulin sensitivity has a detailed and rigorous scientific explanation that has changed my life and the lives of thousands of people I’ve taught.
In this article you will learn about almost 100 years of evidence-based research that unequivocally demonstrates the fact that low-fat, plant-based, whole-food nutrition is a powerful way to maximize your insulin sensitivity – following the same approach as me.
The Scientific Research Behind Insulin Sensitivity
This article summarizes 18 peer-reviewed articles dating back to 1926. Many papers have been published in the most prestigious journals such as: Lancet, New England Journal of Medicine, Journal of the American Medical Association, Archives of Internal Medicine, Diabetes Care and many more.
All of the research presented below showcases one simple point – dietary fat inhibits the action of insulin. As the amount of dietary fat increases, insulin becomes less effective. As the quantity of dietary fat is reduced, insulin becomes more effective.
To be clear, 5 of the 18 studies listed below that did not measure insulin sensitivity directly. Although they did study glucose tolerance and the data represent an indirect indicator of improved insulin sensitivity.
1. Sansum, et al. The Use of High Carbohydrate Diets in the Treatment of Diabetes Mellitus. Journal of the American Medical Association, 1926
In the mid 1920’s, W.D. Sansum, MD, and other physicians began experimenting with diets containing more carbohydrate-rich food. Insulin was discovered in 1921, and prior to its discovery diabetes was essentially a death sentence.
Patients were taught to eat very low-carbohydrate, low-calorie diets and the quality of life was low. They did not have energy, could not think clearly and the diets were barely palatable.
In 1926, Dr. Sansum published a paper reporting on what he called a “radical experiment” he’d been conducting on 150 of his patients. He increased carbohydrate-rich food in his patients diets by adding white bread, potatoes, low-fat milk and fruit (2).
The goal was to make his patients feel better and improve their quality of life. That’s exactly what happened, but the real surprise was that his patient’s insulin requirements did not change.
Even though the diet was still high-fat (43% of calories), simply adding more carbohydrate-rich food and lowering the overall fat content resulted in significantly improved insulin sensitivity.
When eating a significantly higher carbohydrate diet, Dr. Sansum’s patients were able to use the same amount of insulin to escort more glucose out of their bloodstream and into tissues, thus demonstrating improved insulin action.
Additionally, Dr. Sanum reported the following benefits in his patients:
2. Sweeney, et al. Dietary Factors that Influence the Dextrose Tolerance Test. Archives of Internal Medicine, 1927
In 1927, J. Shirley Sweeney, MD, published a fascinating study with 23 male medical students split into four groups. The subjects in the first group were given a high-protein diet consisting of lean meat and egg whites. Subjects in the second group were fed a fat diet included oil, mayonnaise, cream, and butter.
Subjects in the third group were not given any food, and instead fasted for two days. Subjects in the fourth group were given a carbohydrate-rich diet consisting of sugar, candy, pastries, bread, potatoes, syrup, fruit, brown rice, and oats.
All subjects underwent an oral glucose tolerance test, and the results were fascinating. The carbohydrate diet showed the greatest level of glucose tolerance. At the 2-hour mark, the average blood glucose amongst the carbohydrate group was 96 mg/dL, which is considered a non-diabetic blood glucose value despite the fact that they ate processed carbohydrate-rich junk food.
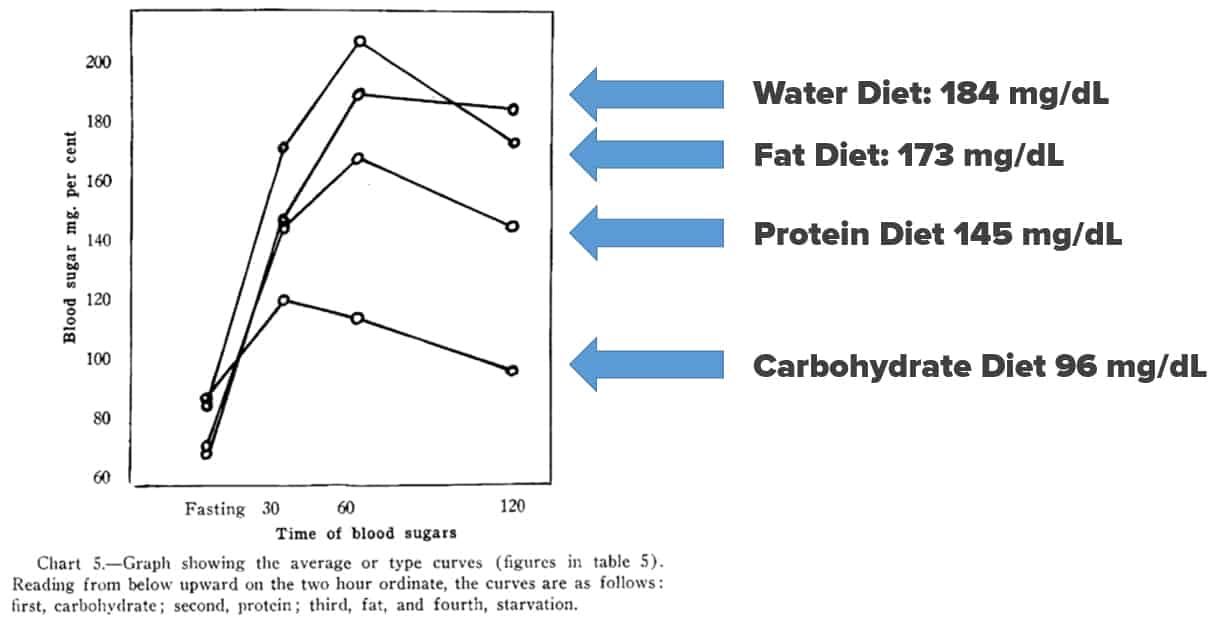
The average blood glucose level on the high-fat diet was 173 mg/dL, which suggests that in as little as 2 days, non-diabetic medical students began displaying the symptoms of type 2 diabetes. In response to this, Dr. Sweeney took his experiment one step further.
The students who showed the highest blood glucose readings on the high-fat diet were fed the high-carbohydrate diet and vice versa.
When these students were switched from one diet to the next, their blood glucose values changed rapidly. Those who ate a high-fat diet experienced blood glucose values greater than 190 mg/dL and those that ate a carbohydrate-rich diet experienced blood glucose less than 100 mg/dL. (3)
This evidence was one of the first papers to clearly demonstrate that high blood glucose occurs in response to an increasing quantity of dietary fat (and not carbohydrate energy).

