If you are living with diabetes, you've probably been told to minimize or eliminate your intake of fruit because "fruit is high in sugar."
And if this is the case, maybe you refrain from eating fruits because it causes your blood glucose to spike. Attracted by the smell, color and taste, you may find yourself asking a simple question:
"Should I avoid fruit in the long-term? And if so, will I ever be able to eat fruit again?”
It turns out that this ant-fruit message is a perfect example of pseudoscience at its best. A recent study published in PLOS medicine tracked the health of 512,891 Chinese men and women between the ages of 30 and 79 for an average of 7 years, in order to understand the effect that their diet had on their overall health (1).
We like these types of studies because they are:
- Performed in large numbers of people
- Performed over long periods of time
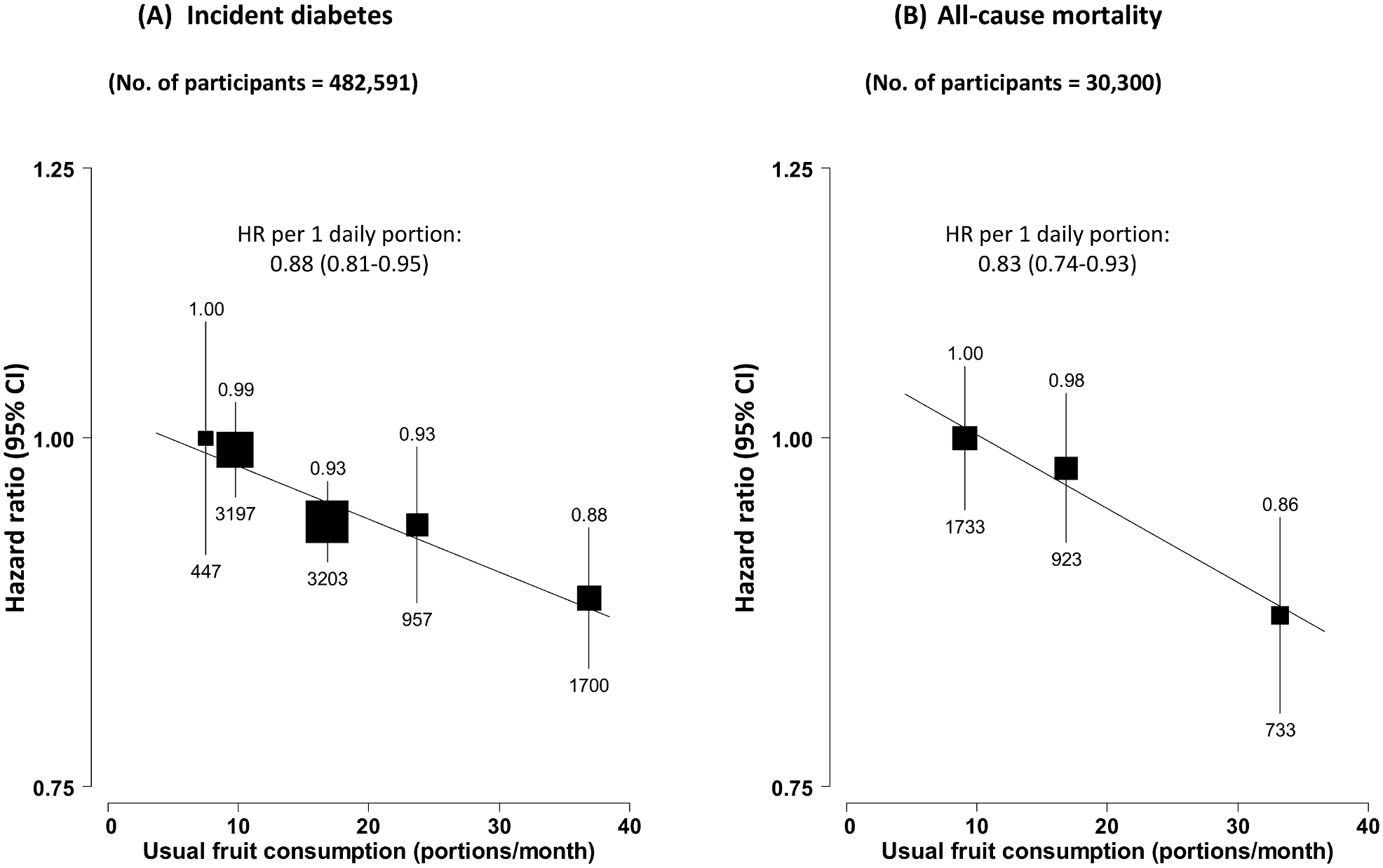
For those who did not have diabetes at the beginning of the study, those who had a higher fruit consumption were 12% less likely to develop diabetes, compared with those who ate zero pieces of fruit per day.
