
What is Type 2 Diabetes?
Type 2 diabetes mellitus, is a chronic condition characterized by high blood glucose (hyperglycemia) and a wide range of ensuing side effects.
Type 2 diabetes, sometimes referred to as adult-onset diabetes, affects more than 31 million people in the U.S. alone, and is one of the fastest-growing chronic conditions in the world today.
Type 2 diabetes specifically manifests as a result of a condition called insulin resistance, which is caused by the accumulation of excess fat in cells that are not designed to store large quantities of fat.
In its early stages, type 2 diabetes is referred to as “non-insulin-dependent,” which is characterized by the following sequence of events:
In later stages, type 2 diabetes can become classified as “insulin-dependent,” resulting in the following events:
Fortunately, type 2 diabetes is reversible in the majority of cases via strategic diet and lifestyle changes that increase insulin sensitivity.
In this article, we’ll touch on the difference between type 1 and type 2 diabetes, as well as the specific symptoms to identify type 2 diabetes.
We’ll also explore the causes and risk factors of type 2 diabetes, as well as what you can do to prevent, treat, and reverse type 2 diabetes completely.
Type 1 vs Type 2 Diabetes: What’s The Difference?
In type 1 diabetes, insulin deficiency initially occurs as a result of an autoimmune condition in which your immune system mistakenly attacks the beta cells in your pancreas.
As a result, the population of beta cells in your pancreas is significantly compromised, resulting in insulin insufficiency and high blood glucose.
In non-insulin-dependent type 2 diabetes, the beta cells in your pancreas can produce enough insulin, but the insulin they produce is not powerful enough to overcome the amount of insulin resistance in your muscle and liver.
In the case of insulin-dependent type 2 diabetes, beta cells that have been overproducing insulin for months to years begin dying, resulting in a reduced population and insufficient insulin production.
Symptoms of Type 2 Diabetes
The core problem that all forms of diabetes have in common is hyperglycemia (high blood glucose), which can have a wide variety of side effects.
As a result, type 2 diabetes symptoms can include:
It’s important to note that these symptoms overlap with many other forms of diabetes, including type 1 diabetes, prediabetes, gestational diabetes, and type 1.5 diabetes.

What Causes Type 2 Diabetes?
Type 2 diabetes is caused by insulin resistance. Left untreated, insulin resistance progresses to prediabetes, and then eventually to type 2 diabetes.
One common misconception is that high blood pressure and a high body weight are causes of type 2 diabetes. However, this is not technically true.
The same diet and lifestyle issues that can cause type 2 diabetes can also contribute to high blood pressure and weight gain, but they are not always a direct cause.
Instead, high blood pressure and weight gain are considered comorbidities of type 2 diabetes.

Type 2 Diabetes Risk Factors: What To Look For
There are both controllable risk factors (factors that you can change) and uncontrollable risk factors (factors you cannot change) for type 2 diabetes.
Fortunately, the vast majority of type 2 diabetes risk factors are within your control, including:
The good news for you is that there is only one major factor of increased risk for type 2 diabetes that is technically out of your control:
However, despite the fact that certain genetics may leave you with a higher risk for type 2 diabetes, this condition is still extremely treatable and preventable through your diet and lifestyle in the majority of all cases.

Complications of Type 2 Diabetes
If left unmanaged, type 2 diabetes drastically increases your risk for other diseases, with one report finding that people with type 2 diabetes spent up to 3 times more on medical complications.
