
What Is Time in Range?
Time in range (TIR) is a diabetes management strategy in which you measure what percentage of time your glucose levels are within your “target range,” compared to the amount of time in which they are either too high (hyperglycemia) or too low (hypoglycemia).
Time in range can be used for people living with all forms of diabetes (type 1, type 1.5, type 1, prediabetes and gestational diabetes) , and helps provide a “glucose profile,” a snapshot of how your blood glucose levels are throughout the day.
This can, in turn, help assess your risk for kidney disease, high blood pressure, and other complications.
In this article, we’ll explore the following:
Time in Range for Diabetes Management
Glycemic control, the process of properly managing your blood glucose, is a very important aspect of living with any form of diabetes. Hyperglycemia and hypoglycemia are two of the main challenges for people with diabetes, and controlling these fluctuations is crucial to reducing your risk for long-term complications like peripheral neuropathy, chronic kidney disease, fatty liver disease, high cholesterol, high blood pressure, and Alzheimer’s disease.
Most doctors use a standard measure called the hemoglobin A1c (HbA1c) to measure your blood average over a 90-120 day period.
The A1c measures the percentage of hemoglobin in your blood that has been glycosylated. This provides doctors with an indicator of how much glucose has attached to hemoglobin over the course of the lifetime of hemoglobin molecules (90-120 days).
The higher the percentage, the more glucose has attached to hemoglobin, and the higher your average blood glucose.
The A1c test can also be used to diagnose diabetes, based on the following guidelines:

Image courtesy of the American Diabetes Association: https://www.diabetes.org/a1c
If you’re living with autoimmune diabetes (type 1 or type 1.5), interpreting your A1c value can be slightly more challenging. We recommend maintaining an A1c value between 5.5%-6.5% with a low frequency of hypoglycemia (generally less than 4%).
While the A1c measurement is the standard of care for diabetes and certainly has its utility, a new form of measurement called time in range is quickly becoming a more valuable indicator of glycemic control.
Monitoring your time in range allows you to determine a few key things that the A1c measurement does not directly measure:
Using continuous glucose monitoring, it’s now possible to measure how long you’re in an acceptable blood glucose range, and provide a more detailed response to improve your overall health.
Time in Range CGM (Continuous Glucose Monitoring)
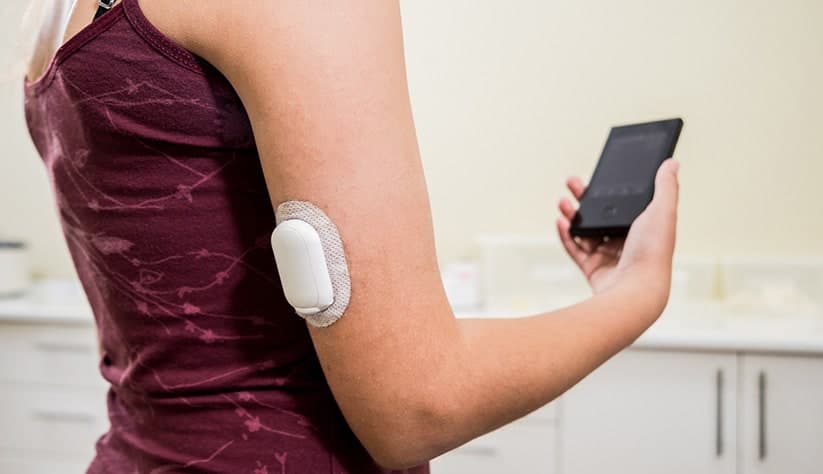
The most accurate way to measure time in range is through a process called continuous glucose monitoring.
Continuous glucose monitors (also known as CGMs) are disposable medical devices that measure your blood glucose levels throughout the day. CGMs communicate with your mobile phone and some insulin pumps have integrated CGM functionality which can help automate insulin delivery using real-time data.
Based on CGM data, you have virtually real-time measures of your blood glucose levels 24 hours a day, which allows you to monitor your blood glucose closely.
CGMs are most often recommended by healthcare providers when people experience difficulty controlling their blood glucose. This includes people living with type 1, type 1.5, or insulin-dependent type 2 diabetes, and also includes individuals with a history of complications including obesity or diabetic retinopathy.
Time in Range (TIR) vs HBA1c
Time in range is a more accurate and helpful measure of your blood glucose management for anyone with diabetes, and this is especially true if you have type 1, type 1.5, or insulin-dependent type 2 diabetes.
Your hemoglobin A1c is a measure of how much glucose has attached to hemoglobin molecules found in red blood cells.
While this is a helpful indication of your blood glucose trends in the long term, it can fall short if you’re trying to improve your real-time diabetes control and prevent both highs and lows.
Meals, exercise, and exogenous (external) insulin all create fluctuations in your blood glucose levels, which can lead to alternating hypoglycemia and hyperglycemia throughout the day if not managed correctly.
Your A1c value does not provide an accurate measurement of blood glucose fluctuations, it merely provides a measurement of your average blood glucose value over 90-120 days.
So in essence, your A1c is helpful, but not as informative as your time in range.
The largest landmark study supporting the use of TIR was the The Diabetes Control and Complications Trial (DCCT), which helped show that through careful, intensive management, it was possible to avoid or lessen many of the long term risks and complications of diabetes.
Time in Range Diabetes Guidelines

