
Without doubt, the human brain is the most sophisticated biological machine in existence.
In fact, the human brain is so sophisticated that it can’t even understand itself.
Modern science has discovered many interesting facts about how your brain functions, including the location of your memory center, the location of your speech center, where long-term memories are formed, and how sleep restores neurological function.
Yet despite a deep understanding of this organ, scientists routinely debate the answer to an incredibly basic question:
What Is Your Brain's Optimal Fuel Source?
It’s a simple question with a simple answer, but unfortunately the answer has become overly complicated due to conflicting dietary philosophies.
Attempting to understand how to fuel your brain optimally is a challenging task indeed. Read 10 articles on the internet and you’ll likely get 10 different answers. Read 10 more articles and you’re bound to get utterly confused.
In the quest for understanding what to eat to fuel your brain optimally, the two most prominent arguments are:
In order to get to the bottom of this debate, let’s dig into basic brain physiology and understand the logic behind both arguments.
Argument #1: Your Brain Runs Best When Fueled by Glucose
Make no mistake, your brain is the most selfish organ in your body. Think of your brain as a metabolic pig – constantly taking energy from the bloodstream and storing none of it for itself.
It’s no wonder that your brain is one of the hungriest organs in your body – more than 80 billion neurons are sending and receiving electrical signals 24 hours a day, creating complex thoughts and emotions.
Even when you are asleep, neurons in your brain are busy sending a flurry of electrical signals from one region to the next, consolidating memories and information from the previous day. To put things in perspective:
Your brain occupies only 2% of your body weight but consumes about 20% of your body’s oxygen and up to 50% of your body’s glucose.
Unlike your muscle and liver, your brain cannot store fuel, it simply oxidizes (or burns) fuel on demand.
In addition, your muscle and liver are capable of oxidizing glucose, amino acids, and fatty acids for energy, whereas your brain oxidizes glucose easily, and cannot oxidize either amino acids or fatty acids for energy.
Your brain lacks the biological mechanisms necessary to burn amino acids and fatty acids, and therefore must rely on glucose for the bulk of its energy demands.
Think of your brain as a picky child, burning glucose almost exclusively, incapable of burning amino acids and fatty acids at any cost.
Your brain is so picky in fact, it is specifically designed to operate on glucose for 99.9999% of your waking life, and only switches to oxidizing ketones when carbohydrates are in short supply in your diet.
Hypoglycemia is Brain Starvation
Given what you now know about your brain’s ability to use only glucose as fuel, when the concentration of glucose in your blood falls, your brain is one of the first organs to recognize the problem.
When threatened by low blood glucose, your brain is actually starved for fuel, resulting in confusion, lightheadedness, a loss of balance, slurred speech, and impaired vision. This state is called hypoglycemia, or low blood glucose.
Hypoglycemia can be very dangerous and sometimes fatal – when your brain is starved for glucose, your cognitive abilities rapidly decline, resulting in a system-wide panic.
That’s why it’s very important to ensure that you recognize the symptoms of hypoglycemia immediately, and consume carbohydrate-rich food to restore your brain function back to normal once again.
Your Brain Despises Refined Sugars
Since glucose is the most important brain fuel, it stands to reason that a diet high in whole carbohydrate energy can make a significant positive impact on your cognitive ability.
Studies have shown that eating carbohydrate-rich whole foods can improve memory within an hour after ingestion, and that glucose from refined sources actually impairs brain function (1).
In a 2007 study entitled Dietary Influences on Cognitive Function with Aging, the authors describe how diet can affect brain function, and reason that “…[diets] high in fruits, vegetables, cereals, and fish are associated with better cognitive function and lower risk of dementia (1).”
That being said, refined sugars can have detrimental effects on brain function, especially for those living with any form of diabetes. Consume whole carbohydrate energy from plants rather than refined sweeteners from packages and bottles in order to maximize cognitive function.
Researchers have investigated the effects of refined sugars on cognitive function, and conclude that “Special care in food selection at meals should be exercised by those with type 2 diabetes since ingestion of rapidly absorbed, high–glycemic index carbohydrate foods further impairs medial temporal lobe function, with food-induced increases in oxidative stress and cytokine release likely explaining the association between food ingestion and reduction in cognitive function in those with type 2 diabetes (1).”
What are Ketones?
Ketones or ketone bodies are a collection of fuels that your liver is capable of manufacturing when your brain is deprived of glucose.
If you eat a ketogenic diet and restrict your carbohydrate intake to approximately 30 grams per day, your selfish brain says, “Hey, I need some more glucose! If you don’t have any left, then provide me with another fuel that I can use to stay alive.”
Your liver then responds by converting stored fatty acids (from meats, eggs, dairy, and fatty vegetables) into ketone bodies, to be used as an emergency backup fuel to keep your brain happy. Your liver makes 3 primary ketones, named acetone, acetoacetate, and 2-hydroxybutyric acid (or beta-hydroxybutyric acid).
