Type 1 diabetes is a chronic condition that typically requires constant management and monitoring throughout your life. One of the key problems with this type of diabetes is the lack of beta cells -- caused by an autoimmune response -- which hampers your body's ability to produce insulin when you have elevated blood sugar levels.
While there are treatments available, such as insulin shots, is it possible for people living with type 1 diabetes to regenerate their own beta cells naturally? We'll discuss why it's not likely, and some alternative strategies to improve your health and lifestyle while living with type 1 diabetes!
Why Do We Want to Regenerate Beta Cells?
The Role of Beta Cells in the Body
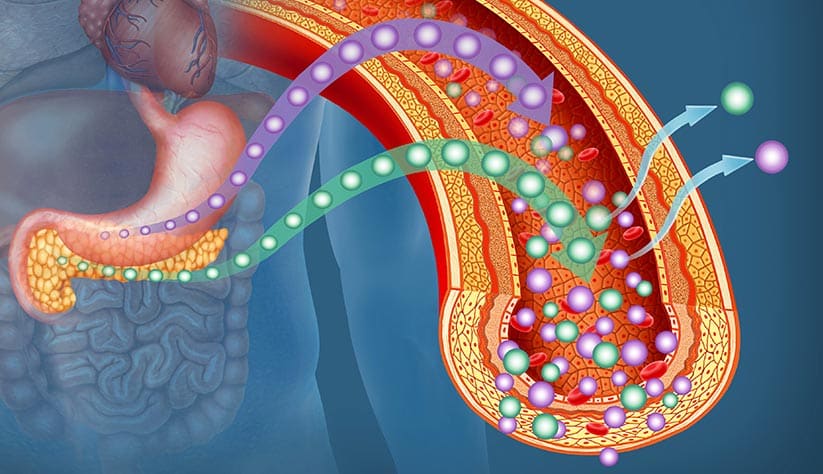
Beta cells are pancreatic cells that make up about 15% of the total number in your pancreas. In a healthy person, beta cells release insulin when your blood sugar levels rise -- which triggers muscle and fat tissue to absorb glucose from the bloodstream for energy or storage.
By itself, this is a normal response by your body to keep blood sugar levels within a healthy range.
What Can Happen to Them?
One of the most common conditions involving your body's beta cells is type 1 diabetes. In type 1 diabetes, beta cells are attacked by the body's own immune system, which causes a decrease in their ability to produce insulin.
It's currently unclear exactly why this happens, though there are some theories.
One of the most prominent is a sort of biological subterfuge in which harmful cells disguise themselves as cells in your body. Then, when your immune system detects these cells and tries to attack them, they also destroy the beneficial beta cells.
Another theory is that something in the environment triggers an autoimmune response against beta cells. Scientists are currently working to isolate what, if anything, causes this autoimmune response, to prevent it from happening.
The Results of Type 1 Diabetes and A Lack of Beta Cells
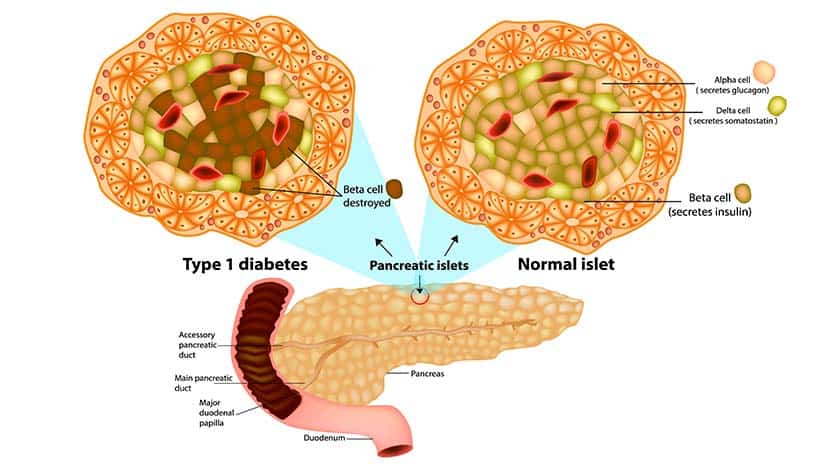
However, the result of type 1 diabetes is consistent -- your body becomes hardwired to attack beta cells, leaving you with very few (if any) in your pancreas, and leading to a lack of insulin production from the pancreas.