The researchers found a dose-response relationship, which means that the more frequently these nondiabetic individuals ate fruit, the lower the risk for developing diabetes.
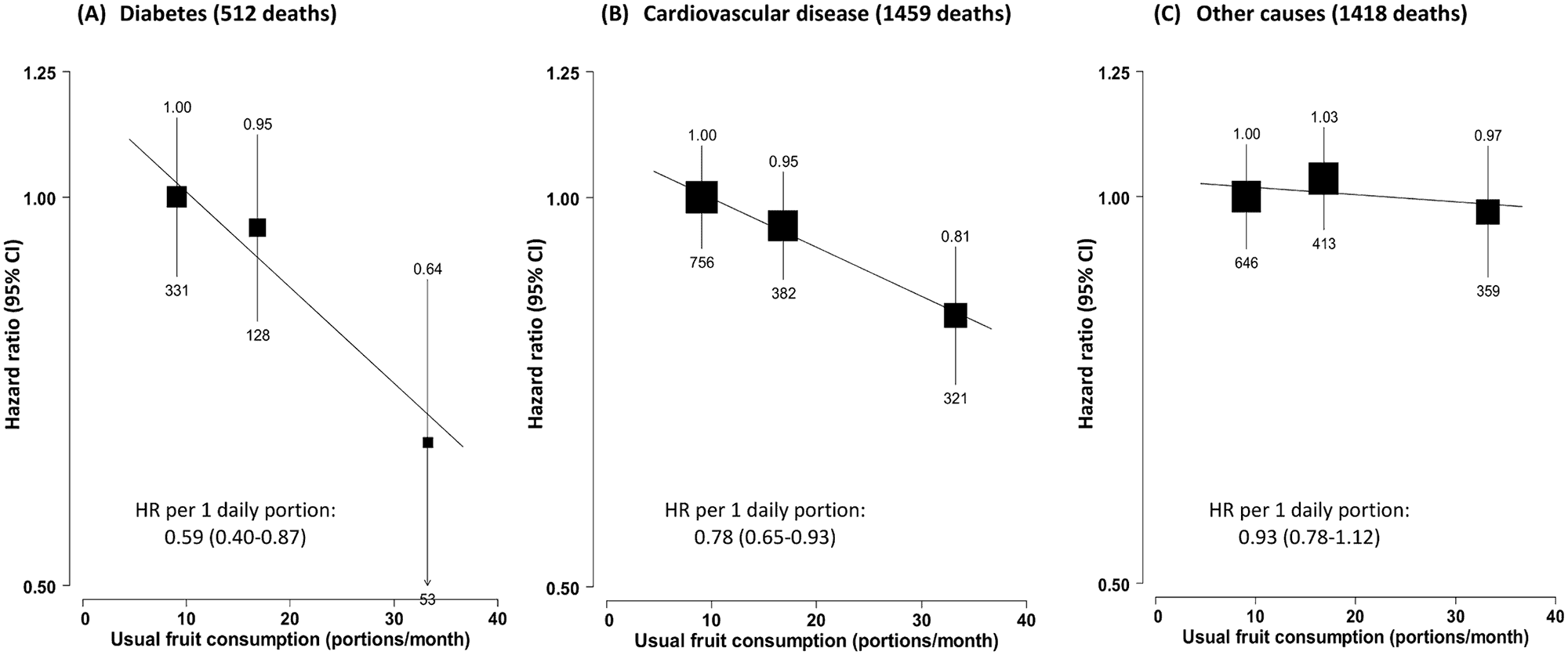
Amongst those living with diabetes at the beginning of the study, those who ate fruit 3 times per week reduced their risk of all-cause mortality (death from any cause) by 17%, compared with diabetic individuals who ate zero pieces of fruit per day.