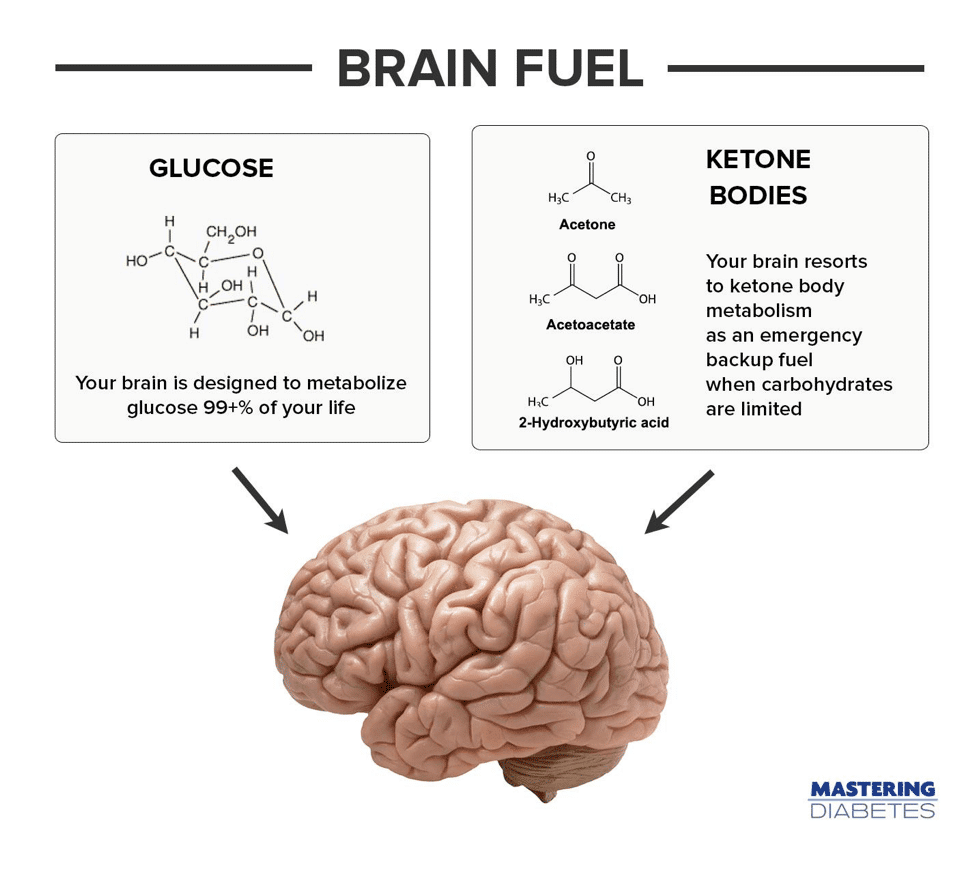
These ketones are shuttled to your brain to be used as backup fuels, to keep your brain operating at full capacity. Because your brain is a finely tuned organ, it may take a few days to adapt from oxidizing glucose to oxidizing ketones.
In the same way that your laptop computer has a backup battery when a wall outlet is unavailable, ketone bodies are the backup power source for your brain when carbohydrates are out of reach.
Side Effects of Ketogenic Diets
Originally developed as a treatment for epilepsy, ketogenic diets result in flatline blood glucose profiles and reduced A1c values, both of which are positive indicators that your diabetes health is improving.
In the short term, restricting carbohydrate intake can dampen overall cognitive function (2). In a study conducted in 2008, women placed on a low-carbohydrate diet for 28 days suffered from impaired reaction time and reduced spatial memory compared to women placed on a high-carbohydrate diet.
The researchers concluded that, “The brain needs glucose for energy and diets low in carbohydrates can be detrimental to learning, memory, and thinking (3).”
It’s also important to understand that just because a diet flatlines your blood glucose does NOT mean that it is a safe diet in the long-term. Ample scientific evidence shows that ketogenic diets come with a laundry list of unwanted side effects that simply cannot be overlooked (4), shown here:
These side effects are chronic health conditions that are fueled by a diet low in carbohydrates, high in fat, high in protein, and low in water, antioxidants, vitamins, fiber and water.
Most importantly, low-carbohydrate diets increase your risk for all-cause mortality, premature death from any cause (5–13).
And independent of any other positive or negative outcome – if your diet increases your risk for premature death, it’s time to seriously reconsider your options.
Take Home Messages
To answer the question: What are ketones? – remember the following things:
Lower Your A1c and Get to Your Ideal Body Weight ... Guaranteed

Your results are guaranteed. Join more than 10,000 ecstatic members today
Personalized coaching puts you in immediate control of your diabetes health, helps you gain energy, improves your quality of life, and reduces or eliminates your meds.

