
In a recent study published in the journal Lancet, 135,000 people from 18 countries were followed over the course of 7.5 years to determine how their food choices affected their risk of death from cardiovascular disease, stroke, and non-cardiovascular disease (1).
This study, called the Prospective Urban Rural Epidemiology (PURE) study, investigated the relationship between those that ate high carbohydrate foods and those that ate higher fat foods on cardiovascular disease and overall mortality.
After performing an analysis on the mortality of individuals from all around the world, researchers from this study conclude that eating a diet containing a high percentage of calories from carbohydrates from high carbohydrate foods is associated with an increased risk of total mortality, and that eating a diet containing a minimum of 30% of energy from fat and a minimum of 10% of energy from saturated fat reduces your risk of death.
Based on the number of people in the study (135,000) and the length of time of the study period (7.5 years), many people may consider these results to be groundbreaking. Unfortunately, there are many limitations to the study, and as a result these data are very untrustworthy.
In this article we’ll explain:
- Important flaws in the study design that limit the credibility of the PURE study data
- Why all high carbohydrate foods are not created equal, and why the type of carbohydrate you eat is as important as the quantity of carbohydrate you eat
- Why those who ate more protein-rich foods in the PURE study actually lived longer because of better access to healthcare
- Why focusing on macronutrients (instead of food) misleads both the general public and accomplished scientific researchers
Poor Study Design Leads to Untrustworthy Data
It’s almost impossible to gather relevant data from a study with a poor design from the onset. This study is a classic example of an investigation that was designed to fail from the beginning. There are many reasons why, including the following:
Reason #1: The study asked people to recall their food intake using a questionnaire at the beginning of the study, which is problematic because dietary recall questionnaires are notoriously inaccurate.
Reason #2: The study did not ask people to recall their food intake at ANY point during the following 7.5 years. If they changed their diet, this information would have been missed entirely.
Reason #3: The data that they did gather on the participants’ diets was not analyzed with enough attention to detail, including failure to differentiate between processed or whole foods (as we will explain further in the next section).
The authors state the limitations of their study design by writing the following:

All Carbohydrate-Rich Foods Are Not Created Equal
The authors of this study conclude that eating a diet greater than 60% of carbohydrate energy containing high carbohydrate foods is associated with an increased risk of death, and that a diet containing more than 30% fat with less high carbohydrate foods leads to improved longevity.