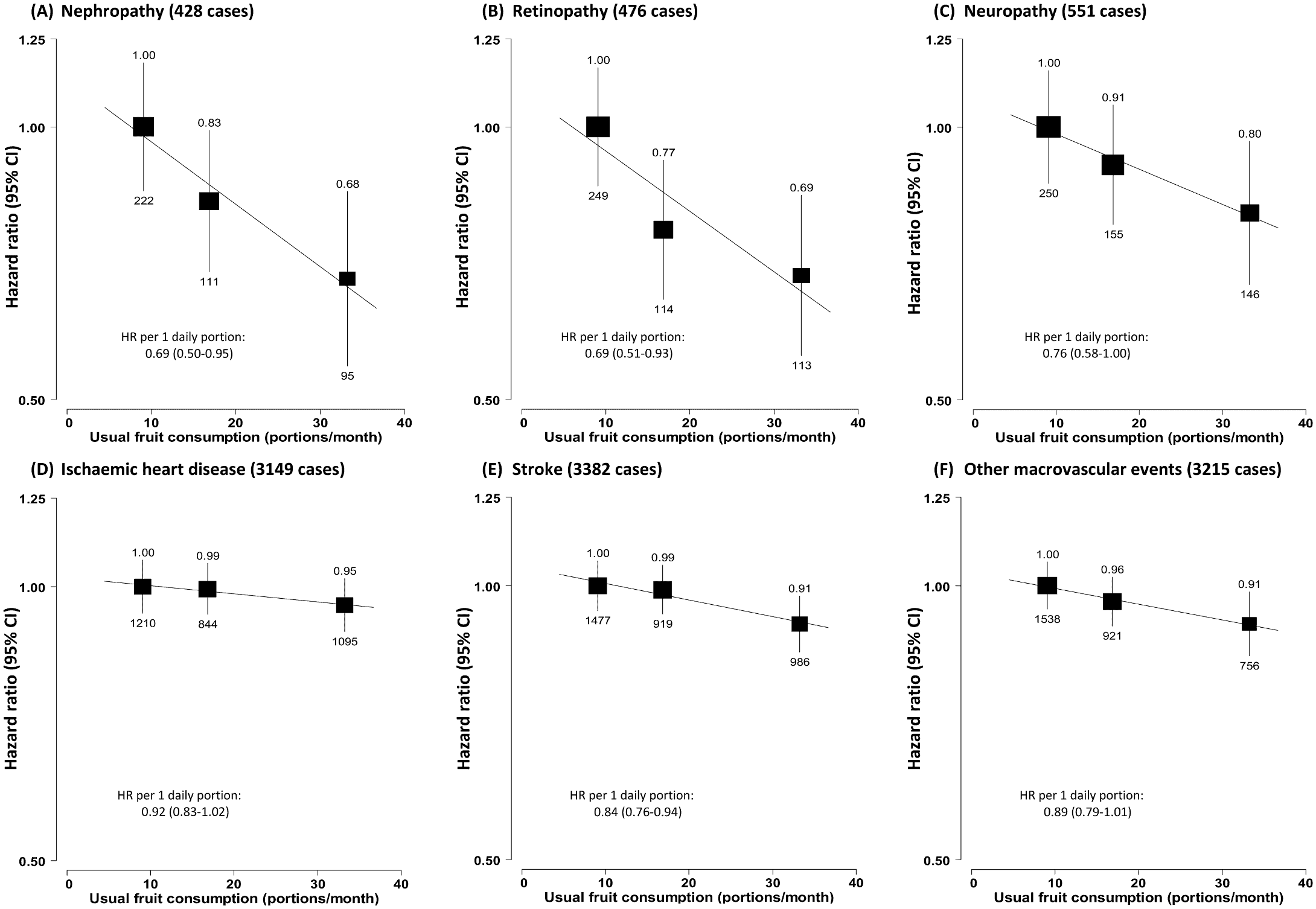
In addition, researchers uncovered that those who ate fresh fruit 3 days per week were 13-28% less likely to experience macrovascular complications (heart disease and stroke) and microvascular damage (kidney disease, retinopathy and neuropathy).
