
What is Type 3 Diabetes?
Type 3 diabetes is a condition that is intricately linked with Alzheimer’s disease (sometimes referred to as Alzheimer’s dementia), which is the most common form of dementia in the US.
Alzheimer’s disease is a form of vascular dementia and is so pervasive in today’s world that it has become the third leading cause of mortality in both the United States and the United Kingdom.
Dementia is a broad term for multiple neurodegenerative diseases that typically affect older adults, causing cognitive impairment and a steady decline in brain function and mental acuity.
Scientists are actively studying the relationship between type 3 diabetes and Alzheimer's, and many have begun to think of them as the same disease.
By the numbers, dementia is arguably the most devastating disease of the 21st century:
The cost of dementia absolutely dwarfs other leading causes of mortality in the U.S., including heart disease ($219 billion) and cancer ($80.9 billion).
In this article, we'll explore the connection between insulin resistance, diabetes, dementia, and Alzheimer's disease and showcase the research that demonstrates that your brain health is determined mainly by your lifestyle – not by your genetics.
Why is Alzheimer’s Disease Considered Type 3 Diabetes?
The negative effects of diabetes come from insulin resistance, a buildup of fatty acids in cells that are not meant to store fats. This prevents cells from effectively processing glucose, leading to hyperglycemia (high blood glucose) and many other side effects.
For an in-depth understanding of insulin resistance and the metabolic dysfunction it causes, check out our definitive guide to insulin resistance.
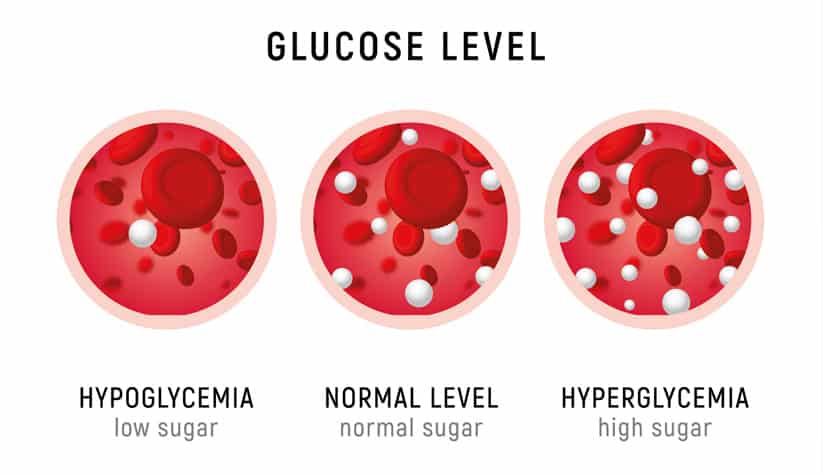
In the case of type 1 diabetes, insulin deficiency is primarily caused by the autoimmune attack of insulin producing beta cells in your pancreas, dramatically reducing your ability to manufacture and secrete insulin.
In the case of type 2 diabetes, oftentimes beta cells are capable of manufacturing and secreting sufficient insulin, but insulin resistance in your muscle and liver results in reduced insulin action in both tissues.
However, rather than manifesting early in life (as is often the case with type 1 diabetes) or in young to middle adulthood (as often happens with type 2 diabetes), type 3 diabetes typically affects adults 65 and older.
The other difference with type 3 diabetes is that it primarily manifests in damage to the brain, and can cause a dramatic decline in cognitive function.
Is Type 3 Diabetes The Same as Type 3C Diabetes Mellitus?
Even though type 3 diabetes and type 3c diabetes have similar names, these two forms of diabetes are actually quite different.
Type 3 diabetes is a form of diabetes that affects the brain and impairs cognitive function.
Type 3C diabetes mellitus is a form of diabetes that reduces insulin secretion, not from damage to the brain, but from damage to the pancreas caused mainly by chronic pancreatitis.
Alzheimer's Disease and Diabetes: A Scientific Look
Your brain is the most powerful and most important organ in your body. In fact, your brain is a fascinating tissue that:
As a result, your brain has a high demand for blood flow to bring a constant supply of oxygen and nutrients. However, it is also a very delicate organ, with millions of capillary blood vessels and very specific requirements for nutrients.
How Type 3 Diabetes Occurs
Over time, a brain that is constantly adjusting to suboptimal nutrition and impaired blood flow will accumulate slow and steady damage.
Your brain is very adaptable, so typically a condition like dementia doesn’t manifest when you’re young, and becomes more apparent as you age.
However, over the course of a lifetime, these risk factors can each contribute to cognitive decline and increase your risk for type 3 diabetes:
Once type 3 diabetes takes hold, this long term damage can increase, causing a wide variety of cognitive impairments like memory loss, cognitive decline, and more.
Type 3 diabetes is different from other forms of dementia like vascular dementia based on the rate of loss of cognitive function.
Vascular dementia is often caused by a stroke or other traumatic event, and results in an immediate decline in cognitive function, followed by a plateau. Type 3 diabetes manifests as a slow and steady decline in cognitive function.
An Inconvenient Truth About Type 3 Diabetes
Once type 3 diabetes manifests, there is currently no known cure for the disease. There are drugs that help with the symptoms and cognitive decline, but the underlying disease is not currently curable.
For this reason, the scientific community has very recently begun to focus on prevention, and how through a plant-based diet, exercise, proper sleep, cognitive activity, and management of stress it’s possible to reverse early signs of type 3 diabetes and prevent cognitive decline.