The time in range recommendations for each individual are different, though many leading groups of organizations like the American Diabetes Association (ADA) and other organizations have come to a recommended international consensus on a benchmark “target glucose range”.
This recommended blood glucose range is between 4.2 to 5.4 mmol/L while fasting, and up to 7.8 mmol/L when eating, and is based off of a number of diabetes clinical trials to determine which range puts you at the lowest risk for diabetes complications.
This is an excellent benchmark, but we recommend working closely with your doctor to determine the exact numbers you should be targeting.
How to Measure Time in Range
There are two ways to measure your time in range. The most accurate is through the use of a continuous glucose monitor (CGM), with Dexcom as the current industry leader of these devices.
The second is through the more old-fashioned use of fingersticks throughout the day. Though not as accurate in terms of up-to-the minute monitoring of your blood glucose, this strategy can actually still be very effective.
Taking fingersticks before and after meals, exercise, sleeping, or any other behaviors that can change the direction of your blood glucose trend can all help paint a reasonably accurate picture of how often you’re in range.
How to Improve Your Time in Range
Based on the decades of personal experience and hundreds of studies considered by the Mastering Diabetes Method, we’ve come up with five quick tips to help you improve your time in range.
However, our most important piece of advice for time in range overall is to follow the Mastering Diabetes Method, which includes eating a low-fat, plant-based, whole-food diet, making use of intermittent fasting, integrating daily exercise into your routine, and using decision trees on a regular basis.
These strategies are the key building blocks to reversing insulin resistance and getting control of your time in range, and without them, most of the other tips will not be very effective.
Focus on Insulin Timing
Pay attention to when you inject exogenous insulin. If you notice that you go out of range immediately after a meal, inject ten or fifteen minutes before. This can help level out those spikes and increase your time in range.
Optimize Your Basal Rate
Optimizing your basal rate can help keep you in range while you’re sleeping. Assuming you sleep for 8 hours a day, optimizing your basal rate of insulin can give you ⅓ of your day in range without any other changes to your diabetes management strategy.
Include Greens and Non Starchy Vegetables at Your Meals
These foods take longer to break down and process, which can help blunt any blood glucose spikes after a meal by extending the rate at which glucose enters your bloodstream. Which doesn't mean you should cut out starchy vegetables entirely -- just be aware of them.
Take a Walk After a Meal
Walking after a meal can also help curb blood glucose spikes by inciting your body to start burning energy at a slow, sustainable rate. There’s no need to exercise intensely, or get sweaty, but simple movement can help keep you in range.
Adjust Your Alarms
If you have a CGM device, adjust your alarms to beep before you go out of range (either high or low). This way, if your blood glucose is rising or falling, you’re able to adjust and make a change early, keeping you in range.
TIR and the Mastering Diabetes Method
TIR goals vary from person to person and depend on your age, health status, technology, and the type of diabetes you're living with.
In general, these are good time in range goals to aim for:
We have found that those who follow the Mastering Diabetes Method can achieve a time in range between 70% and 93% while not being obsessed with looking at their CGM device too frequently.
Your quality of life is very important to us, and we encourage you not to get lost in the details of trying to improve your TIR.
If you’d like help improving your TIR, consider joining our coaching program or getting started with the Weekly Meal Plan today. Both work incredibly well – so choose the one that’s right for you!
Stop Guessing What to Eat
Get Delicious Recipes Sent to Your Inbox Every Week!

Discover the custom-designed Weekly Meal Plan that gives you clarity on what to eat and how to shop to simplify your journey to lower blood sugar, weight loss, and your best A1c




