Meet Meghan.
Diagnosed with type 1 diabetes in 2008, Meghan has been living a low-carb lifestyle from the time she was first diagnosed. At the age of 10, she adopted a vegetarian lifestyle, and then transitioned to a vegan lifestyle in the middle of 2015.
Like most people living with type 1 diabetes, Meghan followed the traditional advice given to her by her medical team: restrict your carbohydrate intake in order to properly control your blood glucose.
So she did. She ate large quantities of nuts. And seeds. And avocados. And olive oil. And processed tortillas.
Meghan’s Solution
In February of 2016, Meghan decided to join our diabetes nutrition online coaching program, in the hopes that it would improve her blood glucose control. She was intrigued, yet skeptical because our philosophy of low-fat, plant-based, whole-food nutrition went against everything she thought to be true.
In the first week of her new low-fat, plant-based, whole-food lifestyle, Meghan dropped her insulin use by more than 25% while almost doubling her total carbohydrate intake. In order to avoid frequent hypoglycemia, Meghan quickly reduced her insulin use, faster than she had anticipated.
Similar to Jessica, Meghan now has more energy than she knows what to do with, and no longer needs coffee to power her through the day.
Change in Insulin Sensitivity After 3 Months
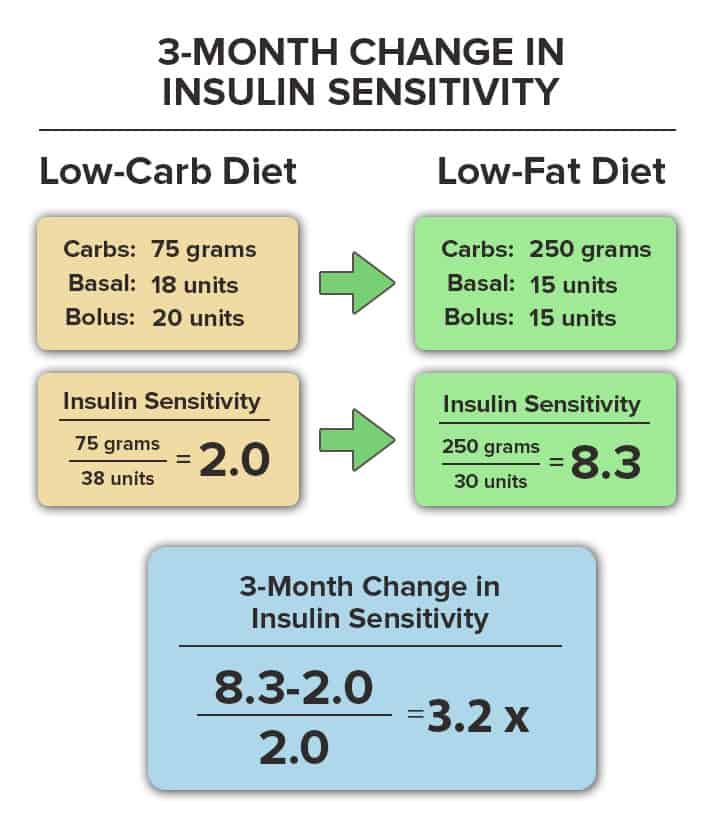
Before Meghan changed her lifestyle, she averaged a proximately 75 grams of carbohydrate per day, and injected a total of 38 units of insulin per day. On a low-carb diet, her basal insulin requirement was about 18 units per day, and her total bolus insulin requirements averaged about 20 units per day.
Within 3 months of adopting a low-fat, plant-based, whole-food lifestyle, she had increased her carbohydrate intake to approximately 250 grams per day, and reduced both her basal and bolus insulin requirements to approximately 30 units per day.
Her basal insulin dropped from 18 units per day to 15 units per day, and her total bolus insulin use fell from 20 units per day to approximately 15 units per day.
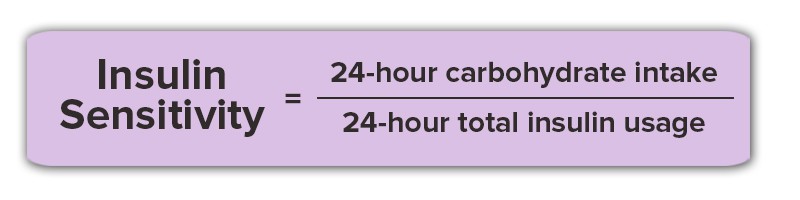
In this first 3 month period, her 24-hour insulin sensitivity increased from 2.0 grams per unit to 8.3 grams per unit, resulting in a 320% or 3.2-fold increase.