So when your blood sugar levels rise, your body cannot produce insulin to bring them back down.
As a result, you have high blood sugar levels -- known as hyperglycemia, which can cause long-term damage throughout your body if not properly controlled through medication or other means.
The Current State of Beta Cell Regeneration
History of Beta Cell Regeneration Research

There has been a concerted effort from the medical community to regenerate beta cells since the discovery of their role in type one diabetes.
Type 1 diabetes research dates back to the late 19th century when a young surgeon named Paul Langerhans first discovered these pancreatic cells and their association with type one diabetes.
However, it wasn't until more than 100 years later that researchers began to fully understand the mechanisms of this autoimmune response against beta cells in type one diabetics -- as well as potential ways to regenerate beta cells, reverse this autoimmune response, and regenerate functional beta cells in type one diabetics.
There are currently several research teams around the world working to regenerate these pancreatic cells naturally or using stem cell technology.
However, there are some roadblocks that have made progress slow for researchers looking into regenerating beta cells -- namely the difficulty in identifying the cells that regenerate beta cells naturally, as well as determining the role of these regenerated beta cells in a healthy pancreas.
After all, if you no longer have enough beta cells to produce insulin -- or they're being attacked by your body's own immune system -- then obviously that would be a good option for treatment!
Modern Advancements
However, despite significant progress over the last few decades, there has been little in the way of concrete results.
One key issue is that once beta cells are destroyed, they're gone for good -- there's no regenerating them like you can regenerate skin or other types of tissue after an injury.
However, researchers have found some potential ways to regenerate beta cells within people who already have type one diabetes.
For example, one study found that by injecting a type of stem cell directly into the pancreas, insulin production increased in patients with diabetes. While this research is still ongoing -- and has yet to be tried extensively on humans -- it's showing some promise.
Struggles Moving to Human Testing
One of the most difficult problems in this search for a solution is that research has focused on rodents for the most part.
While mice are an important model organism to study -- especially when it comes to genetics, development, and cancer suppressors like p53 -- there's a lot of variation between human biology and rodent biology that makes translating results from animal studies to humans very difficult.
In fact, many proofs-of-concept in animal studies fail to translate well when tested on humans.
For example, a widely cited proof of concept for regenerating beta cells from human embryonic stem cells was published back in 2002 by Douglas Melton and colleagues at Harvard University -- yet it took another 13 years until the results were successfully replicated in a clinical trial.
So while the research is promising, it's going to take some time before any practical treatment can be developed from these studies.
Clinical Trials
That doesn't mean that there's no hope!
In fact, onel trial is using a similar approach to regenerate beta cells as the Harvard study above.
Specifically, this research team injected human embryonic stem cell derivatives directly into diabetic mice and found that their blood sugar levels were reduced -- even without immunosuppressive drugs! The treatment was also seen to regenerate both pancreatic beta cells and insulin-producing cells in human patients!
These results are promising, but it's important to keep in mind that this is still only a proof of concept -- and even if successful, these treatments may not be suitable for humans.
However, continued research into regenerating pancreatic beta cells naturally or using stem cell technology will hopefully provide some answers for people affected by type one diabetes.
The Central Problem: Autoimmune Condition Still Exists
Regeneration Doesn't Work If Your Immune System Still Attacks
One of the central problems with type 1 diabetes, is that once your immune system has 'flagged' your insulin-producing beta cells as a foreign invader, your immune system will attack it relentlessly.
This response is called autoimmune disease, where the immune system turns against your own body's cells, and its an unfortunate byproduct of a very beneficial process of your immune system.
