I was interviewed by Chef AJ, a Los Angeles chef with 40 years of experience eating a plant-based diet. In this video, we discuss the positive changes that eating a low-fat, plant-based, whole-food diet has on diabetes.
The Differences Between Type 1 and Type 2 Diabetes
There are three generally recognized types of diabetes: type 1, type 1.5 and type 2 diabetes. Each type involves a slightly different biological mechanism that regulates insulin production.
Type 1 diabetes, or insulin dependent diabetes mellitus, was originally classified as a juvenile disease that affected only young children [0:50]. In type 1 diabetes, pancreatic beta cells lose their ability to secrete insulin almost entirely [1:48]. An episode of diabetic ketoacidosis (DKA), a condition marked by excessive thirst, weight loss and low energy, often precedes diagnosis in individuals with type 1 diabetes.
Many people who develop type 1 diabetes tell a similar story, with the same collection of symptoms [2:01]. It is also common for many newly diagnosed individuals with type 1 diabetes to to have a blood glucose higher than 400 mg/dL (22.2 mmol/L) at the time of diagnosis.
Type 1.5 diabetes, known as Latent Autoimmune Disease in Adults (LADA), is similar to type 1 diabetes in that pancreatic beta cells lose their ability to secrete insulin over time.
The main difference between type 1 diabetes and type 1.5 diabetes is that type 1.5 diabetes progresses slowly, and those diagnosed often require only small amounts of insulin at first, then larger amounts of insulin over the course of many years.
Formerly called adult onset diabetes, type 2 diabetes usually results in a slightly different path to diagnosis; in this case, the body is no longer able to mask increasing amounts of insulin resistance [1:07]. Pancreatic beta cells generally still secrete insulin in those with type 2 diabetes, but their insulin output decreases over time as the beta cells are forced to overproduce insulin.
People diagnosed with type 2 diabetes typically experience weight gain before they are diagnosed, due to increasing insulin resistance. While type 2 diabetes was formerly classified as an “adult disease,” the number of children diagnosed with type 2 diabetes has significantly increased due to poor eating habits and reduced activity.
My Type 1 Diabetes Diagnosis
I was diagnosed in 2002 with type 1 diabetes at the age of 12 [1:54]. I experienced standard symptoms and recognized the signs quite early because my older brother was living with type 1 diabetes.
After living with diabetes for about 4 years, I began modifying my diet trying to achieve better health [6:20]. I began taking supplements, eating grass-fed beef, drinking raw milk, and cutting food additives out of my diet. Eventually, I ended up eating a Weston A Price diet and trying a Gabriel Cousens phase 1 diet [7:09].
In college, my diet changed dramatically. After reading a discussion on an online forum, I watched the movie Earthlings [8:08]. This movie served as an introduction into the world of plant-based nutrition, and drove me to learn as much as I could about eating a diet based entirely on plants.
What I Eat: Diabetes and Fruit
Over time, I experimented with various plant-based approaches, but the one that gave me the most profound results was a low-fat, whole-food, plant-based diet. While there is some latitude for different expressions of this type of diet, I have settled into deriving most of my calories from fruits and fresh vegetables [14:42].
The vast majority of the foods that I eat come from the farmer’s market and produce wholesalers [55:30]. My food is as fresh as possible, and is only processed by blending fruits and vegetables into a smoothie on occasion [16:40]. I recommend a plant-to-mouth approach for people with diabetes because preserving the fiber that binds the natural sugars in the foods helps to stabilize blood glucose [15:53].
A typical day of food for me involves grabbing perfectly ripened fruit off my 6-foot fruit storage shelf and throwing a few vegetables/greens with them in a bowl. For breakfast I may eat 3 to 4 mangos, a couple bananas, and half a papaya [19:41]. I eat 4 meals a day, and the proportion of vegetables per meal increase as the day progresses; the last meal of the day is usually a salad with fruit mixed in.