In addition, type 2 diabetes can cause a number of direct and indirect health problems. Direct complications from diabetes include:
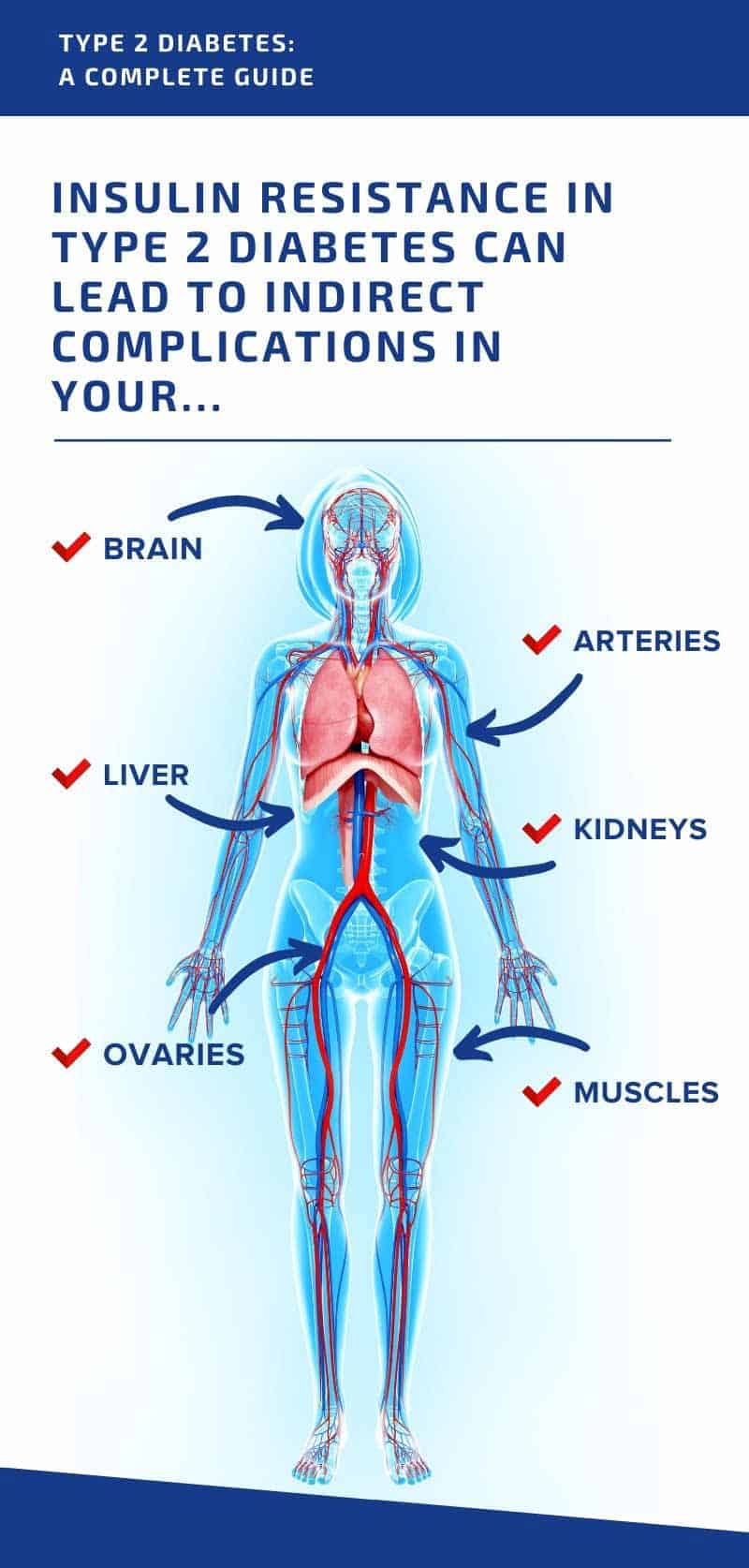
The underlying problem of insulin resistance in type 2 diabetes can also lead to indirect complications in your arteries, liver and muscles, kidneys, and ovaries, along with various neurological and brain disorders.
These diabetes complications include, but aren’t limited to:
Diagnosing Type 2 Diabetes
According to the American Diabetes Association, in order to be diagnosed with type 2 diabetes, one of the following must be true:
The majority of people live with some form of insulin resistance without recognizing the symptoms for years before being officially diagnosed with type 2 diabetes.
The A1c test is a blood test that provides information about your average blood glucose levels over the past 3 months.
An OGTT is a test of your ability to metabolize glucose in response to a glucose “challenge,” and works like this:
Identifying Type 2 vs Type 1 Diabetes
Type 2 diabetes is a vastly more common form of diabetes, especially when diagnosed in adults.
