Have you ever heard of OZEMPIC? As the kids would say, “It’s all the rage” on social media. Just in the past few weeks, there’s been an explosion of posts about Ozempic, a pharmaceutical medication that was designed to lower blood glucose in those living with T2D.
So why are people talking about it? Especially non-diabetic individuals? Well, it’s because many people are claiming it’s their silver bullet for weight loss, and the results that people are advertising are certainly very attractive.
You’re seeing studies on these weight loss drugs published in reputable journals, influencers are posting that they are losing large amounts of weight without changing their lifestyle, and suggesting that you can see results like losing 15% of your body weight, and start to lose weight in just two weeks.
It’s a lot of compelling claims, but as with every supposed miracle drug, we’re skeptical here at Mastering Diabetes. This is because of something we discuss all the time – people on the internet, and actually just humans in general, are obsessed with fun, fast, and easy results.
And that’s totally fine to look for, especially since the results in this case are admittedly very strong and supported by evidence. But the one thing that people suffer from – and this is in weight loss and with any form of chronic condition – is short-term thinking.
You’re looking for the quick answer NOW. But how does it work in the future? How will it affect your long term weight, lifestyle, and chronic diseases? Surely you don’t want to be exposing yourself to unknown disease risks, so it’s always worth reality-checking these compelling claims.

That’s why in this piece we’re going to break down the science behind this “miracle drug” and how it works. Then we’re going to review some of the results, the risks and side effects, and what happens if you stop taking Ozempic.
And finally, we’re going to take a big picture look and answer these big questions:
Why are people taking Ozempic in the first place?
Are people making the right decision to use it as an off-label weight loss drug?
What might be missing from the people looking at Ozempic as their “get skinny quick scheme”?
And is there any situation where we’d recommend Ozempic as part of your weight loss or diabetes strategy?
Let’s start by diving into the data.
The Science Behind Ozempic | Taking the Microscope to This “Miracle Drug”
Is Semaglutide (Ozempic) a Miracle Molecule?
Ozempic is a GLP-1 receptor agonist which means that it functions just like GLP-1, a hormone within your body that tells your body “there’s food in the system, we can stop being hungry right now.”
More specifically, GLP-1 sends signals that:
Actually distend your gut to make you feel full
Reduce the movement of food material in your gut to make you feel fuller
Reduce your appetite by signaling directly to your hypothalamus (in effect it says “I’m full, reduce appetite now)
Increase insulin secretion by your pancreas
This is really interesting, because it highlights one important way that humans are constructed – parallel pathways. Different parts of your body are constantly talking to other parts of your body, so a single peptide (like GLP-1) can stimulate mechanical receptors in nearby organs AND can stimulate neurons that send electrical signals to your brain.
Essentially, this is a bi-directional phone call between your gut and your brain that tells you you’re full, and reduces your desire to eat more calories. Happening naturally, this means that when you have a full belly, you don’t want to eat anymore.
This is one of the principal reasons why Oz is so popular. Because it doesn’t make you crave food. Instead, it decreases your appetite, which is always helpful when losing weight. Most weight loss programs force you to restrict your food intake and count calories/points/servings, which can be problematic in the long-term because it increases your desire to want to eat food.
Breaking Through the Recent Science and Surge of Popularity

