
In the past few years, Continuous Glucose Monitoring (CGM) technology has transformed the ability of people to visualize their blood glucose profile in real-time. CGM technology is an exciting development for improving blood glucose control, and is gaining massive popularity.
A paper published in the American Diabetes Association journal Diabetes Spectrum last month (on which co-founder Cyrus Khambatta, PhD, is a coauthor) examines how CGM technology aids in maximizing blood glucose control (1).
What is CGM and Why Is It Valuable?
The most common method of monitoring blood glucose is the self-administered fingerstick, which is both inexpensive and relatively easy to learn.
However, fingersticks only provide information about blood glucose concentrations at a single point in time, requiring the user to “connect the dots” to understand their complete blood glucose patterns.
Moreover, fingersticks do not teach you the direction that your glucose is moving - up, down, or sideways - making it challenging to know when to eat, inject insulin, exercise, or take oral medication.
Another common test that people with diabetes are told to test frequently is hemoglobin A1c – a test that measures your average blood glucose control over the course of a 3 month period. The A1c provides you with a birds-eye view of your overall blood glucose control, but does not provide you insight into moment-by-moment blood glucose trends.
While fingersticks and A1c provide insight into your blood glucose patterns, neither of them allow you to observe your daily blood glucose trends.
Enter CGM technology.
There are two types of CGM systems currently available: professional CGM (also known as “masked” or “retrospective” CGM) and real-time CGM. Both types measure blood glucose levels through a sensor that is inserted into your skin, and both measure your blood glucose concentration every 5 minutes.
The article compares the three major FDA-approved professional CGM devices, made by Medtronic, Dexcom, and Abbot. Ultimately, all of them are excellent CGMs and the one you choose is up to personal preference.
The CGM creates PDF reports that both you and your physician can view to gain information about your blood glucose patterns over the course of time.
Being able to visualize your 24-hour blood glucose patterns is incredibly valuable. It allows you to see how different factors – such as exercise, high-fat or high-carbohydrate meals, and stress – affect your blood glucose throughout the day.
CGM Technology Provides Instant Feedback to Guide Your Lifestyle Changes
Diabetes is the most quantifiable chronic disease.
What this means is simple: if you regularly check your blood glucose, a CGM gives you instant feedback about how your lifestyle choices affect your blood glucose profile.
This is especially important if you transition to a low-fat, plant-based, whole-food diet. As your body becomes more insulin sensitive, the risk of hypoglycemia increases dramatically (and quickly), raising your chances of experiencing dangerous situations if you do not rapidly adjust your insulin doses or oral medications accordingly.
With CGM technology at your fingertips, both you and your doctor can visualize what’s happening to your blood glucose and make real-time changes to your medication use.
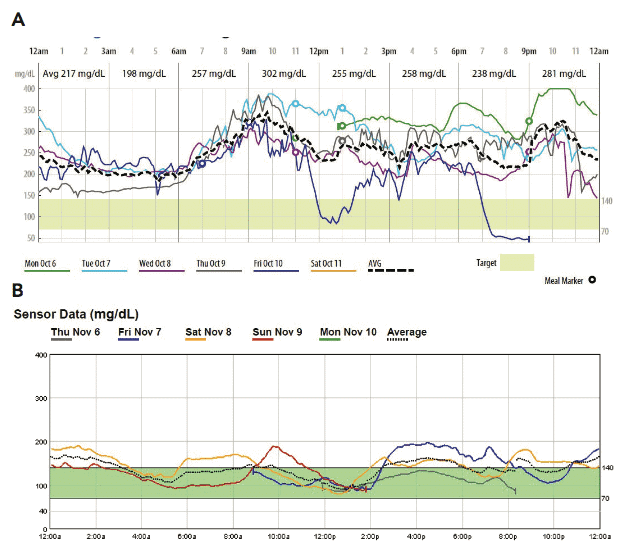
Figure 1: (A) Multiple days of CGM on a single patient prior to making lifestyle changes. Notice frequent blood glucose elevations during the day, and elevated average blood glucose. (B) After making simple lifestyle changes and adopting a low-fat, plant-based, whole-food lifestyle, CGM technology allows both the doctor and patient to visualize the same patient’s blood glucose profile and quantify glycemic improvements.
Without CGM technology, obtaining an accurate sense of the post-prandial (post-meal) blood glucose curve requires you to test your blood glucose multiple times over a 2-hour period following a meal, then manually graph this to determine your post-meal blood glucose “excursion.”
With CGM technology, all of this data is passively recorded for you. It gives you the feedback you need in order to assess how different foods or activities affect your blood glucose, and helps you to plan ahead to reverse insulin resistance, increase insulin sensitivity, and maintain precise blood glucose control.
As you adjust to low-fat, plant-based, whole-food nutrition, you likely will discover that high-fat meals cause your blood glucose to spike within the subsequent 6-12 hours, and that high-carbohydrate foods like bananas and potatoes improve your overall blood glucose control as long as your total fat intake remains between 10-15% of total calories (2-3).
Take Home Message
Using CGM technology is a great opportunity to visualize your blood glucose profile and see how it is affected by your lifestyle choices.
As shown in this article, either real-time or professional CGM technology can help you and your doctor make critical decisions quickly about how to adjust your medication needs to avoid hypoglycemia when transitioning to a low-fat, plant-based, whole-food diet.
Lower Your A1c and Fasting Blood Sugar... Guaranteed

Your results are guaranteed. Join more than 10,000 ecstatic members today
Personalized coaching puts you in immediate control of your diabetes health, helps you gain energy, improves your quality of life, and reduces or eliminates your meds.