Change in Insulin Sensitivity After 6 Months
At the 6 month marker, Meghan had further increased her insulin sensitivity.
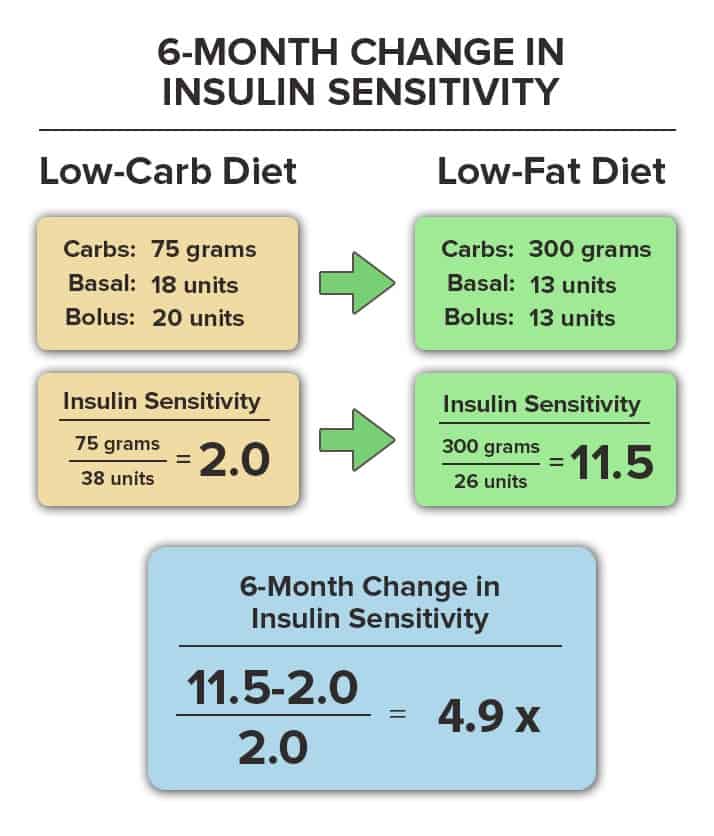
She increased her carbohydrate intake to approximately 300 grams per day, and further reduced both her basal and bolus insulin requirements to approximately 26 units per day, split between 13 units of basal insulin and 13 units of bolus insulin.
In this 6 month period, her 24-hour insulin sensitivity increased from 2.0 grams per unit to 11.5 grams per unit, resulting in a 485% or 4.9-fold increase.

Candidly, Meghan told us the following:
“I honestly would not have believed it if somebody just told me. I had to experience it to believe that it was true. It’s insane how quickly it [increased insulin sensitivity] happens.”
Change in Hemoglobin A1c Over 6 Months
None of the changes in insulin sensitivity described above would mean anything if her overall blood glucose control did not improve significantly. For that, we look to her hemoglobin A1c value, to understand how her average blood glucose control had changed as a result of a low-fat, plant-based, whole-food lifestyle.
- In February of 2016, Meghan's A1c was 8.1%.
- By May of 2016, her A1c had dropped to 6.9%.
- By August of 2016, her A1c had dropped to 6.3%.
She is a happy camper, given that an A1c value of 6.3% represents the best blood glucose control that she has had since the time she was diagnosed with type 1 diabetes in 2008.

Meghan's Advice
We asked Meghan to give her advice to someone considering changing their diet to help manage their blood glucose living with type 1 diabetes. Her response was simple:
“Just try it for a month because you seriously won’t go back… commit to doing it for a month and you won't go back. That's a guarantee!”
Lower Your A1c and Fasting Blood Sugar... Guaranteed

Your results are guaranteed. Join more than 10,000 ecstatic members today
Personalized coaching puts you in immediate control of your diabetes health, helps you gain energy, improves your quality of life, and reduces or eliminates your meds.