Now let’s dive into the research for a bit because there’s some important information to learn about how semaglutide, the active ingredient in Ozempic, was studied in non-diabetic individuals.
The STEP-1 trial was tested in about 1961 non-diabetic patients, who had a BMI>30 or BMI>27+weight-related comorbidity. They were tested with a Semaglutide injection (2.4mg 1x/week injection) and the results were published in The New England Journal of Medicine.
After the 68 week long, individuals who were given Semaglutide lost an average of 14.9% of their body weight, whereas people who had just taken the placebo who saw a 2.4% change in body weight.
This is a clear, significant set of results for Semaglutide patients.
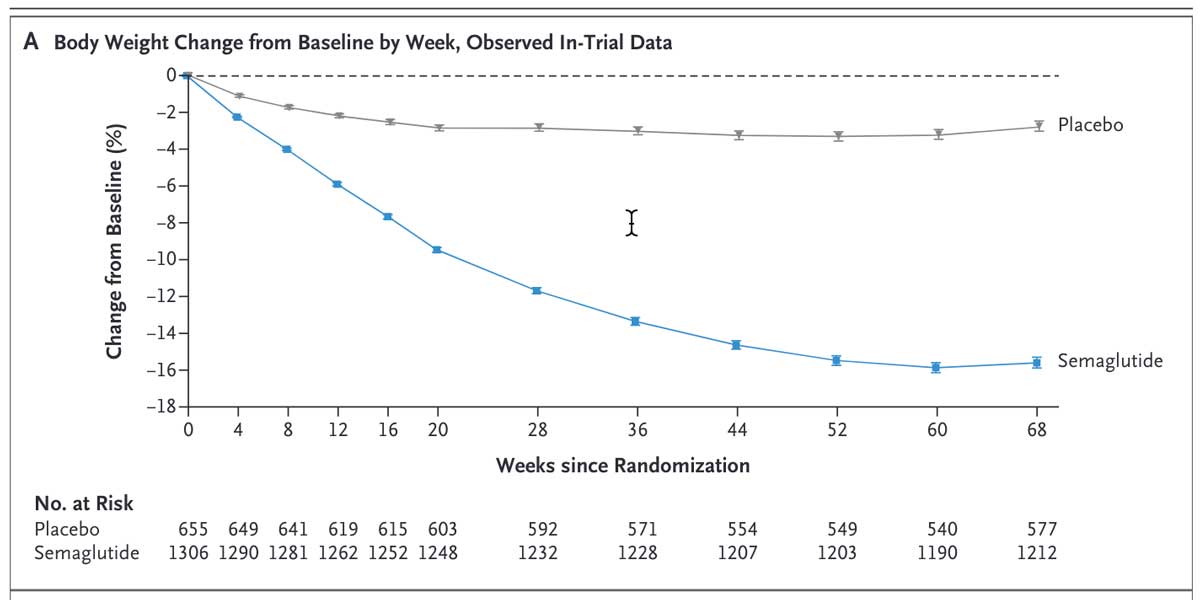
So the data is clear – Semaglutide (the active ingredient in Ozempic) does help you lose weight.
The Deceptively Tempting Results of Ozempic
So you can see why these results are tempting. Losing 15% of your body weight just from an injection taken once a week? And it’s published in a reputable journal, so why wouldn’t you believe it?
Well, the key here is to understand the side effects. There are other drugs that have shown similar weight-loss properties in a vacuum – things like methamphetamine, MDMA, cocaine – that are not recommended for your overall health.
We often joke here that the most effective weight loss drug ever invented is called the flu – just get it and watch as the weight melts off of you.
Of course, we’re joking but it’s important to understand that just because something helps you lose weight doesn’t mean that it’s safe. That’s why it’s important we also look at the side effects and risks of using a pharmaceutical drug to lose weight – both in the short-term and long-term.
Risks and Side Effects of Ozempic