3. Rabinowitch, I, M. Effects of the High Carbohydrate-Low Calorie Diet Upon Carbohydrate Tolerance in Diabetes Mellitus. The Canadian Medical Association Journal, 1930
In 1930, Israel Rabinowitch, MD, started experimenting with high-carbohydrate, lower-fat diets in his patients. He used a very methodical approach, where he taught the diet to patients using wooden blocks to help them understand portion sizes (4).
His diet plan consisted of the following:

The bread alone contained 162 grams of total carbohydrate per day, which was a significant departure from standard treatment at the time. Dr. Rabinowitch made it very clear that bacon, fatty meats, fish, and cream were forbidden, with a total of approximately 24% of total calories of fat per day.
In 50 patients, Dr. Rabinowitch reported the following results
The brilliance of this study is that his patients were not calorie restricted – they ate a similar number of calories on both diets.
4. Rabinowitch, I, M. The Present Status of the High Carbohydrate-Low Fat Diets for the Treatment of Diabetes, The Canadian Medical Association, 1932
In 1932, Dr. Rabinowitch published a paper sharing the results of 500 patients who improved their blood glucose control and overall health eating a high-carbohydrate diet as compared with a low-carbohydrate diet (5).
A lot of Rabinowitch’s success came down to his ability to teach patients how to eat a high-carbohydrate diet and follow it. In this paper Dr. Rabinowtich wrote:
“Diabetes does not appear to be due to defective production of insulin but to interference with the action of a normal supply.”
In this paper, Dr. Rabinowitch identified that insulin production is not the problem for most people living with diabetes, but that a high-fat diet interfered with insulin action.
5. Rabinowitch, I, M. Effects of the High Carbohydrate-Low Calorie Diet Upon Carbohydrate Tolerance in Diabetes Mellitus. The Canadian Medical Association Journal, 1935
In 1935, Dr. Rabinowitch published another paper involving 100 patients in which 50 were treated with his old, low-carbohydrate diet consisting of 60% of daily calories coming from dietary fat, and 50 were treated with a new diet containing 24% of daily calories. He followed patients in both groups for 5 years (6).
In patients who followed a diet containing 60% fat, the average daily insulin use fell from 32.2 units per day to 31.8 units per day over the course of 5 years, a total reduction of 1%.
Patients who ate the reduced-fat diet reduced their insulin use from 24.6 units per day to 10.6 units per day, a 57% reduction in total insulin use. Twelve patients who ate the high-carbohydrate diet were able to discontinue their use of insulin altogether compared to four people following the control diet.
Patients who ate the reduced-fat diet reduced their insulin use from 24.6 units per day to 10.6 units per day, a 57% reduction in total insulin use. Twelve patients who ate the high-carbohydrate diet were able to discontinue their use of insulin altogether compared to four people following the control diet.

In patients following the reduced-fat diet, Dr. Rabinowitch reported the following observations:
Rabinowitch and co-investigators concluded:
“Suffice it to say that it now appears to be fairly well established that carbohydrates improve whereas fats impair, carbohydrate tolerance; and that carbohydrates increase whereas fats decrease the sensitivity of the individual, animal and man, to insulin.”
6. Himsworth, H, P. High Carbohydrate Diets and Insulin Efficiency. The British Medical Journal, 1934
At the same time as Dr. Rabinowitch, H.P. Himsworth, the Director of the Medical Unit at the University College Hospital in London, conducted fascinating studies on topic of insulin sensitivity, establishing himself as a true pioneer in the field of diabetes research.
In this particular study, the participants were healthy males between the ages of 18 and 22. Dr. Himsworth chose to use healthy subjects (people living without diabetes) because he wanted to explore the mechanism that caused the body to be able to utilize carbohydrate in the presence of insulin. He chose to study subjects whose pancreases were capable of manufacturing and secreting insulin (7).
Participants were fed either a high-carbohydrate, low-fat diet or a low-carbohydrate, high-fat diet. They consumed one diet for at least a full week, had their insulin sensitivity tested, and then placed on the opposite diet for at least a full week and were subsequently tested.
The study was carried out in a hospital setting so it was ensured that participants would follow the diet with 100% compliance.
What happened?
According to the results:
“It is evident that on the high fat diet, insulin takes longer to act, and then acts more slowly on the blood sugar than when the subject is given a high carbohydrate diet.”
In a dietary high-fat environment, glucose tolerance is compromised. When challenged with an oral glucose tolerance test, those eating a high-fat diet experienced blood glucose as high as 200 mg/dL, whereas those eating a high-carbohydrate diet never experienced a blood glucose in excess of 120 mg/dL.
In this study he established that the higher the carbohydrate content of the diet, the more effective insulin became.
The image below shows a direct comparison of glucose tolerance on a high-fat and high-carbohydrate diet (containing the same number of calories) in one subject.
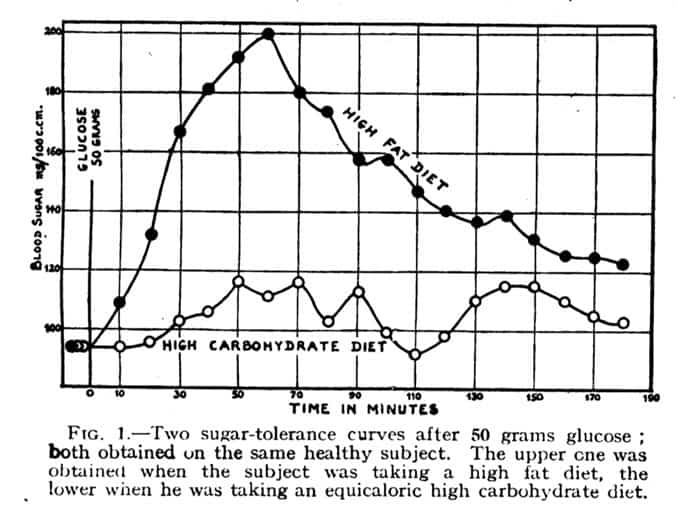
7. Himsworth, H, P. The dietetic factor determining the glucose tolerance and sensitivity to insulin in healthy men, Clinical Science, 1935
In 1935, Dr. Himsworth published another rigorous study on small group of healthy young men. All 5 subjects were fed 7 different diets for a minimum of 7 days each (8).
