A few weeks ago, we completed another successful Mastering Diabetes Retreat in Idyllwild, CA. This was our 4th diabetes retreat, and the improvement in insulin sensitivity in our attendees with type 1 diabetes was very consistent.
Think of the Mastering Diabetes Retreat as insulin sensitivity bootcamp. Every day is packed with information, exercise, fresh food, laughs and plenty of high-fives. From Thursday night through Monday morning, we ensure that you get the personal attention you need to understand exactly how to incorporate a low-fat, plant-based, whole-food lifestyle for maximum insulin sensitivity.
How much insulin sensitivity can you gain in 4 days?
Most people think that 4 days is not enough to see dramatic improvements in blood glucose, energy levels or weight loss. I’ll be the first to admit that when we started our diabetes retreats, we thought the same thing.
However, after reflecting on the rapid improvements in blood glucose and speedy decreases in insulin need that many of our clients experience, it became obvious that rapid increases in insulin sensitivity are possible in as little as 24-48 hours.
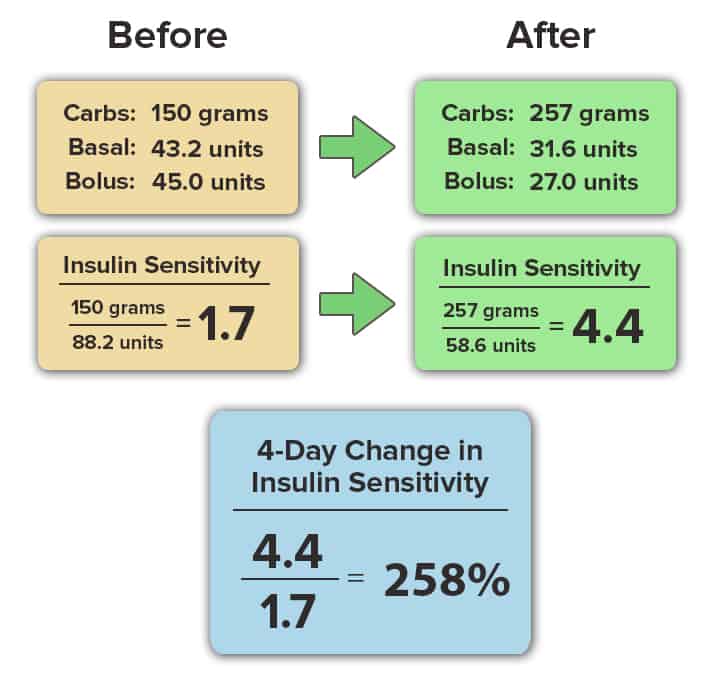
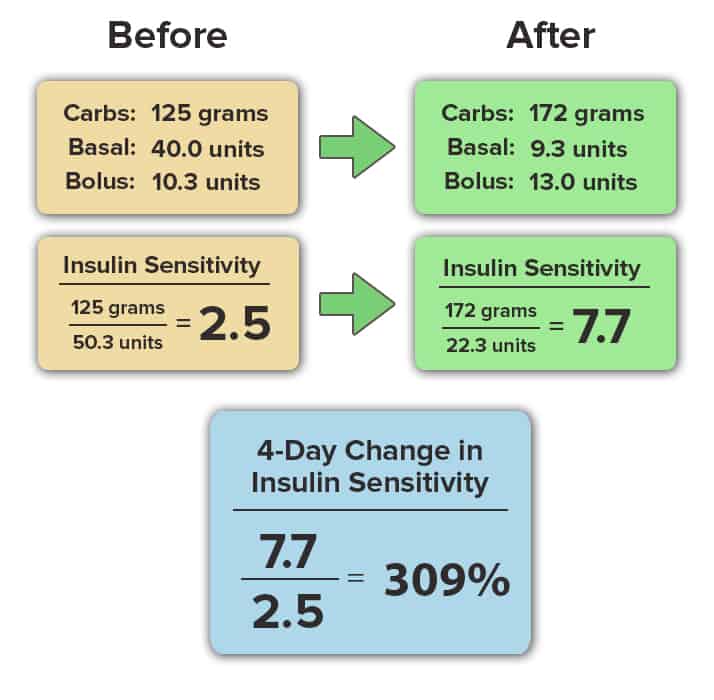
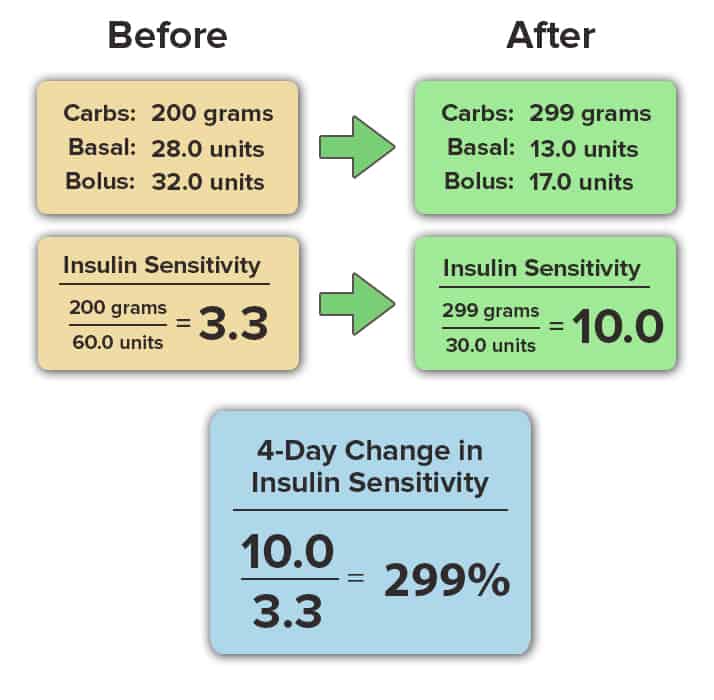
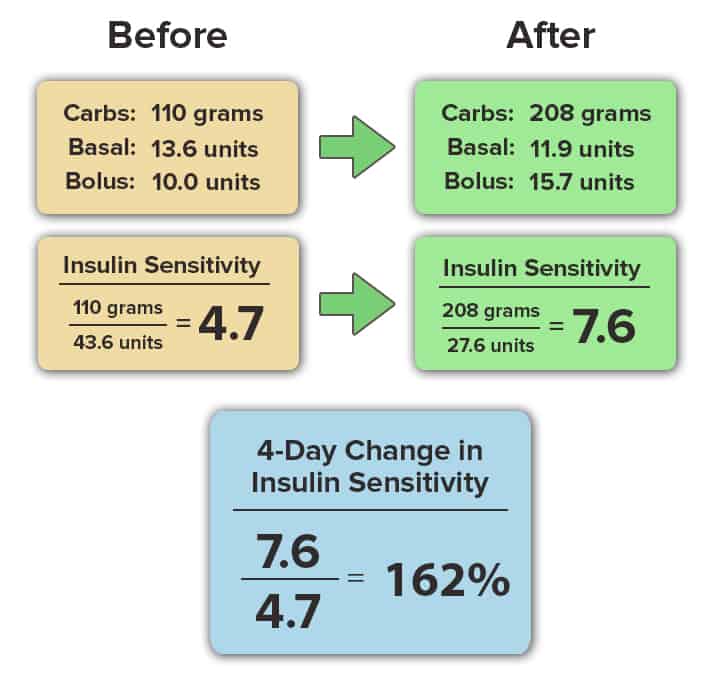
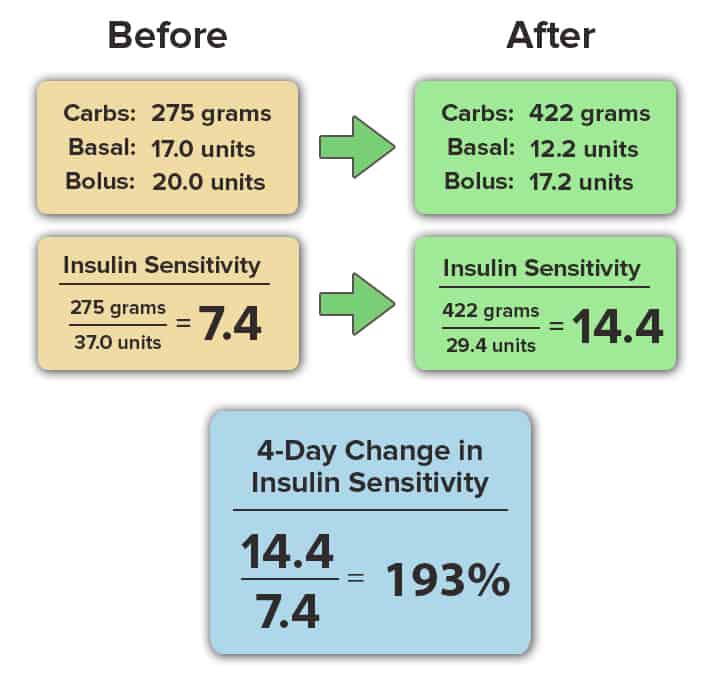
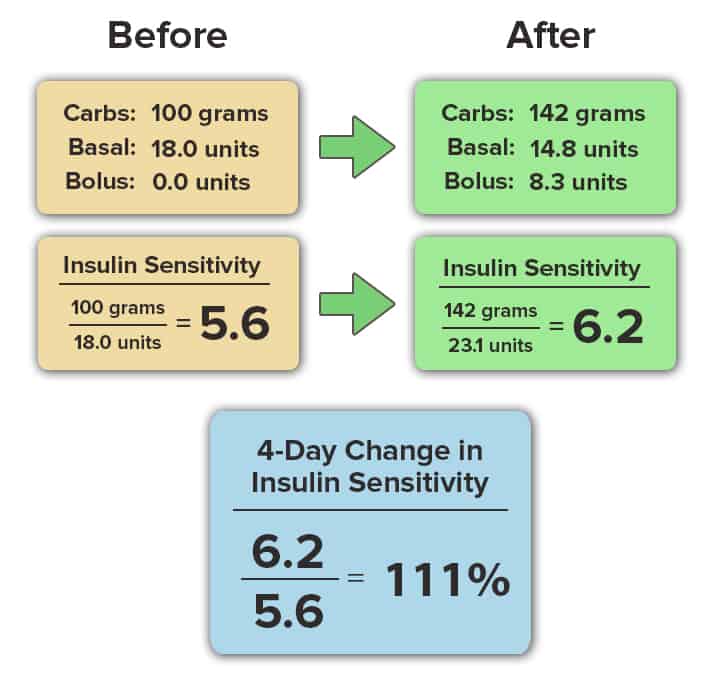
