Can Diabetic Nerve Damage Be Reversed?
One of the many challenges faced by people with diabetes is the risk of diabetic nerve damage, also known as diabetic neuropathy.
This painful condition is caused by chronically high blood glucose (high blood sugar), and often manifests in the legs and feet.
In this article, we’ll discuss the types, causes, and symptoms of diabetic nerve damage, and explore how changing your diet to treat, in tandem with medication, can significantly lower your blood glucose and help combat this condition.
What Is Diabetic Neuropathy?
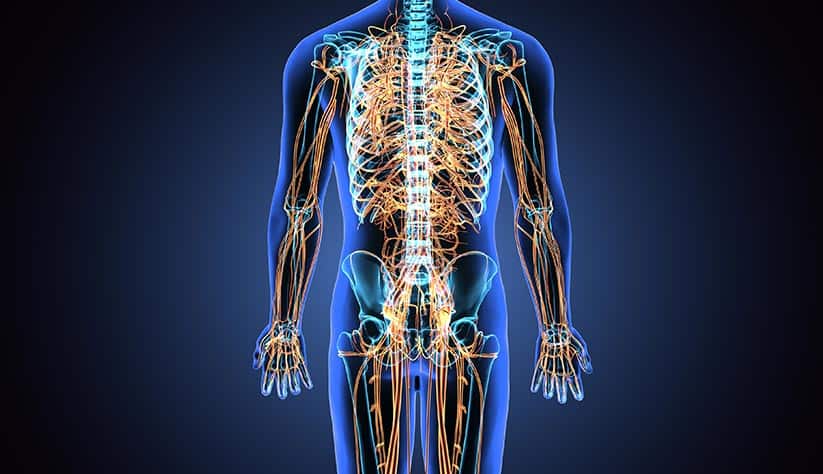
Diabetic neuropathy, more commonly known as diabetic nerve damage, is damage to your nerves that is caused by prolonged high blood glucose (high blood sugar) levels.
Though the exact cause of this condition is still being studied, researchers theorize that consistently high levels of blood glucose can damage both the blood vessels that supply nerves with blood, as well as the nerves themselves, interfering with their ability to send information.
Since diabetic neuropathy is tied to high blood glucose, this condition can occur in anyone with type 1 diabetes, type 2 diabetes, prediabetes, or any other condition that results in chronic hyperglycemia.
Risk Factors for Diabetic Neuropathy
The risk factors for diabetic neuropathy are similar to those for hyperglycemia. Some of these risk factors include:
Symptoms of Diabetic Neuropathy

We’ll touch on each of the symptoms below, and focus on which forms of diabetic neuropathy tend to cause them. However, it’s recommended that you get immediate medical help if:
Types of Diabetic Neuropathy and Their Complications

Peripheral Neuropathy
Diabetic peripheral neuropathy is the most common type of diabetic neuropathy, and often affects the hands, feet, and legs, with symptoms like:
Though these symptoms can range from mild to severe, peripheral neuropathy can be a precursor to more severe infections or slow-healing wounds. If caught early, peripheral neuropathy can usually be reversed, but in extreme cases of infection can require amputation.
Autonomic Neuropathy
Autonomic neuropathy is the second most common form of diabetic neuropathy, in which high blood glucose levels primarily affect organs monitored by the autonomic nervous system, which you do not consciously control.
Symptoms of autonomic neuropathy can be:
Proximal Neuropathy
Proximal neuropathy is a more rare form of diabetic neuropathy that tends to affect older individuals (50+) with type 2 diabetes. This form of nerve damage occurs in the hips, thighs, and buttocks, and can provide a number of symptoms including:
Unlike most forms of diabetic neuropathy, which require medication and a reversal of high blood glucose to subside, proximal neuropathy can often subside just by lowering your blood glucose.
Focal Neuropathy
Focal neuropathy is a form of diabetic neuropathy that occurs when a specific group of nerves (a focal point), experience nerve damage. Though this condition is not only reserved for individuals with diabetes (one common form is carpal tunnel syndrome), diabetes increases the risk for these conditions significantly.
Symptoms of focal neuropathy include:
Similar to proximal neuropathy, focal neuropathy is more likely to go away without medication, but can be helped significantly by getting your blood glucose under control.
Diabetic Nerve Damage Treatment Options
The most important aspect of combatting diabetic neuropathy is to control your blood glucose, to ensure that your symptoms and nerve damage do not get worse. From there, there are a number of different methods to help combat and alleviate the symptoms.
Blood Glucose Control
The most important aspect of treating diabetic nerve damage is reversing high blood glucose levels to ensure that no further diabetic nerve damage occurs. In early stages, this can be done through medications like metformin, but lifestyle changes are always preferable for long-term treatment.
And when it comes to lifestyle, the three fastest ways to lower your blood glucose are through changes to your diet (preferably a low-fat, plant-based, whole-food diet), daily movement, and intermittent fasting, which explore in further depth at each of those links.
Medication
There are a number of medications that can be used to treat the symptoms of diabetic neuropathy, which can include:
We recommend working with your doctor to understand the full scope of these medications and their side effects if you’re dealing with one of the four forms of neuropathy.
Personal Body Care
When dealing with pain, numbness, or weakness due to low blood flow, increased movement or massaging the affected areas have often been reported to provide some positive benefits.
Specifically with peripheral neuropathy, it’s important to be diligent with personal body care around your fingers, feet, and toenails, as limited feeling in these areas can lead you to miss out or fail to identify potential cuts, ingrown nails, or infections.
Hydrotherapy
Hydrotherapy refers to the use of hot and cold water to improve blood circulation, which in turn alleviates nerve damage. Hydrotherapy has been used for centuries to treat bloating and constipation, viral infections, and musculoskeletal injuries, and is a powerful tool for people with diabetes who experience nerve pain in their extremities.
Performing hydrotherapy requires immersing body parts that experience nerve damage (usually your hands and/or feet) in hot water for a specified period of time, followed by cold water for a specified period of time.
By alternating between hot and cold water for specific time periods, blood vessels contract and relax, which in turn regulates blood flow to the affected body parts. Nerves in the affected area often experience dramatic improvements within days or weeks of an active hydrotherapy regimen.
For more detailed information, listen to our podcast episode with Rich and Ronda Smith from the Black Hills Lifestyle Medicine Center who have performed hydrotherapy on thousands of clients with diabetes with overwhelming success.
So, Can You Reverse Diabetic Nerve Damage Naturally?

In certain cases, yes. In the cases of focal and proximal neuropathy, most nerve pain and weakness tends to subside after a few months or years if you take the steps needed to reduce your high blood glucose, like switching to a plant-based diet, which has consistently shown results.
However, there are some aspects of nerve damage that can’t be reversed, particularly complications associated with peripheral or autonomic neuropathy. This is one of the many reasons why it’s important to tackle high blood glucose and its most common underlying cause, insulin resistance, early.
If you’d like to learn more about our three best, evidence-based recommendations for lowering your overall blood glucose quickly — a plant-based diet high in whole carbohydrates, intermittent fasting, and daily movement — and get the best tips on implementing these changes, you can explore our coaching program.
We’ve helped show thousands of people the keys to reverse high blood glucose through their lifestyle, and master whatever form of diabetes they were struggling with.
Stop Guessing What to Eat
Get Delicious Recipes Sent to Your Inbox Every Week!

Discover the custom-designed Weekly Meal Plan that gives you clarity on what to eat and how to shop to simplify your journey to lower blood sugar, weight loss, and your best A1c