Below are the results of insulin sensitivity tests in one healthy, non-diabetic patient who was fed seven different diets, ranging from 13-80% calories from fat.
Important to observe is the shaded region in the upper right corner of each graph – the larger the shaded region, the higher the insulin sensitivity.
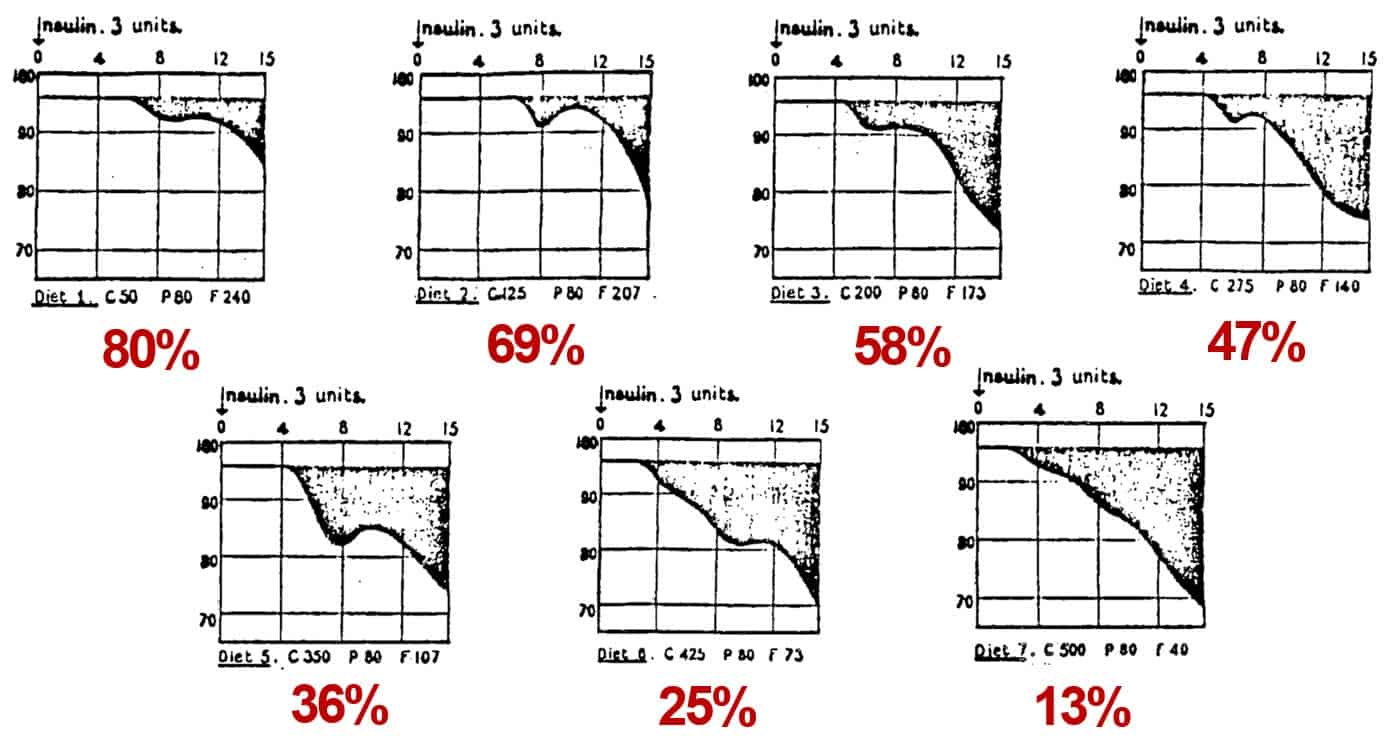
Patients were injected with 3 units of insulin, and researchers measured (a) how long it took insulin to lower blood glucose and (b) the amount of blood glucose reduction. They discovered the following:
In conclusion, Dr. Himsworth wrote the following:
"It is demonstrated that the efficiency with which a standard dose of crystalline insulin acts on the blood sugar is determined by the carbohydrate content of the diet so that the greater the amount of carbohydrate in the diet the greater the sensitivity of the organism to insulin."
Walter Kempner, MD – The Rice-Fruit Diet
In 1939, Walter Kempner, MD, from Duke University created the rice-fruit diet to treat malignant hypertension, a condition that was considered “incurable” at the time.
Dr. Kempner devised a diet for these patients consisting of white rice, sugar, fruit, and fruit juice, comprised of 94% carbohydrate, 2% fat, and 4% protein, suspecting that the amount of dietary protein played a major role in blood pressure.

The rice-fruit diet was Dr. Kempner’s attempt at creating a no-salt, no-cholesterol diet containing almost pure carbohydrate energy. His original intention was to reverse malignant hypertension, a condition, but in the process of teaching his patients how to dramatically reduce their blood pressure eating the rice-fruit diet, he inadvertently reversed the following conditions:
It’s important to note that despite the fact that the rice-fruit diet contained highly refined foods, it was still very effective at reversing many chronic diseases.
To study the rice-fruit diet further, Dr. Kempner next asked: What would happen if people living with diabetes ate the rice-fruit diet?
8. Kempner, Lohmann Peschel, & Schlayer. Effect of Rice Diet on Diabetes Mellitus Associated With Vascular Disease. Postgraduate Medicine, 1958
In 1958, Dr. Kempner published a paper reporting results of 100 diabetes patients in which he reported the following (9):
Take a moment and think about this carefully: Conventional diabetes wisdom states that foods high in carbohydrate energy will exacerbate diabetes and increase your insulin and oral medication requirements, especially if the source of carbohydrate energy includes refined foods like white rice and white sugar.
Therefore, Dr. Kempner’s rice-fruit diet should have resulted in metabolic disaster for his patients living with type 2 diabetes because it consisted of mainly rabidly absorbed carbohydrate energy.
The rice-fruit diet should have increased insulin requirements, caused unwanted weight gain, and promoted cardiovascular disease. But it didn’t. Why?
Because the rice-fruit diet was so low in total fat that his patient’s insulin sensitivity increased, resulting in a significantly higher ability to utilize glucose for fuel in their muscles and liver.
Critics of this study point out the fact that 9 of the 100 patients died during the period of observation. The reason for this is not because the rice-fruit diet was harmful, but because Dr. Kemper’s patients were incredibly sick, and were willing to try his “radical” approach to improve their overall health. Separate from the deaths reported in this study, the overall results of the rice-fruit diet in thousands of patients is absolutely remarkable.