Now if you check the Ozempic website, they’ve got a big friendly list of common side effects, which include gastrointestinal issues, including constipation, diarrhea, nausea, vomiting, and abdominal pain.
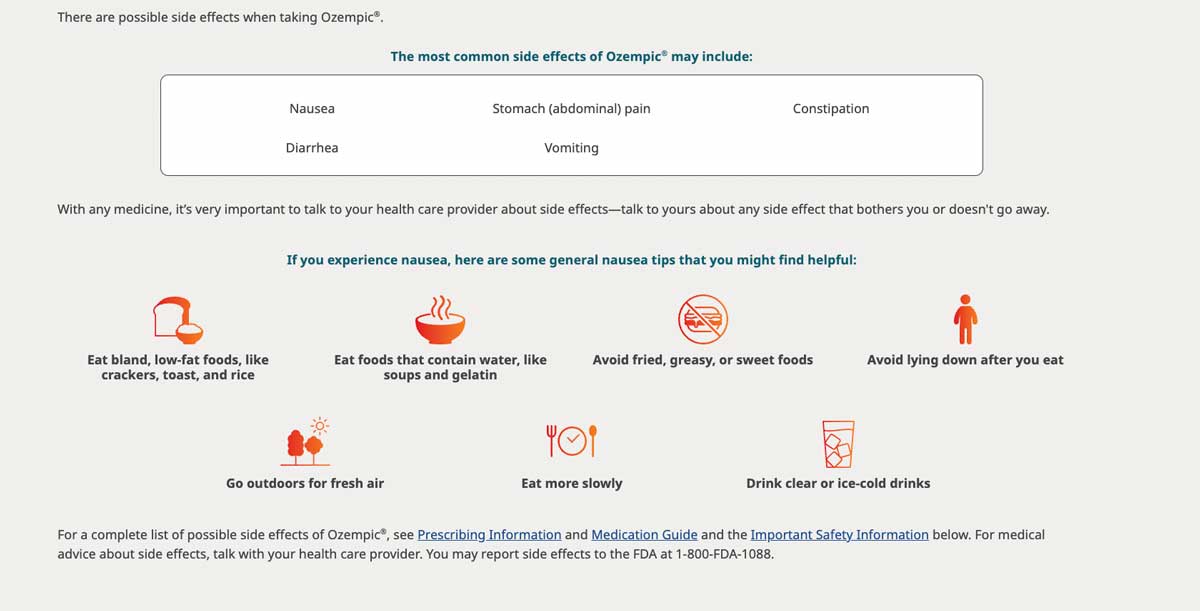
It is also contraindicated (flagged as UNSAFE) for patients who are living with MEN-2 or MTC (two specific forms of cancer).
This happened because studies in rats demonstrated that Semaglutide was associated with an increased risk of c-cell cancer, which is similar to that found in multiple endocrine neoplasia 2 (MEN-2) or medullary thyroid cancer (MTC).
It is also contraindicated for pregnant women, since there is insufficient data on the safety of Semaglutide in pregnant women (a huge ethical hurdle), as well as for individuals living with gastrointestinal issues (gallbladder disease, pancreatitis, and gastroparesis).
But if you’re thinking “well, compared to some drugs, that’s actually not that bad”, you might be right (though that certainly says something about the state of medicine in the U.S.). But the key problem with Ozempic isn’t the risks of side effects. In fact, it’s due to a glaring issue with Ozempic as a long-term solution.
The Crucial Problem with Ozempic | What Happens If I Stop Taking Ozempic?
Which, the long and short of it is that if you stop taking Ozempic, you are incredibly likely to gain back all of the weight you lost. So while you’re taking Ozempic you’re living your life with the potential for these side effects (and any long term side effects), and if you ever stop, you’re just back in the same place as the beginning.
This isn’t just hearsay either. In order to understand the effects of Ozempic in the long term, the STEP-4 trial (a sibling to the STEP-1 trial that showed Ozempic’s benefits) was tested in about 800 non-diabetic patients with either a BMI>30 or BMI>27 as well as a weight-related comorbidity.