The sheer amount of fruit I eat may be surprising, but I emphasize the extreme importance of eating enough calories on a plant-based diet [19:08]. This is the #1 reason most people abandon eating a plant-based diet is because they are simply not eating enough calories.
What is Insulin Resistance and Why is it Important?
A low-fat plant-based diet addresses the basic complicating factor in the treatment of diabetes - insulin resistance [22:00]. Insulin resistance occurs when muscle and liver store excessive quantities of fat.
When the muscles and liver accumulate fat, insulin has a difficult time communicating with them, thus trapping glucose in your blood.
A low-fat, plant-based, whole-food diet significantly improves insulin sensitivity, by reducing the amount of tissue fat, and optimizing the ability of muscle and liver to communicate with insulin.
This increase in insulin sensitivity also decreases the risk of diabetes complications [23:48]. Additionally, when your body is receiving sufficient calories and your insulin sensitivity is high, your muscles receive large quantities of glucose to support an active lifestyle [32:35].
It’s important to understand that insulin is a required biological hormone and the best approach is to focus on increasing insulin sensitivity, rather than simply decreasing total insulin [26:07].
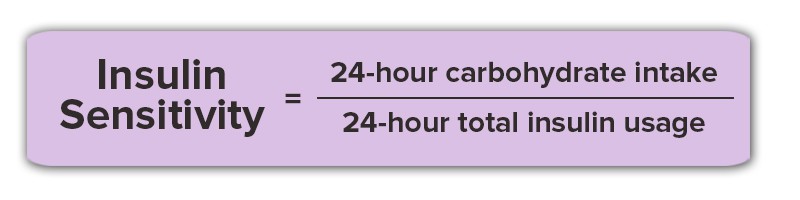
To calculate insulin sensitivity, simply divide the total number of grams of carbohydrates eaten in 24-hours by the total number of units of insulin injected. This can only be calculated in those that are insulin-dependent:
The Positive Changes I Experienced Eating a Plant-Based Diet
Eating a low-fat, plant-based, whole-food diet can result in radical health gains beyond increased insulin sensitivity. In my case, I was able to stop taking a number of medications for acne (including accutane) and allergies (Claritin-D). I also no longer suffer from plantar fasciitis [42:43].
In the Mastering Diabetes Online Group Coaching Program I run with Cyrus Khambatta, PhD, our clients often experience the following:
- Increased insulin sensitivity (more carbohydrates for less insulin)
- Reduced need for oral medications
- Decreased A1C (3-month marker of blood glucose control)
- Reduced total body inflammation
- Weight loss
- Increased flexibility
- Abundant energy
- Increased activity
- Increased mental clarity
- Significantly improved digestion
How To Handle Social Situations When You Eat Outside the Societal Norm
One aspect of eating a low-fat plant-based diet that can prove tricky is navigating social situations. There are many ways to modify menu choices to your nutrition goals, but it is important to stand up for your nutritional needs. I choose to take food with me to social events, because it allows me to monitor my portions accurately, thereby making insulin dosing more accurate [52:15].
Stand up for your needs, and give others the confidence to do the same.
I genuinely believe that maintaining a firm stance on your food choices is not rude. By doing so, you are choosing to manage your health, so that you can be your best self and give more to those around you.
Take Home Messages
- Keep fat intake consistent and at 15% or less of daily calories [27:42]
- Exercise regularly to help increase insulin sensitivity and control blood glucose [35:05]
- Make sure to eat enough calories [19:08]
- As your insulin sensitivity increases, you will need less insulin per gram of carbohydrate eaten [24:07]
- Enjoy your food! There is an incredible variety of foods in the plant world. Make the most of it!
Lower Your A1c and Get to Your Ideal Body Weight ... Guaranteed

Your results are guaranteed. Join more than 10,000 ecstatic members today
Personalized coaching puts you in immediate control of your diabetes health, helps you gain energy, improves your quality of life, and reduces or eliminates your meds.
Leave a Comment!
Tell us about your experience eating a plant-based diet below.