Even though this study was observational, the results of the study have profound implications for people living with diabetes around the world.
The lead researcher, Dr. Huaidong Du, believes that the reason why eating more fruit reduces the risk for diabetes and its complications is actually quite simple:
“The sugar in fruit is not the same as the sugar in manufactured foods and may be metabolized differently. And there are other nutrients in fruit that may benefit in other ways.” - Dr. Huaidong Du
Why is Fruit Good for You?
We are large advocates of eating fresh fruit on a daily basis. We are fortunate to get hands-on experience with people living with diabetes, and are able to witness the blood glucose lowering effect that a low-fat, plant-based, whole food diet has in those living with type 1 diabetes, prediabetes, type 2 diabetes and gestational diabetes.
We have taught thousands of people the exact method of increasing their fruit intake without causing blood glucose spikes, and have experienced similar results to those described in the research:
The more fruit our clients with diabetes eat, the more predictable their blood glucose becomes.
The more fruit our clients with diabetes eat, the more predictable their blood glucose becomes.
Just like Dr. Huaidong Du said, the carbohydrates found in fruits do not behave the same as refined sugars found in packaged and processed foods.Refined sugars like fructose and glucose can easily spike blood glucose values, which in turn increases your risk for diabetes, heart disease, cancer, obesity, and the metabolic syndrome (2-8).
Whole sugars found in fruits come prepackaged with water, antioxidants, fiber, vitamins and minerals (WAV-FM), which act as behind-the-scene players that protect against blood glucose spikes and actually increase your insulin sensitivity.
It’s true that the sugars in fruits can increase your blood glucose values, but the amount of insulin required to fully metabolize fruits is less than the amount of insulin required for the equivalent amount of refined glucose and fructose.
The reason for this is because your blood glucose is designed to rise and fall gradually in response to the foods you eat. Even in a non-diabetic individual, blood glucose variations between 80 mg/dL - 140 mg/dL occur on a daily basis. This normal variation in blood glucose is part of normal human physiology.
How Much Fruit is Too Much?
You may be asking yourself a simple question: if eating fruit is good for you, then how much fruit is too much? Is it possible to overeat on fruit, leading to worsening health, higher A1c values, increased blood pressure, increased risk for heart disease and weight gain?
In a study performed in 1971, researchers classified the effects of a “mainly fruit diet” to determine what happened to 17 people who ate 20 servings of fruit per day (9). On this regimen, people ate up to 200 grams of fructose per day, the equivalent of 8 cans of soda.
Researchers found that after 3 to 6 months on a mainly fruit diet, there were no adverse effects, and that body weight, blood pressure and insulin levels began trending down.
Following up on this research, in 2001 researchers tested the effect of 20 fruits per day on blood lipids and colon function, and found that within the first 2 weeks, total cholesterol dropped significantly (-40.6 mg/dL), as did LDL cholesterol (-37.9 mg/dL) (10). Although in this case it was a short-term study, they also reported zero adverse side effects of a diet packed with fruit.
Based on this evidence, it appears that there is no upper limit on the amount of fruit you can eat on a daily basis, and that any argument suggesting that fruit contains “too much sugar” is misinterpreting the scientific evidence.
