Meet Jessica.
Since the time she was diagnosed with type 1 diabetes in 1996, she has worked hard to follow a strict low-carb diet, in order to control her blood glucose to the best of her ability. Over the course of time however, she found that no matter how few carbohydrate-rich foods she ate, her blood glucose was quite challenging to control.
Low-Carb Diet
Searching for an easier approach to managing diabetes, Jessica adopted a low-carb diet in 2015. On her low-carb diet, she reduced her total carbohydrate intake to approximately 20 grams per day, hoping that it would give her tight blood glucose control.
Following this low-carb diet, Jessica's blood glucose was chronically elevated. Routinely, when she checked her blood glucose - either before or after a meal - she often saw values in the high 200s or low 300s.
Increasing Medication Requirements
To cope with increasing insulin requirements, Jessica’s doctor recommended starting 1000 mg of Metformin on a daily basis in addition to basal and bolus insulin. She found her doctor’s advice quite strange, given that Metformin is often prescribed for people with type 2 diabetes suffering from insulin resistance.
Despite this, she followed her doctor's advice and began taking 1000 mg of Metformin per day, desperate for any solution that would help improve her diabetes health.
Jessica found herself losing energy rapidly. From the time she woke up in the morning to the time she went to sleep, staying awake seemed increasingly difficult, and exercise was almost entirely out of the question.
Jessica knew something was terribly wrong, she just didn't know what to do to improve her health.
Enter Low-Fat, Plant-Based, Whole-Food Nutrition
While perusing on the Internet, Jessica stumbled across our website, and was intrigued by our low-fat, plant-based, whole-food approach to improving insulin sensitivity for people with type 1 diabetes.
She found our evidence-based approach to nutrition intriguing, and decided to enroll in our coaching program for type 1 diabetes.
In the first 3 weeks, Jessica transitioned from a low-carb diet to a low-fat diet, plant-based, whole-food lifestyle, by significantly increasing her intake of fruits and vegetables and reducing her intake of animal products.Initially, she was nervous that eating carbohydrate-rich foods would dramatically increase her insulin use, but despite this she started her program with an open mind, hopeful to experience positive change transitioning away from a low-carb diet.
After only 90 days on her program, Jessica’s carbohydrate intake had increased from approximately 20 grams per day to about 325 grams per day, significantly higher than she thought was possible for a person living with type 1 diabetes.
In that same 30 day period, she found that her blood glucose had become significantly more predictable, and in an effort to avoid hypoglycemia multiple times per day, she stopped using Metformin altogether.
Increased Insulin Sensitivity
Jessica remembers that the most surprising part of the first 3 months of her low-fat journey was how rapidly her basal and bolus insulin requirements fell.
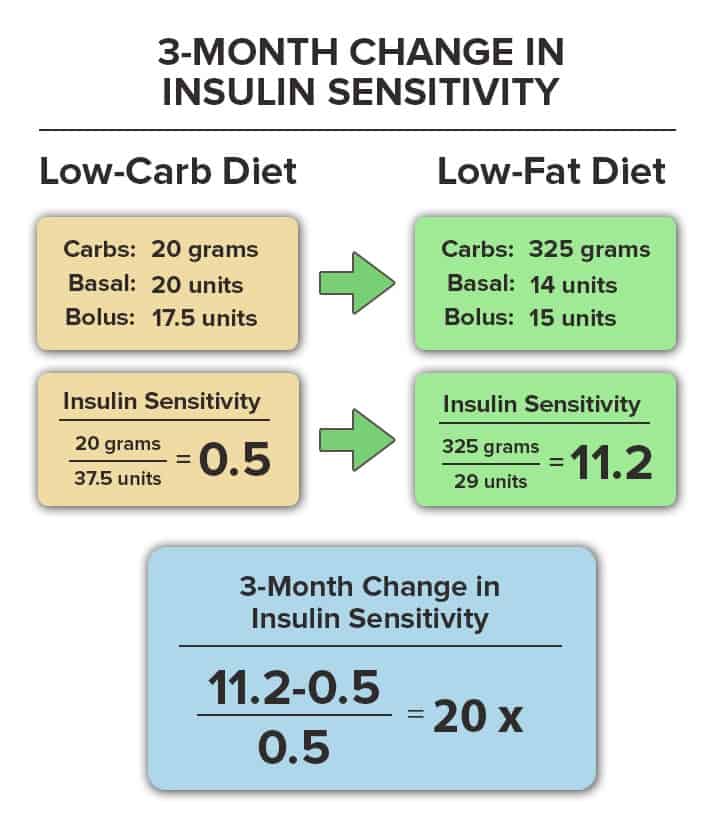
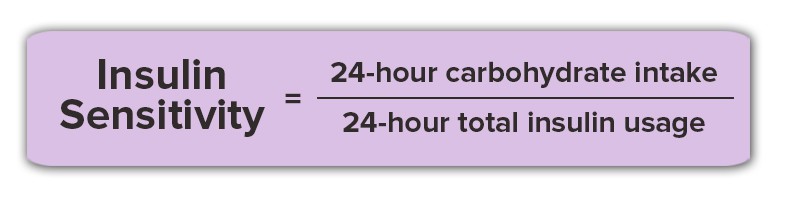
Following a low-carb diet, she averaged 20 units of basal insulin and 17.5 units of bolus insulin per day while eating about 20 grams of carbohydrate. Her baseline 24-hour insulin sensitivity was therefore 0.5 grams/unit.
By the end of the first 3 months, her basal insulin requirements had fallen to 14 units per day and her bolus insulin requirements had fallen to about 15 units per day, even though her carbohydrate intake had significantly increased to 325 grams per day. Her new 24-hour insulin sensitivity was therefore 11.2 grams/unit.