Symptoms of Type 3 Diabetes

The symptoms of type 3 diabetes are primarily related to cognitive function, and include:
One other early sign of type 3 diabetes is unexplained weight loss, which can occur both due to the same insulin resistance that often accompanies type 3 diabetes as well as behavioral changes.
How is Type 3 Diabetes Diagnosed?

There is currently no single agreed-upon method to diagnose type 3 diabetes.
In most cases, noticing one or multiple symptoms will result in a doctor running several cognitive tests. These tests, which test various aspects of cognition, are administered to determine your degree of cognitive impairment, and also eliminate other causes of impairment.
These cognitive tests tend to be frequently administered starting in early middle age, which can also help establish a baseline to show any decline in brain health.
On a physical level, there are two biomarkers that can help indicate the presence of type 3 diabetes: amyloid plaques, and neurofibrillary tangles.
Cognitive impairment combined with the presence of these biomarkers, along with other diabetes markers like high glucose levels, is a very strong indication of the presence of type 3 diabetes.
Can Type 3 Diabetes be Cured?
Type 3 diabetes currently has no known cure. Despite $2.8 billion of research funding expected in 2020, currently, 100% of medications have failed clinical trials.
Research continues for a cure for type 3 diabetes, but recent years have placed a focus heavily on more effective prevention and risk reduction of the disease.
One of the most effective prevention methods has involved identifying the highest risk factors for type 3 diabetes and working to counteract them.
Type 3 Diabetes Risk Factors
There’s a common misconception that type 3 diabetes is untreatable and unpreventable. However, this is not true.
There are less than 3% of cases in which type 3 diabetes is genetically determined, which means that no change in lifestyle will affect whether or not it manifests.
In the rest of cases, type 3 diabetes manifests as a result of genetic and lifestyle factors, where the effect of lifestyle vastly outweighs the effect of genetics.
Uncontrollable Risk Factors

There are several risk factors that you cannot control that can potentially affect your risk for developing type 3 diabetes, and all are related to genetics.
According to the research, the following factors can signal an increased risk for type 3 diabetes:
Controllable Risk Factors
On the other hand, there are a number of different, powerful risk factors for type 3 diabetes that are very controllable. They include, but are not limited to:
Type 3 Diabetes Prevention
Currently, there’s no way to reverse type 3 diabetes. However, as mentioned above, less than 3% of all type 3 diabetes cases are genetically determined.
The remaining 97% of cases can be affected by your lifestyle. The same risk factors above, when controlled, can drastically decrease your chance of developing type 3 diabetes, or at the very least delay its onset.
NEURO — Components of a Healthy Lifestyle
One helpful acronym developed by the experts at Team Sherzai is NEURO, which stands for Nutrition, Exercise, Unwind, Restorative Sleep, and Optimize Brain Function.
Each of these lifestyle areas has a strong neuroprotective effect and reduce the factors that can lead to type 3 diabetes, like high blood pressure, high blood glucose, and inflammation.
Nutrition