9. Kempner W, et al. Treatment of massive obesity with rice/reduction diet program. An analysis of 106 patients with at least a 45-kg weight loss. Archives of Internal Medicine, 1975
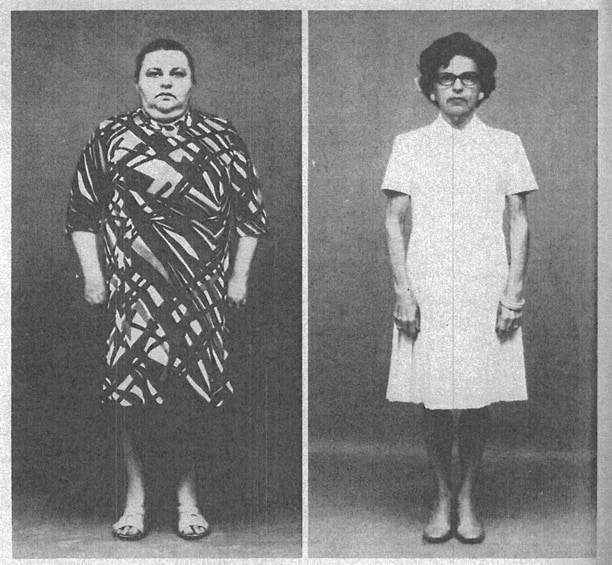
In 1975, Dr. Kempner published an analysis of 106 patients who had lost a minimum of 100 pounds eating the rice-fruit diet (10).
One female patient experienced the following:
After 8 months of the rice-fruit diet, the following happened:
And make no mistake, the patients in his studies were not selected because of excellent results. The results of his experiments were extremely repeatable and showed dramatic improvements in many aspects of metabolic health in addition to improved blood glucose.
10. Singh, Rangoon, & Colonel. Low-Fat Diet and Therapeutic Doses of Insulin in Diabetes Mellitus. The Lancet, 1955
In 1955, Inder Singh published a study on 80 patients with insulin-dependent type 2 diabetes.
He placed subjects on a diet consisting of:
Most patients ate 1,600 to 2,200 calories per day, and a few underweight patients ate 4,000 to 4,500 calories per day, and all patients were instructed to eat enough to prevent against weight loss.
After only 3-6 weeks, Singh observed that 63% of his patients became non-diabetic and did not require insulin any longer. After 18 weeks, 80% of his patients were non-diabetic and did not require insulin any longer.
Six patients who initially required 80-120 units of insulin per day gained full control of their blood glucose using 20-40 units of insulin per day following 6 weeks of the low-fat, high-carbohydrate diet (11).
He concluded this study by stating:
“There is no indication that healthy people taking a diet high in carbohydrates are especially liable to diabetes; in fact, numerous observations show improvement of carbohydrate tolerance following its greater intake.”
11. Brunzell, et al. Improved Glucose Tolerance with High Carbohydrate Feeding in Mild Diabetes. The New England Journal of Medicine, 1971
In the early 1970’s, John D. Brunzell, MD conducted a study in 22 subjects, 13 of which were living with prediabetes (12).
The patients were fed a weight-maintaining control diet containing 40% of calories coming from fat for 8-10 days, then switched to a weight-maintaining, low-fat processed diet for 10 days, with 0% of calories coming from fat.
Although eating a zero-fat diet is impossible when eating whole foods, Dr. Brunzell was able to invent a 0% fat diet by feeding his patients nothing but pure sugar and pure protein. This experimental diet was specifically designed to contain 0% fat, so that he could investigate it’s effects on insulin sensitivity without confounding variables.

All 22 patients in his study experienced a drop in their fasting blood glucose values – those without diabetes experienced an 8% reduction in fasting blood glucose, and those living with prediabetes experienced a 9.6% reduction in fasting blood glucose.
In the same study, 12 of the patients were administered an oral glucose tolerance test (OGTT) which measured their glucose and insulin levels in response to a glucose challenge.
Those in the high-carbohydrate group experienced reduced blood glucose and insulin levels at all time points during the OGTT, even though their diet consisted of refined sugar and protein.
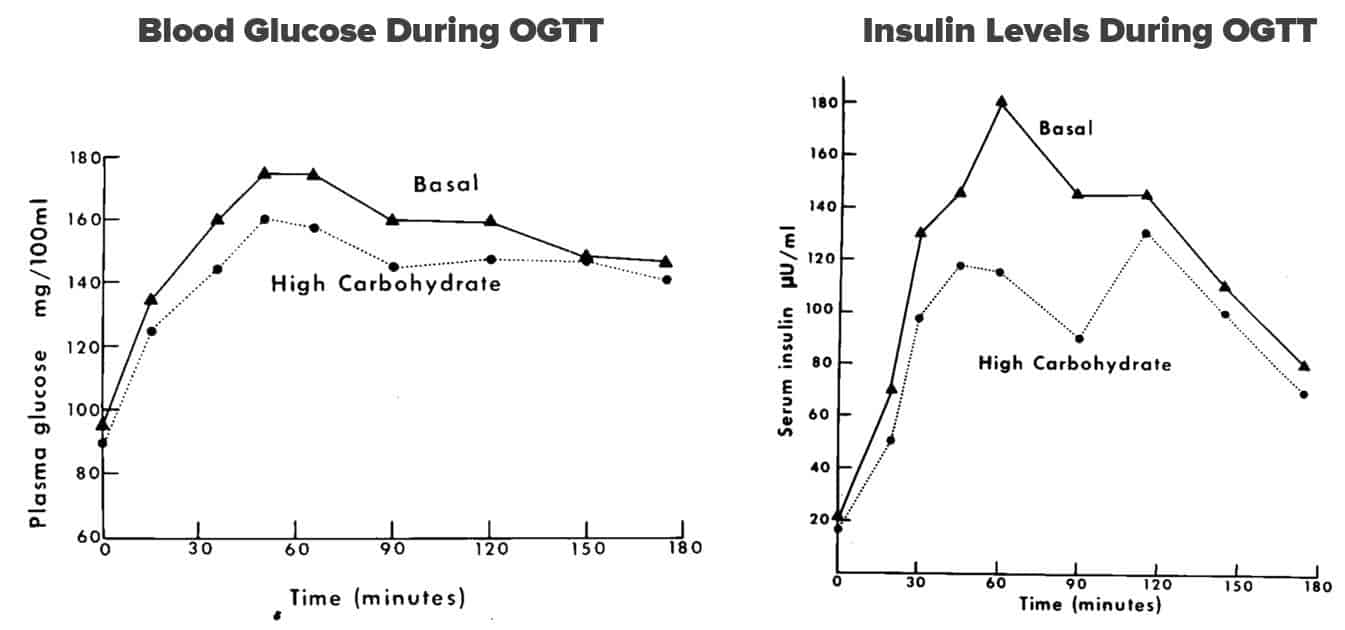
Perplexed by his own results, Dr. Brunzell wrote the following:
“How then, is the paradox of improved glucose tolerance with unchanged insulin response explained? These data suggest that the high carbohydrate diet increased the sensitivity of peripheral tissues to insulin.”