This 68 week trial featured a 2.4mg semaglutide 1x/week injection, very similar to the STEP-1 trial, and saw similar reductions in body weight (-7.9%, compared to a GAIN of +6.9% in the placebo group).
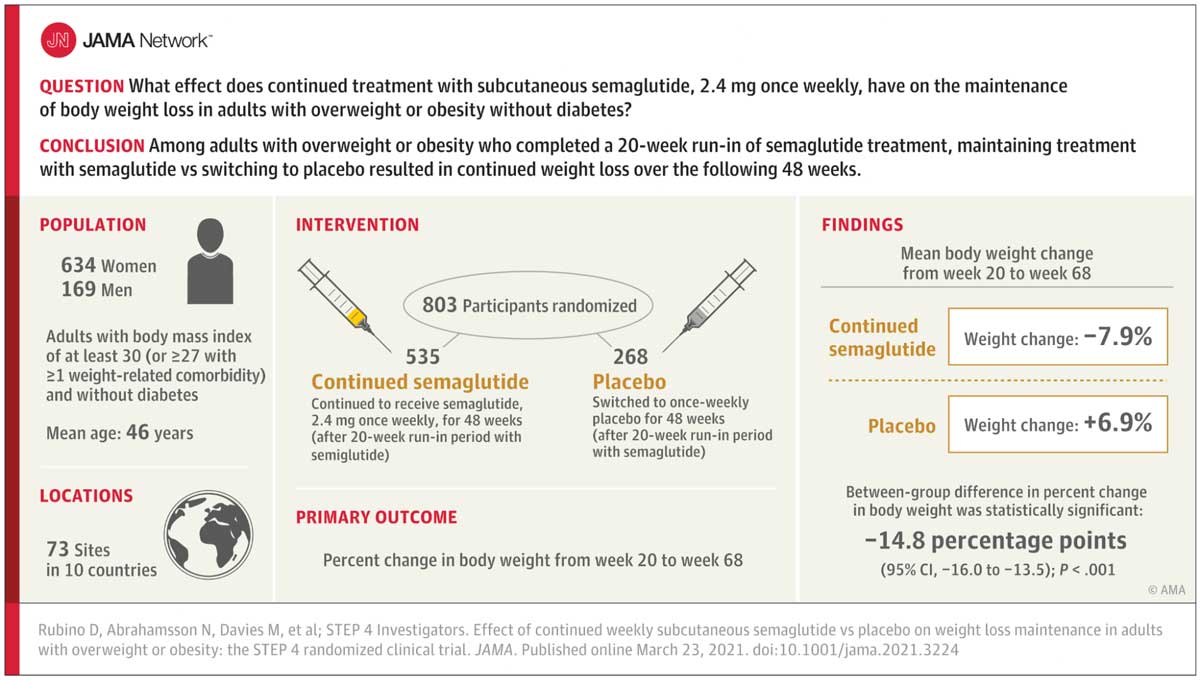
Once again, this confirms that semaglutide has an almost undisputed, independent weight loss effect.
But the same trial showed that semaglutide (and Ozempic) stops working when you stop taking. It’s similar to insulin in this way – insulin only works when you take it, and if you stop, it won’t help you lower your blood glucose anymore.
And the exact same STEP-4 trial that re-confirmed semaglutide’s power as a weight-loss drug also displayed its effects when you stop taking semaglutide. There was a smaller group who were administered semaglutide for 20 weeks and then stopped. And those who stopped taking semaglutide gained back the weight they originally lost AND MORE.
What This Means For You and Ozempic
So as the world is going bonkers for Ozempic, what does the research mean for you? And is Ozempic a viable strategy for weight loss (or diabetes management) in the long term?
Well, there are a few problems.
Problem 1: Ozempic is an Expensive Short-Term Band-Aid
People who are living with type 2 diabetes are typically prescribed Ozempic to lower their blood glucose. But more and more people are using it as an off-label weight-loss drug, thinking that with one weekly injection you can completely transform your life.
But the truth is that in most cases, Ozempic is a short-term solution for people that aren’t willing to put in the work to change their lifestyle. Essentially, a very fancy, very expensive band-aid.