Proper nutrition is quickly rising to prominence as maybe the most powerful preventative step for type 3 diabetes, with one clear emphasis: low-fat, plant-based, whole-food nutrition.
Studies have shown that plant-based diets, and even the Mediterranean diet, which has a very low portion of meats, can slow the early stages of dementia, while high-fat diets clearly increase the risk of dementia in mice.
Fortunately, the guidelines for type 3 diabetes are exactly the same as for type 1 and type 2 diabetes, which you can find at our convenient guide here.
Exercise

Frequent exercise is another powerful preventative measure for type 3 diabetes, with research by the Alzheimer’s Research and Prevention Foundation showing that frequent exercise can lower your risk by up to 50%.
Their research also shows that frequent exercise can slow mental deterioration in individuals diagnosed with type 3 diabetes or other forms of dementia, which makes it a powerful habit to start and maintain.
We have a podcast talking about some easy ideas to get moving and stay active starting today.
Unwind

Though it can be hard to quantify, researchers agree that high levels of stress can increase the incidence of type 3 diabetes and worsen its neurodegenerative effect.
However, with stress as a continuously rising problem in the US, it’s more important than ever to pursue activities that lower stress.
Whether that’s socializing, time in the outdoors, mindfulness practices, or one of many other techniques, managing your stress is a health issue to take seriously.
Mild stress and challenges can actually help your brain. ‘Bad’ stress, however, is a chronic form of stress that can increase your risk for cognitive decline.
Restorative Sleep

Just as getting insufficient sleep can increase your risk for Alzheimer’s, taking care to get adequate sleep every night has a powerful neuroprotective effect.
Sleep has been proven to improve memory, metabolism, and mental sharpness, which have the added effect of improving other aspects of type 3 diabetes prevention.
For example, when you sleep enough you are less stressed, more likely to be active, and are more prepared to be mentally active — all factors that help prevent type 3 diabetes.
Optimize Brain Function

The last major area for type 3 diabetes prevention (and prevention of dementia as a whole) is in maintaining a high level of brain function.
Research shows that having a strong social network and community, living with purpose, and continuing to challenge your mind all have a strong neuroprotective effect while aging.
Finding this balance is different for everyone, but Team Sherzai has an excellent set of resources to get started.
How to Treat Type 3 Diabetes
As we mentioned above, you can’t reverse type 3 diabetes once it occurs. However, you can slow its progression, and help reduce the symptoms.
Treating Type 3 Diabetes with Lifestyle
The core lifestyle changes laid out in NEURO are the exact same lifestyle changes that can help treat and slow the progression of type 3 diabetes.
See above for an in-depth list, and accompanying resources.
Treating Type 3 Diabetes with Medication
In addition to lifestyle changes, there are several forms of medications and treatments that can help with the various symptoms of type 3 diabetes.
Metformin and other common diabetes medications can, in addition to dietary changes, help lower blood glucose and fight hyperglycemia.
There are also medications to help with memory, mood and behavior, and sleep changes, which can provide more acute treatment to specific issues faced by individuals with type 3 diabetes.
The Alzheimer’s Association has a thorough set of resources regarding treatment on their website.
Note: The extended-release version of Metformin has been recalled. For detailed information read the article linked above.
Wrap Up
Though type 3 diabetes still does not have a cure, the good news is that the vast majority of type 3 diabetes risk factors are entirely within your control.
By taking steps early to reduce your insulin resistance and improve your diabetes health, you can drastically reduce your risk for not only type 3 diabetes, but also type 2 diabetes and many other health conditions.
The key steps are simple — maintain proper nutrition, exercise frequently, unwind and control stress, restore with proper sleep, and optimize your mental activity — but making them happen can seem complicated.
That’s where our coaching program comes in. With a wealth of online resources and coaches with dozens of years managing insulin resistance and diabetes health, there’s a plan that works for everyone.
Lower Your A1c and Fasting Blood Sugar... Guaranteed

Your results are guaranteed. Join more than 10,000 ecstatic members today
Personalized coaching puts you in immediate control of your diabetes health, helps you gain energy, improves your quality of life, and reduces or eliminates your meds.