12. Kiehm, et al. Beneficial effects of a high carbohydrate, high fiber diet on hyperglycemic diabetic men. The American Journal of Clinical Nutrition, 1976
In 1976, Tae Kiehm, MD published the results of a study involving 13 patients living with diabetes, experiencing significant fasting hyperglycemia and using either insulin or oral medications to manage their blood glucose.
He compared the American Diabetes Association (ADA) diet containing 34% of calories from fat to a low-fat diet, containing 9% of calories coming from fat (13).
After only 14 days eating a low-fat diet, the researchers reported the following results:
Medications | ADA (34% Fat) | Low-Fat (9% Fat) | Notes |
|---|---|---|---|
Sulfonylureas | 5 | 0 | |
15-20 units insulin/d | 5 | 1 | Dropped from 28 to 15 units |
40-55 units insulin/d | 3 | 3 | 234g to 414g carbohydrate |
Researchers reported the following in these study subjects:
13. Anderson JW, Ward K. High-carbohydrate, high-fiber diets for insulin-treated men with diabetes mellitus. Am J Clin Nutr. 1979
Despite the research conducted by Sansum, Sweeney, Rabinowitch, Himsworth, Singh, Kempner, and others, many scientists questioned whether improvements in insulin sensitivity occurred simply because patients lost weight, not because they ate a low-fat diet.
To uncouple these two variables, James W. Anderson, MD and Kyleen Ward, RD conducted a study in 1979 in which they enrolled 20 subjects who had been living with type 2 diabetes for up to 20 years (14).
They fed participants a low-fat, plant-based, whole-food diet and demanded that their patients eat enough to prevent weight loss. Some subjects complained of physical discomfort from eating so much food, but the protocol ensured that all subjects remained weight stable.
By doing this, they could then study how insulin requirements changed on a low-fat diet, independent of weight loss.
The study involved 20 insulin-dependent lean men with a fasting blood glucose greater than 200 mg/dL. Subjects were fed a weight-maintaining control diet for an average of 7 days, containing 37% of calories from fat, then switched to a weight-maintaining, low-fat diet for 16 days containing 9% of calories from fat.
Insulin requirements plummeted by an average of 58 percent in the group that ate a low-fat diet, whereas insulin requirements did not change in those eating a conventional diabetes diet. Ten out of 20 subjects were able to discontinue taking insulin altogether, and those who continued insulin therapy were able to reduce their dosages between 7-98%.
The most surprising result was that more than 50% of subjects discontinued insulin completely after only 16 days on a low-fat diet, even having lived with type 2 diabetes for a minimum of 1 year.
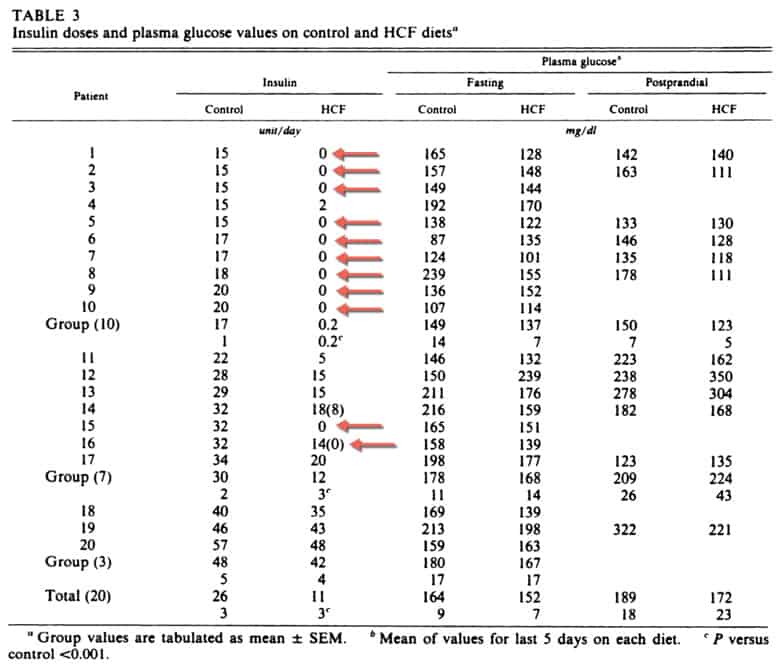
All patients in this study reduced or discontinued insulin and reduced their cholesterol levels, demonstrating that reduced dietary fat results in reduced biological insulin need, independent of weight loss.
14. Shintani, et al. Obesity and cardiovascular risk intervention through the ad libitum feeding of traditional Hawaiian diet. The American Journal of Clinical Nutrition, 1991
In 1991, Terry Shintani, MD, conducted a study including 19 obese Native Hawaiians in which he fed them an ad libitum plant-based diet for 21 days consisting of 7% calories from fat. (15)
Participants in the study visited a community center for the duration of the 21-day study and had all meals and snacks provided. The participants were required to come to the community center twice a day.
Study subjects were encouraged to eat as much as they wanted of the Native Hawaiian inspired diet, focused on carbohydrate-rich foods such as taro, sweet potato, yams, fruit, vegetables and greens, and were told to limit their intake of chicken and fish to 5-7 ounces per day.
Before the study started, the participants ate an average of 2,600 calories per day (3.8 pounds of food). On the high-carbohydrate traditional Hawaiian diet, study subjects ate approximately 1,000 calories less per day (4.1 pounds of food).

Each day, the participants level of satiety was tested using a hunger-satiety scale. If they were not satisfied, they were encouraged to eat more in order to remain fully satisfied throughout the day.