When your immune system identifies a foreign invader, like a virus or bacteria that can make you sick, it flags the cells as targets for destruction.
This is why your body gets rid of these invaders -- because they're clearly not supposed to be there!
This is how vaccines and adaptive immunity work. Your body is constantly learning about pathogens so that it can better defend itself in the future.
However, this response has a side effect: when your immune system flags certain cells as foreign invaders -- like beta cells for example -- then you have an autoimmune disease where these otherwise normal and healthy parts of your body are attacked by the immune system!
So even if you regenerate insulin-producing beta cells naturally or using stem cell technology -- like in the Harvard study above -- it may not be enough to overcome this autoimmunity process.
This is why many researchers are focusing on preventing type one diabetes before it ever occurs.
Is There Hope?
That's not to say that hope isn't on the horizon!
As stated in the introduction, there are several clinical trials currently testing different approaches for regenerating beta cells naturally. This means using stem cell technology or perhaps even gene therapies so your body can regenerate its own insulin-producing beta cells instead of relying on external sources, like insulin injections or pancreatic transplants.
On the plus side, many of these clinical trials are being tested on humans -- so if successful they can be used off-the-shelf rather than requiring custom development for every patient!
The research is promising and may provide some answers to people suffering from type one diabetes.
However, the problem of autoimmunity remains and is a bit more difficult. Currently, there's unfortunately little progress being made on how to prevent or reverse autoimmunity, so the best thing to do is try to prevent type one diabetes from occurring in the first place.
However, even if you've got type 1 diabetes, there's still hope! Even if it might not be possible to reproduce or regenerate your insulin-producing beta cells, there are many other ways to control your blood sugar levels so that you can live a long, healthy life.
Challenges to Quality of Life with Type 1 Diabetes
This research is all incredibly compelling, but in the meantime there are still challenges to living with type one diabetes.
That's what we focus on here at Mastering Diabetes -- identifying these lifestyle challenges and helping people overcome them through a healthy lifestyle.
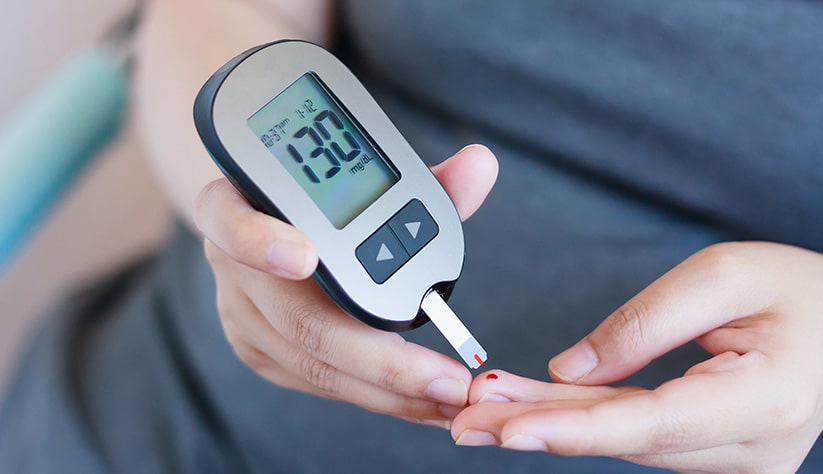
The Difficulty of Blood Glucose Control
Perhaps the biggest challenge to living with type one diabetes is managing your blood glucose levels.
This requires constant testing and insulin injections throughout the day, which can be extremely inconvenient at times -- especially if you're busy or traveling. It's a difficult health care regimen, and if you're not successful it can lead to dangerous consequences like diabetic ketoacidosis.
Then you add in a few complications, and it gets even more challenging.
For example, it's often very difficult to understand which foods will spike your blood glucose, and by how much.
Add in other challenges like daily stresses, having to exercise, and other health problems and your blood glucose management can become overwhelming.

Expensive Medication
Another complication for people with type 1 diabetes is having to take expensive medications.
