Can You Reverse Kidney Damage?
Your kidneys are a crucial part of your body’s waste elimination system. They help regulate excess liquid, remove waste products, maintain acid/base balance, and produce key hormones like erithroprotein (EPO), which signals the production of red blood cells.
As a result, kidney damage and kidney disease can have a number of different effects, causing severe metabolic distress.
Fortunately, your kidneys tend to be durable and capable of healing even from most late stage acute damage (though not all), and by adjusting your diet, improving your cardiovascular health, and avoiding high risk behaviors, you can often experience a full recovery.
What Causes Kidney Damage?

Think of your kidneys act as a natural blood filtration system. Twenty four hours a day, they’re filtering your blood for waste metabolites, which means that your diet can play a large role in their long-term health.
There are three main categories of risk factors for kidney injury:
We’ll touch on a few of the most common below.
Kidney Damage from High Blood Pressure
One of the most common causes for kidney damage is high blood pressure, which can occur as a result of a wide number of different risk factors (including some listed below).
Think of your kidneys as one of your body’s natural “filtration pumps”, which function ideally at normal blood pressure. Hypertension due to heart disease, high cholesterol, or any number of other conditions that can increase your blood pressure puts an excess strain on this filtration system.
Over a long time exposed to high blood pressure, the blood vessels in the kidneys can be damaged, worn down, or hardened, which limit the kidney’s ability to filter your blood and perform its vital functions.
Kidney Damage from Diabetes
Kidney damage from diabetes can occur in people with type 1 diabetes, type 2 diabetes, prediabetes, or any other condition that can cause hyperglycemia (also known as high blood glucose or high blood sugar).
When poorly managed, these conditions can lead to consistently high blood glucose levels, which in turn can damage the blood vessels and nephrons in your kidneys.
Kidney Damage from Alcohol
Your kidneys, along with your liver, are responsible for filtering harmful waste products in your blood, which includes alcohol. However, if exposed to these harmful products in excess quantities for a long period of time, even these filtration systems become damaged.
Combined with the fact that alcohol is a diuretic (which increases urination and can lead to your kidneys ‘drying out’ while dehydrated), and the fact that alcohol can lead to high blood pressure in the long term, you have a three-pronged risk for kidney disease.
Most experts say that increased risk kidney damage from alcohol begins to take place at an average of more than two drinks per day, and with heavy drinkers (more than 4 alcoholic drinks/day or 14 alcoholic drinks/week), this risk can be doubled.
Kidney Damage from Ibuprofen
Ibuprofen, as well as similar over-the-counter pain relievers like naproxen and aspirin, tend to be safe when taken in small doses.
However, the chemical process of these pain killers places a stress on your kidneys, and when taken in high doses or over an extended period of time can cause kidney damage.
We highly recommend following the safety information on these medications carefully, or with the guidance of a doctor.
Kidney Damage from COVID-19
One of the many complications that can result from COVID-19 is acute kidney injury (AKI), in which your kidneys suddenly take damage as a result of some medical condition or toxin.
Though the exact reason for this damage is still unclear due to COVID-19’s relative newness on the world stage, we recommend taking excessive caution if you have a history of kidney disease or one of the other conditions linked above.
Types of Kidney Damage
There are three types of kidney damage, progressing from temporary, acute conditions to end-stage kidney failure. We’ll touch on each below.
Acute Kidney Failure
The first type of kidney damage is acute kidney failure, sometimes referred to as acute renal failure. Despite its comparatively rapid onset compared to other forms of kidney damage, acute kidney failure usually occurs over the course of a few days, and coincides with other serious conditions.
If, for any reasons (usually related to limited or disrupted blood flow), your kidneys lose the ability to filter blood, the resulting lack of filtration causes electrolytes, fluids, and waste products to accumulate in your blood. This can damage any number of organs, and should be addressed by medical professionals immediately.
Left unattended, acute kidney failure can be fatal, so it’s important to immediately visit a doctor if you experience any of the symptoms, which include:
In most cases, however, acute kidney disease can be treated effectively, and patients can experience a full recovery.
Chronic Kidney Disease (Chronic Kidney Failure)
Chronic kidney disease, also known as CKD or early-stage kidney failure, affects 14% of the population and occurs when your kidneys are subject to chronic diseases like hypertension, high blood glucose, or alcohol and drug abuse for long periods of time.
Rather than a sudden build up of fluids and compounds, CKD is caused by the steady wearing down and damage of your kidneys, which reduces their ability to perform critical functions.
The symptoms of chronic kidney disease, which include weight loss, swollen extremities, tiredness, cramps, and urinary difficulties, can onset slowly because your kidneys can still function for a little while while damaged.
For this reason, it’s important to pay careful attention to your blood work and health, particularly if you have diabetes or high blood pressure. If caught early enough, it’s possible to recover from chronic kidney disease before symptoms worsen, or ultimately cause end-stage renal disease.
End-Stage Renal Disease
End-stage renal disease is total failure of your kidneys, which results from chronic kidney damage that has gone on for too long. With end-stage renal disease, your kidneys can no longer filter your blood, which causes rapid onset of a number of conditions.
End-stage renal disease cannot be reversed, and can only be cured via dialysis or a kidney transplant.
Kidney Disease Diagnosis