Even though subjects ate 41% fewer calories, the hunger-satiety scale showed that participants experienced moderate to high levels of satiety. They ate as much as they desired, felt full, and lost weight.
After 21 days of eating unlimited quantities of carbohydrate-rich foods, participants experienced the following results:
The drop in fasting glucose is noteworthy, especially considering patients were taking less medication.
Despite the fact that this study did not directly measure insulin concentrations, it demonstrated significant improvements in diabetes health using a low-fat, plant-based, whole-food diet
15. Barnard, Jung, & Inkeles. Diet and Exercise in the Treatment of NIDDM: The need for early emphasis. Diabetes Care, 1994
In 1994, James Barnard, PhD, published an article reviewing 652 patients who attended the Pritikin Longevity Center between 1977 and 1988. At the center, they participated in a 26-day residential program, eating a low-fat diet containing less than 10% of total calories from fat (16).
The diet consisted of high-starch foods, including bread, peas, beans and vegetables, as well as small amounts of animal products and low-fat dairy
Dr. Barnard reported the following results from the 26-day residential program:
Patients who followed the dietary protocol increased their intake of carbohydrate-rich foods from starchy vegetables and decreased or eliminated their need for oral medications and insulin, suggesting that their responsiveness to insulin increased as a result of this dietary change.
16. Shintani, et al. The Hawaii Diet: Ad libitum high carbohydrate, low fat multi-cultural diet for the reduction of chronic disease risk factors: obesity, hypertension, hypercholesterolemia, and hyperglycemia. The Hawaii Medical Journal, 2001
In 2001, Dr. Shintani published results of a similar study to the study above. This time participants were fed a diet that included slightly more processed food, containing 12% of calories from fat. (17)
In addition to taro, sweet potatoes, fruit, beans, greens, and vegetables, the intervention diet also included some bread, pasta and tofu, and only a small amount of animal products were allowed per week.
Patients were allowed to eat in unlimited quantities, and were told to minimize their animal product intake to a total of 8 ounces per day of skinless chicken or fish.


The 21-day intervention resulted in the following:
Once again, patients who followed his dietary protocol increased their intake of carbohydrate-rich foods from starchy vegetables while decreasing or eliminating their need for oral medications and insulin.
17. McDougall, et al. Effects of 7 days on an ad libitum low-fat vegan diet: the McDougall Program cohort. The Nutrition Journal, 2014
In 2014, John McDougall, MD published a paper in which he analyzed the records of 1,615 patients who had attended his 10-day residential program. Researchers evaluated the changes that occurred after 7 days of following an ad libitum, low-fat, plant-based, whole-food diet containing less than 10% of calories from fat.(18)
Dr. McDougall is well known for advocating a starch-based diet including processed foods like pancakes, pasta, and bread, but focusing on eating starchy vegetables like sweet potatoes, yams, rice, beans, peas, and lentils.

Similar to the work of Shintani and Anderson, patients were encouraged to eat as much food as they wanted. Meals were served as a buffet, and participants were encouraged to take seconds or thirds if they desired.
Even though most antihypertensive and antihyperglycemic medications were reduced or discontinued at baseline, in just 7 days, patients experienced the following improvements:
This study did not include a direct measure of insulin, but once again, patients who followed the low-fat dietary protocol increased their intake of carbohydrate-rich foods from starchy vegetables and decreased or eliminated their need for oral medications and insulin, suggesting that their responsiveness to insulin and glucose tolerance both increased as a result of this dietary change.
18. Wright, et al. The BROAD study: A randomised controlled trial using a whole food plant-based diet in the community for obesity, ischaemic heart disease or diabetes. Nutrition and Diabetes, 2017
In 2017, Dr. Wright published results from a randomized controlled trial including 65 patients, all of whom were either obese, overweight, were living with heart disease, type 2 diabetes, high blood pressure, or high cholesterol. (19)
The intervention group was fed an ad libitum plant-based diet, containing 7-15% of calories from fat. Patients were provided education about a whole-food, plant-based diet, and were taught how to eat to satiation and resist the temptation to constrain portion sizes.
Foods allowed in their plant-based intervention included whole grains, beans, peas, lentils, potatoes, pastas, non-starchy vegetables and fruits, and subjects were encouraged to eat as much as they desired.
The control group, on the other hand, was simply given standard medical care as usual, and were not given any specific dietary recommendations.

Following 6 months, those that were in the control group experienced the following:
After 6 months on a low-fat, plant-based, whole-food diet, those in the intervention group experienced:
Participants also reported increased quality of life, better self-efficacy with nutrition, and higher-self-esteem. There was no significant change in enjoyment or cost of food.
Improved Insulin Sensitivity in the Real World
The Mastering Diabetes Coaching Program has helped thousands of people around the world maximize their insulin sensitivity via low-fat, plant-based, whole-food nutrition, daily exercise, intermittent fasting, and medicinal plants.
Over the years, we are proud to have helped thousands of people transform their health from the inside out, reduce or eliminate their need for oral medication, reduce or eliminate their need for insulin, lose weight, gain energy, become more active, improve their digestion, and dramatically improve their cardiovascular health.
Click below to learn more about the success of a few of our members:
Christopher Hertel (T1D)
Over the course of 1 year, Chris experienced the following:
He discontinued 11 medications (and only uses insulin now), and no longer suffers from hypertension, high cholesterol, atherosclerosis, neuropathy, retinopathy, erectile dysfunction, or rheumatoid arthritis.
Click here to watch and listen to Chris' story
Jessica Stidham (T1D)
Jessica increased her carbohydrate intake from 20 to 325 grams per day, and decreased her insulin use from 37.5 to 25 units per day while losing 15 pounds. Today, she feels better than she has ever felt and has more energy than she could have ever expected–thanks to the power of the Mastering Diabetes Method.
Click here to watch and listen to Jessica’s story
Josh Turner (T1D)
Eating a conventional diabetes diet, Josh ate 50-75 grams of carbohydrate per day and injected 70-80 units of total insulin. His fasting blood glucose ranged from 200-300 and his A1c was consistently above 11.0%. He now eats 600-700 grams of carbohydrate per day and injects 20-30 units of total insulin. His most recent A1c was 5.6% and he's lost 80 pounds.
Click here to watch and listen to Josh’s story
Sanna Kilpelainen (T1D)
Eating a conventional diabetes diet, Sanna ate 25 grams of carbohydrate per day and injected 22 units of total insulin. Within 9 months, Sanna increased her carbohydrate intake to 200 grams per day, while decreasing her insulin dose to 11 units.