They found that participants in low- and middle-income countries consumed more high carbohydrate foods, which suggests that their fat and protein intake were correspondingly low.
The authors state, “...most participants from low-income and middle-income countries consumed a very high carbohydrate diet (at least 60% of energy), especially from refined sources (such as white rice and white bread).”
Furthermore, they were “...unable to quantify separately the types of carbohydrate (refined vs. whole grains) consumed. However, carbohydrate consumption in low-income and middle-income countries is mainly from refined sources.”
It is imperative to understand that whole high carbohydrate foods such as fruits, starchy vegetables, non-starchy vegetables, legumes, and whole grains are associated with increased health and longevity (2–4,4–21), whereas refined high carbohydrate foods are associated with an increased risk of disease and mortality (22–31).
Why then, would they blame “carbohydrates” in general for worse health outcomes rather than blaming “refined carbohydrates” from white rice and bread? This is simply poor data analysis.
The type of carbohydrate you consume is a very important determinant of your long-term disease risk. Refined high carbohydrate foods increase your risk for cardiovascular disease whereas whole high carbohydrate foods decrease your overall chronic disease risk.
Those Eating More Protein Had Better Access to Healthcare
This study reported that “total protein intake was inversely associated with risks of total mortality and non-cardiovascular disease mortality,” suggesting that higher protein leads to less risk of death.
A closer look at the data reveals something very important – countries where people ate a large amount of foods containing refined carbohydrates also had lower median income levels and poor access to education. This suggests that higher rates of mortality in these countries is likely not related to a single variable like food when so many other variables that influence health exist.
So is it higher protein that reduces mortality or access to better healthcare that makes the difference?
The latter makes more sense, given a large collection of research that shows that higher protein intake is associated with a significantly higher risk of all-cause mortality and chronic disease (32,33,33–52).
Food is More Important than Macronutrients
In the world of nutrition, people talk more about carbohydrate, fat, and protein, and often omit talking about food. The PURE study is a perfect example of mistaking whole food for isolated macronutrients.
Whole foods contain a collection of macronutrients and micronutrients, as illustrated by the following picture. A peach is not just one macronutrient (carbohydrates), but actually contains all three, along with important micronutrients. This the the case for ALL whole foods.
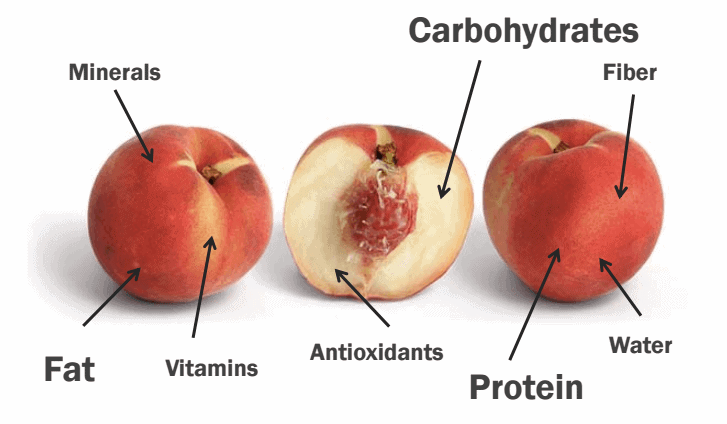
Talking about a macronutrient profile means little without discussing the specific foods that contain a multitude of biological components.
For example, a meal containing high carbohydrate foods containing 60% carbohydrate, 20% protein, and 20% fat could be:
- Black bean stew served over sweet potatoes and topped with avocado
- A white bread sandwich with 2 slices of processed lunch meat and a single slice of Kraft American cheese, with a can of Pepsi on the side
Both meals contain 60% carbohydrate.
Both meals contain 20% protein.
Both meals contain 20% fat.
But the nutrient content, and the way that these meals affect our health, is extremely different.
Meal 1 contains all whole foods, is anti-inflammatory, and reduces your chronic disease risk. It is high in fiber, nutrients, vitamins, minerals, and antioxidants. It promotes a healthy body weight, insulin sensitivity, energy, heart health, and longevity.
Meal 2 contains all processed foods, is proinflammatory, and increases your chronic disease risk. It is highly processed, nearly devoid of fiber or any other nutrition. It promotes atherosclerosis, high blood pressure, insulin resistance, low energy due to a blood sugar spike and the resulting fall, weight gain, and greater risk of mortality.
Humans don’t eat carbohydrate, protein, and fat. We eat potato chips, brown rice, lentils, chicken, spinach, salmon, swiss cheese, skittles, olive oil, bananas, quinoa, etc. How these foods act in our bodies is affected but not determined by their macronutrient profile.
When you focus on macronutrients, you miss the bigger picture. This is exactly what the PURE does by analyzing the effect of carbohydrates, fat, and protein without focusing on whole foods.
Let’s make the PURE study a lesson in the detriment of reducing whole foods to their isolated macronutrients, and remember that a reductionist approach severely limits your ability to understand the elegance of whole food nutrition.
Lower Your A1c and Get to Your Ideal Body Weight ... Guaranteed

Your results are guaranteed. Join more than 10,000 ecstatic members today
Personalized coaching puts you in immediate control of your diabetes health, helps you gain energy, improves your quality of life, and reduces or eliminates your meds.
Enter to Win Free Coaching!
Share this article on social media AND leave a comment below, and you will be entered in a drawing to win 6 FREE MONTHS of coaching ($174 value)!