It’s a fun, fast, and easy solution advertised so that you can keep living your life exactly the same way and see results. But not only are you exposing yourself to the listed side effects, there is still a LOT that we don’t know about Ozempic (including its cardiovascular risks, which are being trialed as we speak).
Combined with the fact that Ozempic stops working as soon as you stop taking it, and you’ve got a recipe for expensive, complicated, and potentially dangerous disappointment.
Problem 2: Ozempic is a Get-Skinny-Quick Scheme
And it’s this exact mindset – the search for easy ways out – that often traps people in chronic disease. The only consistent way to keep your weight down and fight chronic disease is through lifestyle decisions like eating a healthier diet (preferably one that’s low-fat, whole-food, and plant-based), exercising every day, cutting down on your drinking and smoking, and using tactics like intermittent fasting.
Think about it like this – when Ozempic is out of your system, all you’ll have left is the effects of your lifestyle. So if Ozempic comes and goes, and you’ve still got the other habits that caused weight gain or chronic disease, hanging out under the surface… well you haven’t really gone anywhere.

Problem 3: You Can Activate Stretch Receptors Using Food
Another problem with Ozempic is that you can easily replicate its effects with bulk, which is the presence of both fiber and water in your stomach, and activates the exact same receptors that Ozempic does.
Below is a passage from our book in which we discuss this concept:



So if activating stretch receptors triggers your brain to reduce your appetite (the exact same effect that Ozempic provides), then you have a choice
You can take Option 1, which is to activate stretch receptors in your small intestine by slowly increasing your fiber-rich food intake and making sure you drink enough water.
Or, you can take Option 2, which is to activate stretch receptors in your small intestine by injecting Ozempic, a medication known to increase your risk for thyroid cancer, gall bladder disease, pancreatitis, and gastrointestinal issues like nausea, constipation, and diarrhea, and as yet unknown cardiovascular side effects.
Problem 4: The Side Effects Simply Aren’t Worth It
If you were to learn that eating an apple may cause pancreatitis, would you do it? If you were to learn that eating a piece of chicken breast may cause gallbladder issues and thyroid issues, would you still do it?
Likely not. Yet people all around the world are clamoring for a get-fit-quick-scheme even when the answers are right in front of them. Convincing marketing certainly helps, but it comes back down to the fact that we instinctively seek out the easy option. It’s a hard truth of simply being human, which is why we took the time to point out in this article the resounding truth.
Ozempic is NOT your weight loss silver bullet.

When Do We Recommend Using Ozempic?
Well, we can’t recommend whether Ozempic is right for you. First of all, we’re not doctors, and the specifics of cases in which Ozempic is needed – in the case of extreme obesity, type 2 diabetes, and related comorbidities – require a very careful case-by-case use.
What we can say is that no weight-loss strategy is complete without dietary and lifestyle changes. There are certainly drugs and medicines that help with weight loss in the short term. But they aren’t ever going to replace doing the work and making the changes that will transform your life in the long term.

The good news is that you have the power to change your health today with lifestyle factors like we mentioned above – a low-fat, plant-based, whole-food diet, regular exercise, intermittent fasting, and cutting down on drinking and smoking.
And the only side effects of those drugs are happiness, improved mood, a slightly increased risk of scrapes and bruises from being active.The Final Word on Ozempic

Ozempic is popular right now, taking off just like all the other crazes before it. And just like other crazes like Keto, Carnivore, Paleo, etc., it’s got great short term data showcasing its effects.
There are viral videos with models talking about their experience using Ozempic, attractive and well-cut gentlemen teaching you where to get bootlegged Ozempic. And you can enjoy them – but also know that the people in those videos are putting in hard work day in and day out to get the REAL results.
And for the average person, Ozempic is powerful. But it’s also risky, and the moment you stop, if you haven’t made lifestyle changes…that body weight is coming back.
Fortunately, lifestyle change has no rubber-band effect, and no negative side effects. It always will be the answer – you just have to be willing to put in the hard work to change from the inside out.
In the same way that you can get away with cheating in high school, at some point you’re going to get caught. You can get away with cheating on your significant other, but at some point you’re going to get caught. You can get away with eating high calorie density foods, not exercising, drinking alcohol, and ignoring a plant-based lifestyle, and instead just use Ozempic for weight loss but at some point, it’s going to catch up.
If there’s anything you get from this article, it should be the realization that you have the power at any moment in time to change the course of your life. But, you have to be the one to accept the challenge, rise to the occasion and take control of your life.