Click here to watch and listen to Sanna’s story
Lindsay Garcia (T1D)
Lindsay increased her carbohydrate intake from 175 to 500 grams per day and has cut her insulin use dramatically. In addition her A1c dropped from 7.1% to 5.8%, and she is more active than she’s ever been.
Click here to watch and listen to Lindsay’s story
Patricia Walters (T1.5D)
In the first 4 months following the Mastering Diabetes Method, Patricia lost more than 20 pounds. Following a ketogenic diet she ate 30-40 grams of carbohydrate per day using 35 units of insulin, and now she eats as many as 300 grams of carbohydrate per day using only 20 units of insulin.
Click here to watch and listen to Patricia’s story
Tami Cockrell (T2D)
Tami adopted a low-fat, plant-based, whole-food diet and reduced her fasting insulin level from 17.4 to 5.2 mIU/L while increasing her carbohydrate intake from 75 to 350 grams per day. In addition her HbA1c decreased from 7.1% to 5.3% and she has lost more than 38 pounds.
Click here to watch and listen to Tami’s story
Heather Brock (T2D)
Heather Brock had an A1c of 9.2% while using diabetes medications Xigduo (two medications in one) at 1000mg twice daily, and Trulicity at 75mg once per week, Following the Mastering Diabetes Method for 3 months, her A1c reduced from 9.2 to 5.2% without the need for any diabetes medications.
Click here to watch and listen to Heather’s story
Raj Bhatt (T2D)
Raj used the Mastering Diabetes Method to reduce his A1c from 7.4% to 5.2% while decreasing his metformin dose from 2,000 mg per day to 0 mg per day. His fasting blood glucose decreased from 180 to 85 mg/dL, total cholesterol decreased from 215 mg/dL to 149 mg/dL. Additionally, Raj reversed fatty liver disease and lost 64 pounds in only 10 months.
Click here to watch and listen to Raj’s story
The EXACT Foods that Increase Insulin Sensitivity
A hallmark feature of the Mastering Diabetes Method is eating vibrant carbohydrate-rich meals comprised of foods like bananas, mangos, potatoes, butternut squash, lentils, beans, brown rice, farro, and quinoa.
At the center of the Mastering Diabetes Method lies foods that contain the highest nutrient density on the planet, containing an abundance of micronutrients including vitamins, minerals, fiber, water, antioxidants, and phytochemicals.
We encourage you to eat nutrient dense foods at every meal.

We have created a simple, easy-to-understand traffic light system that teaches you exactly what to eat and what to avoid in order to maximize your insulin sensitivity.
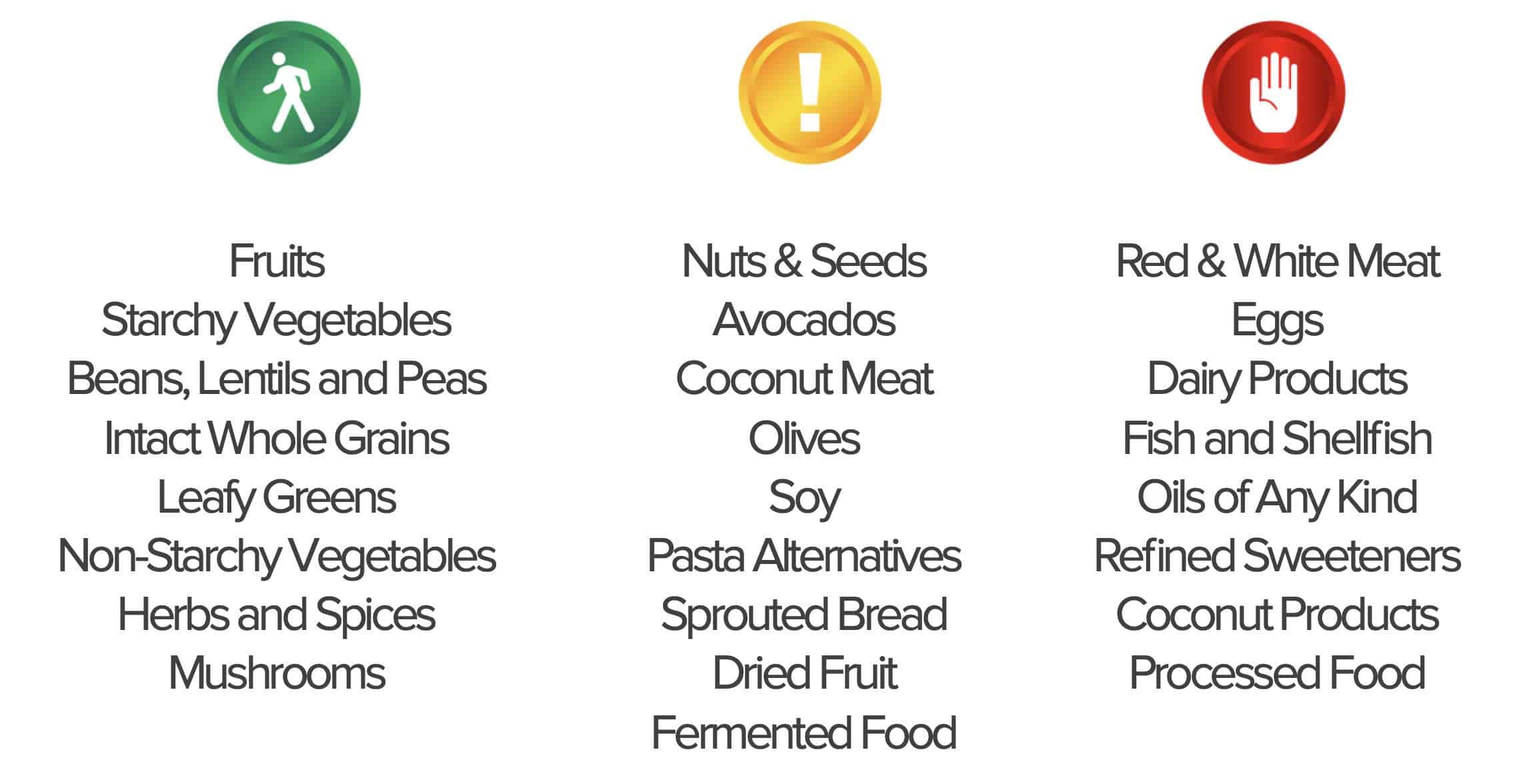
Green light foods include fruits, starchy vegetables, beans, lentils and peas, intact whole grains, leafy greens, non-starchy vegetables, herbs and spices, and mushrooms. For the vast majority of people, these foods can be eaten ad libitum with no restrictions or calorie counting.