Insulin is the most obvious example -- it's essential for living with type one diabetes, but often comes at a hefty price. Then there are other types of medication as well as routine doctor visits and lab tests that can add up!
In many cases, those costs might be covered by insurance companies or government health plans, but it's still a hassle and an added expense.
Constant Insulin Injections
This is all without mentioning the biggest challenge of having type 1 diabetes -- since you lack sufficient beta-cell mass to produce insulin for your body's needs, you need to constantly replace the role of your beta cells through insulin injections.
It's especially difficult when you're trying to eat, exercise or sleep -- these are the times where your body needs insulin most! So that increases the amount of time spent poking yourself with a needle instead of doing what you want in life.
A Major Challenge: Insulin Resistance
Up until now, we've discussed the challenges that come from having type one diabetes. After all, a lack of beta-cell mass and insulin-producing cells is major.
But what if your cells are also rejecting insulin? This condition, known as insulin resistance, can be an added challenge to living with type one diabetes.
Insulin resistance is the buildup of dietary fat cells which are not meant to store it. Cells try to burn this excess fat rather than the glucose/sugar in your bloodstream, meaning your body needs to send even more insulin to 'force' them to accept the blood glucose.
If you're living with type 1 diabetes, the presence of insulin resistance means even more medication and insulin, which can add up and turn into a headache quickly.
A Major Challenge: Lifestyle Causing Unpredictable Blood Glucose
There are a number of habits that can cause unpredictable blood glucose.
For example, eating processed foods or foods with added sugars can cause a significant spike in blood glucose. So can eating large meals, since they're harder for your body to process and absorb at once.
In some cases you might have planned for this with insulin injections -- but that's not always the case. Sometimes it just happens!
And then there are other lifestyle factors like stress or lack of sleep, which can have a significant impact on blood glucose levels.
As you can imagine, these unpredictable changes in blood sugar add to the challenges of living with type one diabetes.
The Mastering Diabetes Method
This is where the Mastering Diabetes Method comes in. The Mastering Diabetes Method is a step-by-step method that explains how to take control of your type one diabetes, reduce the amount of insulin or medication that you need to take, and more accurately control your blood glucose.
A Low-Fat, Plant-Based, Whole Food Diet

We recommend a low-fat, plant-based, whole-food diet for two reasons. The first is that this is the proven best diet to reduce insulin resistance so that your body responds quickly and more effectively to insulin.
The second is that plants and whole foods are high in natural fibers and complex nutrients, which can help you control your blood glucose levels by slowing the rate at which food is absorbed.
Daily Movement
Daily movement and exercise are the second major strategy of the Mastering Diabetes Method. Along with helping fight insulin resistance, consistent exercise actually helps train your body so that it burns energy more consistently, meaning your levels will be easier to predict.
Intermittent Fasting
The final strategy we recommend for people with type 1 diabetes is intermittent fasting. During intermittent periods of fasting, your body starts to burn excess dietary fat, which slowly fights any insulin resistance you might have. It also gives your body a break from food, and makes it easy to control your blood glucose!
Proven Results, Guaranteed
If you've got type 1 diabetes and insufficient beta-cell mass, that doesn't mean you should be hopeless! These insulin-producing cells can be supplemented with insulin from outside sources, and while beta cell regeneration research still has a long way to go, there are lifestyle changes you can make that will make a big difference.
That's what we focus on here at Mastering Diabetes, and we have the results to prove it. It's why we're so big on sharing the "A1c Miracle" that so many people have experienced.
Working with our method, and with the expert guidance of our coaches, thousands of people have already experienced transformations that have completely changed their lives while living with diabetes.
Will you?
Lower Your A1c and Fasting Blood Sugar... Guaranteed

Your results are guaranteed. Join more than 10,000 ecstatic members today
Personalized coaching puts you in immediate control of your diabetes health, helps you gain energy, improves your quality of life, and reduces or eliminates your meds.