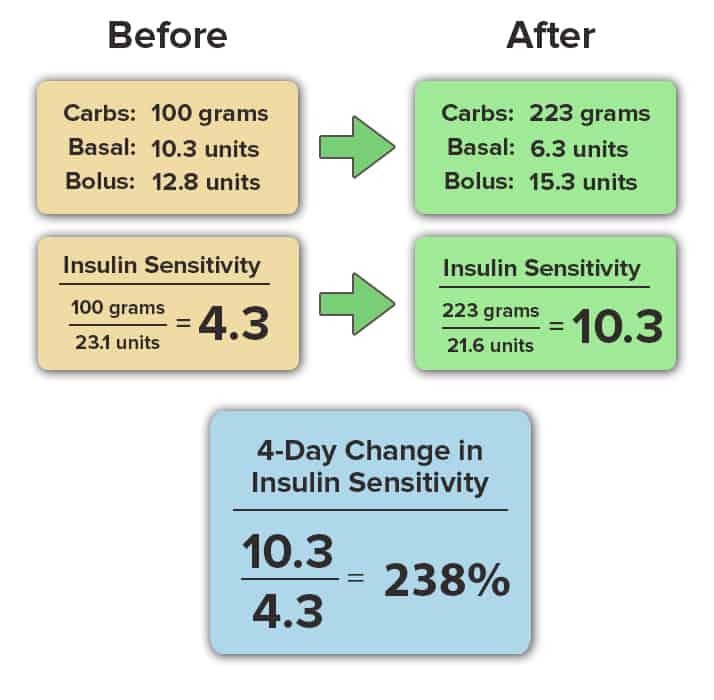
Insulin sensitivity is calculated as the ratio of your total carbohydrate intake to your total insulin use (basal and bolus) in a 24-hour period. This number is calculated only when you maintain your blood glucose in the normal range (70-130 mg/dL) for more than 80% of the day. The calculation is shown here:
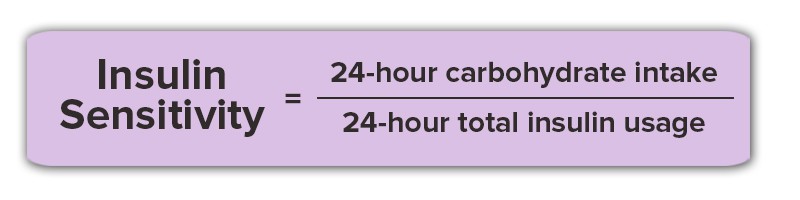
Our attendees results speak for themselves. In this article, we’ll share the change in insulin sensitivity that occurred at our last diabetes retreat in 7 insulin-dependent attendees living with either type 1 or type 2 diabetes.
Data Collection
We teach all of our attendees to fill out a daily Decision Tree, a food, exercise and medication dosing log that provides us with detailed information about their blood glucose patterns over the course of a 24-hour period. The process is designed to provide both the attendee and us detailed information about how their insulin sensitivity changes over time as they improve their eating and movement habits.
By analyzing this data on a daily basis, we are able to visualize how a low-fat, plant-based, whole-food diet can promote significant improvements in insulin sensitivity in a short period of time. This provides everyone with insight about how to reduce oral medication and insulin use while maximizing whole carbohydrate intake from unprocessed fruits and vegetables.
Please note that the names of each attendee below has been removed to protect their identity and personal health information. The data was recorded in detail over the course of the 4-day diabetes retreat, and all data are averages of the 4-day period. All personal information has been removed.
As you can see, the improvement in insulin sensitivity occurred in all individuals shown above, and did not depend on their sex, age, duration of time living with diabetes or baseline A1c value. The biology of insulin sensitivity is universal, and following a low-fat, plant-based, whole-food diet is the most effective eating pattern to reverse insulin resistance.
Take Home Messages
- 24-hour insulin sensitivity is calculated by dividing your total carbohydrate intake by your total insulin use (basal plus bolus) over a 24 hour period
- All of our insulin-dependent attendees experienced a significant increase in insulin sensitivity within 4 days in a retreat setting
- A low-fat, plant-based, whole-food diet is your #1 most effective way to increase insulin sensitivity
Lower Your A1c and Get to Your Ideal Body Weight ... Guaranteed

Your results are guaranteed. Join more than 2,000 members today
Personalized coaching puts you in immediate control of your diabetes health, helps you gain energy, improves your quality of life, and reduces or eliminates your meds.