However, there are cases of adult-onset autoimmune diabetes, also called latent autoimmune diabetes in adults (LADA). This distinction can be found through c-peptide testing.
Fortunately, the Mastering Diabetes Method can treat type 1 diabetes, as well as prevent and reverse type 2 diabetes.
Prevention
There are three major areas that can drastically reduce your risk of developing type 2 diabetes:
These lifestyle changes — adjusting to a more healthy diet, adding more physical activity, and integrating intermittent fasting — are the key to both preventing and reversing type 2 diabetes.
Is Type 2 Diabetes Curable?
Yes, type 2 diabetes is curable.
The key to reversing type 2 diabetes is in reversing insulin resistance through strategic changes to your diet and activity levels.
If you are able to do that, you are able to effectively reverse type 2 diabetes (in the majority of cases).
Simply managing the symptoms of diabetes using oral medications or insulin does not reverse type 2 diabetes.
Pharmacological treatment does not dramatically increase your level of insulin sensitivity, which is required to completely reverse type 2 diabetes.
Below, we’ll touch on the three major areas that can help you reverse type 2 diabetes permanently.
How To Manage Type 2 Diabetes
The same dietary and lifestyle strategies that can help you prevent type 2 diabetes can also help you manage and reverse insulin resistance, return to normal blood glucose levels, and reverse type 2 diabetes.
These strategies are:
We’ll go into each of these areas in detail below.
Managing Type 2 Diabetes Through Diet
The most effective way to manage and reverse type 2 diabetes involves your diet.
Specifically, the research points to a low-fat, plant-based, whole-food diet that’s high in whole carbohydrates.
This way of eating results in dramatically increased insulin sensitivity, which in turn results in:
Compared to the Standard American Diet, these new guidelines can be quite a shift. Here are some helpful guidelines.
Red Light, Green Light, Yellow Light Foods
The guidelines for reversing type 2 diabetes are actually very simple, following a clear “green light, yellow light, red light,” categorization for foods.
“Green light” foods include all fruits (except avocado, durian, and dates), starchy and non-starchy vegetables, all legumes (except soybeans), intact whole grains (minimally processed), and herbs and spices.
Green light foods are foods that you can eat as much as you want, as these are unrefined whole foods low in fat with a high nutrient density that have been demonstrated to reverse insulin resistance.
“Yellow light” foods include whole grain or bean pastas, whole grain cereals, refined grains, whole grain bread and tortillas, avocados, nuts, seeds, coconut meat, soybeans, and soy products.
Yellow light foods are foods okay to include in small quantities, because they are slightly processed or have higher fat content. They shouldn’t be daily staples, but are still considered a “healthy” choice.
“Red light” foods include all red meats, all white meats, all seafood, eggs, dairy products, refined oils, and refined sugars (simple carbohydrates).
Red light foods are foods that we recommend removing from your cabinet, your fridge, and your plate.
These foods are documented by evidence-based research to cause insulin resistance, increase your blood glucose (fasting and post-meal), and promote chronic diseases in individuals with type 2 diabetes.
If you’d like to learn more about the low-fat, plant-based, whole-food diet, and how you can use it to reverse insulin resistance, you can check our comprehensive guide to reversing insulin resistance with your diet.
You can also read this article on high-carbohydrate foods proven to reverse insulin resistance for more details of exactly what to eat.
Managing Type 2 Diabetes Through Intermittent Fasting

Another powerful strategy to reverse type 2 diabetes involves intermittent fasting.
Intermittent fasting is a dietary strategy where periods of food consumption (‘eating windows’) alternate with fasting periods (‘fasting windows’).
Regular intermittent fasting has been shown to be a powerful tool for weight loss, reduced insulin resistance, better cardiovascular health, improved neurological activity, and improved liver health.
How it Works
The key to intermittent fasting is a process called autophagy, which is left over biological adaptation from when humans would need sustain themselves over extended periods without food.
While you’re fasting, cells in tissues throughout your body still need ATP, the cellular form of energy. However, during a fast, those same cells have little-to-no access to nutrients from food.
Rather than shut down, your cells generate ATP by oxidizing:
In essence, your body recycles old cells, proteins, and fats, which is actually very beneficial to your body when done in short and controlled periods.