She had heard stories from other people in the group coaching program that her insulin sensitivity would likely increase following a low-fat, plant-based, whole-food lifestyle, but it wasn't until she experienced it for herself that she began to understand just how rapidly these changes took place.
Jessica returned to her active lifestyle, performing exercise whenever she wanted. She found that the more she continued to eat low-fat, plant-based, whole-foods, the more energy she gained, and the more weight she lost.
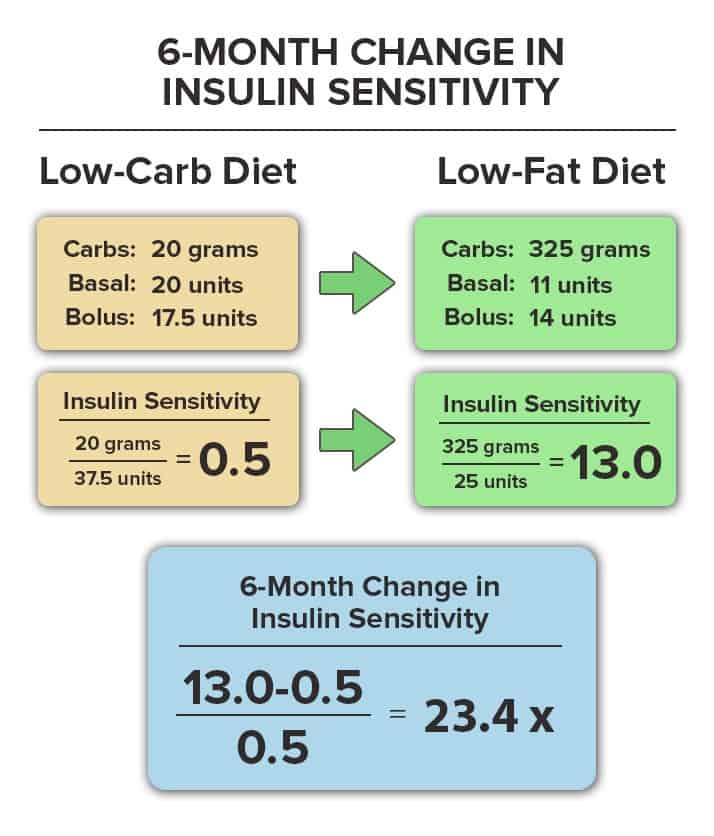
At the 6 month marker, Jessica had lost 15 pounds, and had improved her insulin sensitivity by more than 20x. Her basal insulin requirements had fallen to 11 units per day, and her bolus insulin requirements had fallen to approximately 14 units per day. Now, her 24-hour insulin sensitivity is 13.0 grams/unit.

Whole Body Health
Jessica now feels as though her total body health is completely within her control, and by continuing with a low-fat, plant-based, whole-food lifestyle, she is able to control her blood glucose, body weight, and energy levels simultaneously.
For the first time in her life with diabetes, she feels in full control of her health, and is able to do the things that she loves most: exercise, eat, and be merry.
We are extremely proud of the progress that Jessica has made over the past 6 months, and hope that her story to transition away from a low-carb diet inspires others living with type 1 diabetes about how they can achieve similar results.
If you’re interested in learning more about nutrition and fitness coaching for increasing insulin sensitivity, click here or click on the image below to see if you qualify.
Lower Your A1c and Fasting Blood Sugar... Guaranteed

Your results are guaranteed. Join more than 10,000 ecstatic members today
Personalized coaching puts you in immediate control of your diabetes health, helps you gain energy, improves your quality of life, and reduces or eliminates your meds.