High Carbohydrate Diets (Including Fruit) Have Been Studied for More than 85 Years
Believe it or not, scientists have been studying the effect of fruit on human health for more than 85 years, to understand whether fruit is safe for people with diabetes, but also to determine whether eating large quantities of both fruits and vegetables has any negative repercussions.
As early as 1930, Dr. Rabinowitch and colleagues at the Montreal General Hospital discovered that diets high in fat have detrimental effects on insulin sensitivity, and that diets low in fat improve insulin sensitivity (11,12,13,14).
Dr. Rabinowitch observed that patients who were switched from a low-carbohydrate diet to a high-carbohydrate diet containing large quantities of vegetables, fruits, grains, and beans reduced their need for insulin rapidly, both with and without calorie restriction.
They performed a randomized control trial (RCT) in patients with type 2 diabetes, and found that a high-carbohydrate diet significantly reduced insulin needs incredibly quickly. Dr. Rabinowitch wrote:
“Under-nutrition does not, however, explain the fact frequently noted that it is possible to change the diet of an individual from 50 grams of carbohydrate, 150 grams of fat, and 59 grams of protein to 250 grams of carbohydrate, 50 grams of fat and 75 grams of protein not only without the use of additional insulin but with less than required on the former diets; these diets are equivalent with respect to their caloric value.”
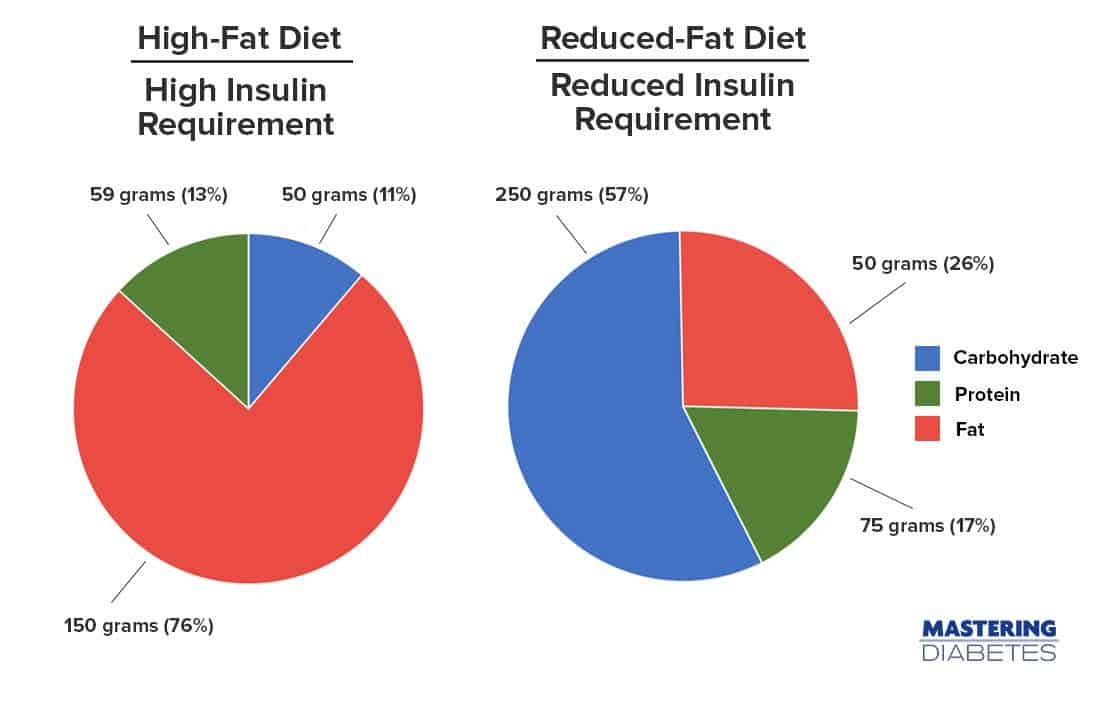
Note: in the graphs shown above, the percentage of fat in the reduced fat diet is approximately 26%, which is still higher than the 15% threshold that we recommend. Reducing total fat intake to below 15% results in even larger increases in insulin sensitivity.