Combined with a low-fat, plant-based, whole-food diet, intermittent fasting becomes an incredibly powerful tool for reversing type 2 diabetes.
Making it Happen
There are multiple methods of intermittent fasting -- the 16:8 method, the 24-hour method, the 5:2 method – and all are designed to allow for intentional, long periods between meals, specifically designed to improve many aspects of your overall health.
If you’d like to learn more about this process, you can check out our comprehensive guide to intermittent fasting.
Managing Type 2 Diabetes Through Exercise
Exercise is the third incredibly powerful strategy for reversing insulin resistance in type 2 diabetes.
When you exercise, cells in your muscle increase their energy requirements, which in turn increases their glucose requirements.
When your cells increase their energy demands, excess triglyceride is burned inside muscle cells, which in turn increases their responsiveness to insulin.
How It Works
At its most basic level, increasing your daily level of physical activity places a strain on your muscle tissue, which then signals muscle cells to manufacture more mitochondria.
Even assuming your diet has not changed at all, this higher mitochondrial density draws on your excess fat reserves, which in turn increases insulin action.
Because daily movement is such a powerful insulin sensitizer, we can all but guarantee that increased exercise can do the following:
Making it Happen
For some advice on adding exercise to your routine and keeping it there, you can check out our article on the topic, as well as our NY Times Bestselling Book on the Mastering Diabetes Method.
For some advice on adding exercise to your routine and keeping it there, you can check out our article on the topic, as well as our NY Times Bestselling Book on the Mastering Diabetes Method.
Managing Type 2 Diabetes Using Medication
In addition to diet and lifestyle changes, type 2 diabetes can also require two more acute interventions: oral medications and insulin.
Diabetes Medications
Treatment for type 2 diabetes often centers around diabetes medications, which are prescribed to lower your blood glucose, independent of diet and exercise.
These oral medications fall into a few overarching categories:
Insulin Injections
Since type 2 diabetes is caused by insulin resistance, insulin injections merely supplement your body’s endogenous insulin production, helping to lower your blood glucose.
Insulin injections fall into two main categories:
Transitioning Away from Medications
Remember, treating the symptoms of type 2 diabetes with medication will not treat the underlying causes.
The only way to effectively reverse type 2 diabetes is to reverse the underlying insulin resistance, which will reduce, and ultimately reduce your biological need for medication.
Pharmaceutical medications can have many benefits. They may help to control your blood glucose, improve insulin secretion, reduce your blood pressure, reduce your cholesterol, and reduce pain in the short term.
But the intensive treatment of blood glucose with medications can have an extensive list of side effects, and a number of negative long-term effects, which include increased risk for heart failure, liver failure, kidney failure, stroke, and even death.
That’s why we recommend a dedicated, concerted effort through lifestyle and dietary changes. These changes are safe, increase your energy and overall health, and are a sustainable long-term solution.
Mastering Type 2 Diabetes | Get Support
The most important takeaway from this article is that type 2 diabetes can be entirely controlled or reversed by changes to your diet and lifestyle.
That’s right. You have the power and the ability to reverse type 2 diabetes.
However, in most cases, these diet and lifestyle changes can be significant shifts to your habits and routine, which can often seem daunting.
To help you make the transition, we have a comprehensive Mastering Diabetes Coaching Program, with expert diabetes educators who can help you every step along the way.
Or, if you prefer to change your lifestyle by yourself, then you can join the Do-It-Yourself Program, which has changed the lives of more than 2,500 people around the world.
Resources, recipes, guides, a vibrant community, small groups, one-on-one coaching — we have options to suit whatever your particular needs are.
Our goal at Mastering Diabetes is to help everyone with diabetes understand that they have the power to transform their lives, and to provide any help we can along the transition to managing and reversing this disease.
And always remember, the power is in YOUR hands!
Stop Guessing What to Eat
Get Delicious Recipes Sent to Your Inbox Every Week!

Discover the custom-designed Weekly Meal Plan that gives you clarity on what to eat and how to shop to simplify your journey to lower blood sugar, weight loss, and your best A1c