If you have any of the symptoms for any of the conditions above, you’ll work with a nephrologist (kidney doctor) to take both a urine test and some blood tests.
The first line of identification is measuring the levels of a waste product called creatinine in your body, which helps determine a biomarker called the glomerular filtration rate (GFR). If your GFR is too low, or there is a compound called urea present in your blood, you’ll need treatment for kidney disease.
A previous medical history can give your nephrologist an indication if your disease is chronic or acute. However, one of the ways they can determine for sure is a process called a biopsy, where they will collect a small sample of kidney tissue for testing via an extraction needle.
Kidney Damage Treatment Options
There are two levels of healthcare to treat kidney damage, depending on the severity of the kidney damage. In cases where damage is acute, or minimal, it’s possible to treat the complications of the disease with medication until lifestyle changes can be made.
However, in the case of severe or end-stage kidney damage, the only treatment options are dialysis and kidney transplant.
Before any treatment for kidney damage, we highly recommend talking to your trusted healthcare professional, as they can determine exactly the stage of your kidney damage and the best solution.
Treating Complications
The first line of treatment for early-stage kidney damage and acute kidney damage is to target the causes of the kidney damage (usually high blood pressure or accompanying high cholesterol), with medication until patients are able to use dietary changes to combat them.
These medications, like angiotensin-converting-enzyme inhibitors (ACE inhibitors), reduce the release of the signals to narrow blood vessels. Again, this is just a temporary fix, and should be accompanied by dietary and lifestyle changes to be fully effective.
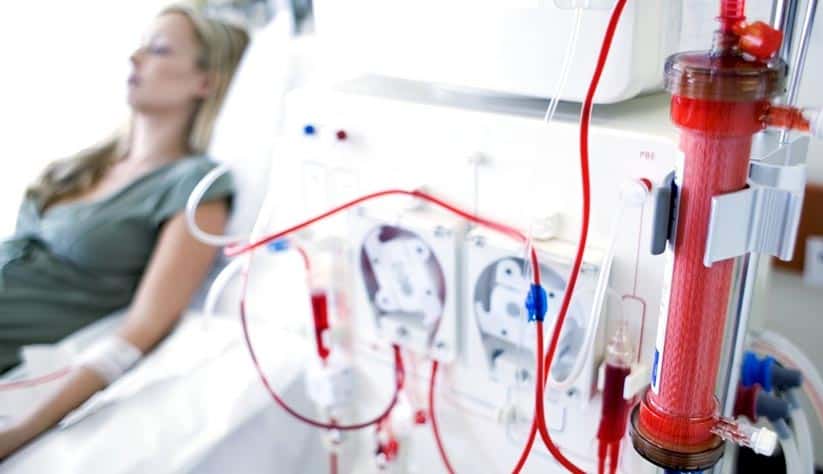
Dialysis
In the case of more extreme cases of kidney damage, dialysis may be required, which is the routine, manual flushing of your kidneys by an artificial machine. This replaces the natural removal of waste products by your kidneys, which can no longer provide this function.
Despite advances in recent years, dialysis is a treatment with a limited scope of success. Most indications show that patients on dialysis survive for 5-10 years, though these treatments have been prolonged for 20-30 years if adhered to correctly.
Kidney Transplant
One last resort for kidney failure, especially with end-stage renal disease is a kidney transplant, which is often used in tandem with dialysis. A kidney transplant involves finding a suitable donor with similar enough blood and biochemistry to allow for a transplant that the body will accept.
Though usually a more permanent solution than dialysis, the transplant process can be very difficult and complicated, often requiring long waits before a suitable donor can be found.
Reverse Kidney Damage Naturally

Despite the various medical advances made to help heal kidney damage, the most powerful way that you can improve your kidney health is with lifestyle changes, especially changes to your diet.
Ensuring that you eat enough potassium, phosphorous, calcium, and vitamin D (all found in various fruits and plants) is a good start, as these nutrients are fundamental to kidney health, but without controlling your high blood glucose and blood pressure, these changes are temporary.
That’s why we recommend a heavily plant-based diet that is high in fruits, vegetables, and whole grains if you’re suffering from high blood glucose and blood pressure. This diet is the first step to reverse insulin resistance, and can help vastly improve your cardiovascular health overall.
Eating potassium-rich foods can dramatically reduce your blood pressure, so include foods like tomatoes, potatoes, avocados, melons, oranges, bananas, nuts, seeds, dates, cruciferous vegetables into your diet on a daily basis.
One of the most effective ways to improve your kidney function is to reduce your intake of protein to approximately 0.8-1.0 g/kg body weight per day. Even though you may be tempted to eat a high-protein diet, understand that reducing your protein intake is a safe and highly effective way to reduce your risk of developing end stage renal disease (ESRD).
To accomplish this, we recommend eating a low-fat, plant-based, whole-food diet because it is an effective way to eat whole foods and target 0.8-1.0 g/kg protein intake per day.
One of the most underappreciated ways to optimize your kidney health is to eat fiber-rich foods. Fiber is a crucial nutrient that functions to improve the health of your microbiome, and people who eat between 50-100 grams of fiber per day experience the lowest rates of all-cause mortality.
To eat more fiber, simply eat the majority of your diet from these foods:
And in the process, do your best to reduce or eliminate your intake of:
For more information, check out the article we wrote about Sanna, who was able to reverse stage 3 kidney disease by changing her diet.
To learn more about how you can use a plant-based diet, along with other strategies, to improve your cardiovascular health, reduce your risk of kidney disease, and even reverse early-stage damage, you can explore our coaching program and resources.
Lower Your A1c and Fasting Blood Sugar... Guaranteed

Your results are guaranteed. Join more than 10,000 ecstatic members today
Personalized coaching puts you in immediate control of your diabetes health, helps you gain energy, improves your quality of life, and reduces or eliminates your meds.