Only 20 years later in the 1950’s, Dr. Walter Kempner at Duke University demonstrated that high fat diets not only caused insulin resistance and type 2 diabetes, but that patients could begin reversing long-standing diabetic retinopathy in a matter of days by eating a diet very high in fruit (15).
Dr. Kempner invented the rice-fruit diet, in which his patients were allowed to eat white rice, fruit, fruit juice, and added sugar - four foods that present day diabetes nutrition condemns almost entirely.

The rice-fruit diet was Dr. Kempner’s attempt at creating a no-salt, no-cholesterol diet containing almost pure carbohydrate. Dr. Kempner found that his rice-fruit diet reversed the following conditions:
- Malignant hypertension
- Heart disease
- Diabetic retinopathy
- Kidney failure
Take a moment and think about this carefully.
Conventional diabetes wisdom states that foods high in carbohydrate energy will exacerbate diabetes and increase the requirement for insulin and medication. By that rationale, Dr. Kempner’s rice-fruit diet should have resulted in metabolic disaster for his patients living with type 2 diabetes.
According to standard diabetes advice, the rice-fruit diet should have increased insulin requirements, caused unwanted weight gain, and promoted cardiovascular disease. But it didn’t. Why? Because whole carbohydrates are NOT the enemy for people with diabetes.
Given that the diets designed by Rabinowitch and Kempner were both low-fat and low-calorie diets, many questioned whether improvements in insulin sensitivity and diabetes were simply due to weight loss, and not to decreased dietary fat.
To separate these two variables, James W. Anderson and Kyleen Ward conducted a study in 1979 in which they enrolled 20 subjects who had been living with type 2 diabetes for more than 20 years (16).
The researchers fed participants a diet low in fat diet and high in carbohydrates but not restricted in calories, and monitored changes in insulin requirements and blood glucose over time.
In order to study the effects of diet alone, they made sure that subjects ate enough to prevent them from losing weight.
Some subjects complained of physical discomfort from eating so much food, but the protocol ensured that all subjects remained weight stable.
By doing this, they could then study how insulin requirements changed on a low-fat diet, independent of weight loss.
The results of this study were nothing short of remarkable. Insulin requirements plummeted by an average of 58% in the group that ate a low-fat diet, whereas insulin requirements did not change in those eating the conventional diabetes diet.
Ten out the 20 subjects were able to discontinue taking insulin altogether, and those who continued insulin therapy were able to reduce their dosages between 7-98%.
The most surprising result was that more than 50% of subjects were able to discontinue insulin completely after only 16 days on a low-fat diet, even having lived with type 2 diabetes for multiple years.
In addition, as a convenient side effect of a reduced intake of dietary fat, cholesterol levels dropped an average of 29%, from 206 mg/dL to 145 mg/dL.
Most importantly, all patients in this study were able to reduce or discontinue insulin therapy and reduce their cholesterol levels without any changes in body weight, clearly demonstrating that less dietary fat results in less insulin need.
Just imagine what would have happened to their cholesterol levels if they added the world's most powerful cholesterol-reducing food – amla (Indian gooseberries)...
Take Home Messages
If you remember a few things from this article, remember these points below:
- Carbohydrates are NOT the enemy for people with diabetes
- The more fruit you eat, the lower your risk for diabetes and its complications
- According to the evidence-based research, you cannot eat too much fruit
- To reduce your insulin requirement, simply drop your fat intake
References
References
Lower Your A1c and Fasting Blood Sugar... Guaranteed

Your results are guaranteed. Join more than 10,000 ecstatic members today
Personalized coaching puts you in immediate control of your diabetes health, helps you gain energy, improves your quality of life, and reduces or eliminates your meds.
Leave a Comment!
What are your thoughts on eating fruit living with diabetes? Tell us what you think about this research.