At the top of the green light list are calorie dense foods including fruits, starchy vegetables, legumes, and intact whole grains. It’s important to eat calorie dense foods at every meal in order to remain satiated.
Below those foods are leafy greens, non-starchy vegetables, herbs and spices, and mushrooms. These foods are essential components of the Mastering Diabetes Method but must be eaten in combination with calorie dense foods in order to remain full.
A key point to remember about green light foods is that you can eat them in large quantities. They are naturally high in water content, fiber and low in fat. When you eat green light foods, your digestive system communicates with your brain to reduce your appetite quickly, making it challenging to overeat.
Yellow light foods are either high in their fat content or are highly processed, as compared with their green light counterparts. High-fat, whole-food plants include nuts, seeds, avocados, coconut meat, olives, and edamame. Processed plants in the yellow light category include pasta alternatives, sprouted bread, and dried fruit.
These foods are associated with many health benefits, but since they are naturally high in fat or more processed, it’s important to limit your intake of yellow light foods to truly maximize your insulin sensitivity.
Red light foods include red meat, white meat, eggs, dairy products, fish, shellfish, as well as oils of all kinds, refined sweeteners, coconut products, and highly processed snack foods (including vegan processed products).
Oils are one of the most refined, calorie dense foods on the planet and we strongly recommend reducing or eliminating your intake of all oil. The majority of vitamins, minerals, fiber, water, antioxidants, and phytochemicals have been lost in the refining process, which makes oil a food with low nutrient density and extremely high calorie density. The high calorie density can also inhibit weight loss.
For optimal insulin sensitivity, focus on eating the vast majority of your calories from the green light category, small amounts from the yellow light category, and as few as possible from the red light category.
A Final Note on Low-Carbohydrate Diets
Many research papers have compared low-fat and low-carbohydrate diets, to determine which approach is a more effective solution for diabetes and weight loss.
A recent article from a popular nutrition website provided a summary of 23 research papers comparing low-fat and low-carbohydrate diets, concluding that low-carbohydrate diets are more effective treatments for people living with diabetes.
Here’s the problem: Each of the 23 studies tested a “low-fat” containing between 17.8-36% calories from fat, even though a truly low-fat diet that maximizes insulin sensitivity contains a maximum of 15% calories from fat. None of these 23 studies tested a diet containing 15% or less calories from fat, and majority of their low-fat diets contained between 25-36% calories from fat.
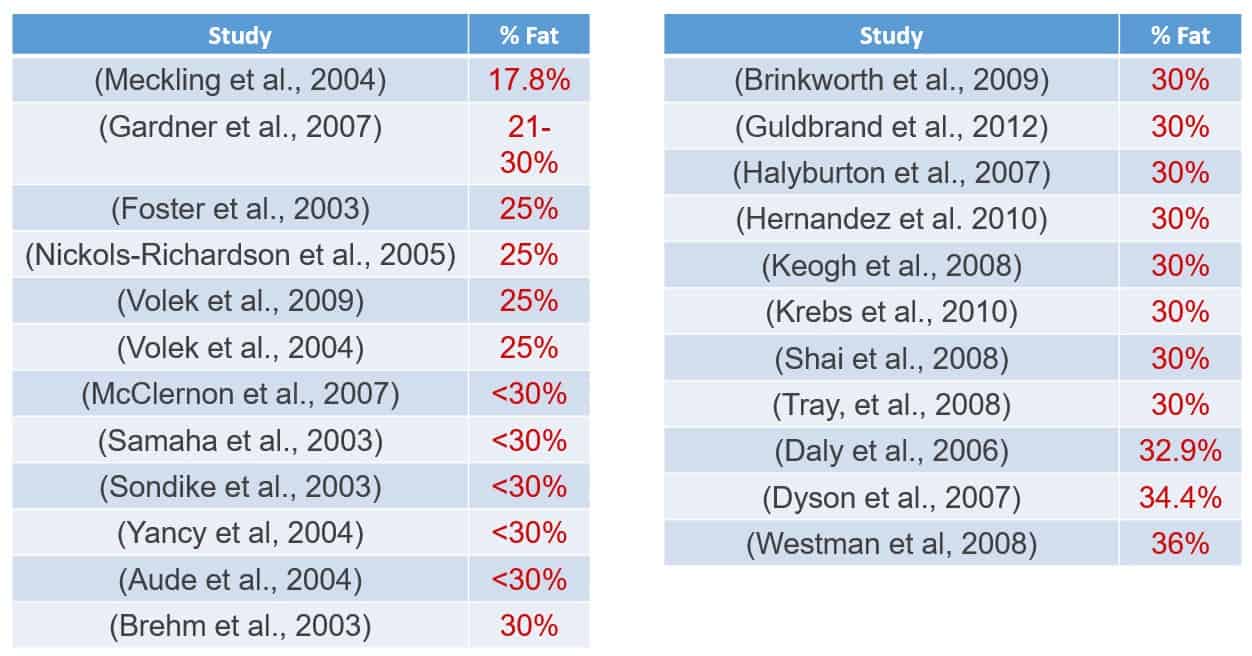
Based off of this analysis, the author concludes that low-carbohydrate diets are more effective weight loss tools, and promote better improvements in blood glucose and A1c than do low-fat diets.
The author states the following:
“These studies are scientific evidence, as good as it gets, that low-carb is much more effective than the low-fat diet that is still being recommended all over the world. It is time to retire the low-fat fad!”
This type of incomplete analysis makes the diabetes landscape incredibly confusing for people seeking true long-term health free of chronic disease. If you’re in this position, paying attention to small (but important) details like this could make the difference between years of ailing health and costly medication and a life free of chronic disease.
Take Home Message
For almost 100 years, scientists have described in grave detail how a high-fat diet increases insulin requirements by decreasing insulin action.
Each of the 18 papers described above are examples of rigorous research conducted in controlled settings that clearly demonstrate how insulin sensitivity and glucose tolerance increase when study subjects begin eating a low-fat, plant-based, whole-food diet.
If you haven’t tried it before, what are you waiting for?
References
Leave a Comment Below

