How much protein do I need?
In the world of nutrition, there is a large debate about the effectiveness of low-carbohydrate vs. high-carbohydrate diets, as well as low-fat vs. high-fat diets.
That being said, the one macronutrient that most people believe is always good to get in larger quantities is PROTEIN.
Especially in the world of diabetes, protein is king. Doctors, nurses, and nutrition professionals often recommend eating more protein to “stabilize” blood glucose.
You may have asked yourself these questions:
Researchers at the Longevity Institute at the University of Southern California investigated these exact questions, and published a ground-breaking research paper in 2014 that described the benefits and drawbacks of increasing protein intake (1).
Study Design
Using data from the NHANES II Study, researchers investigated the link between protein intake and mortality in men and women age 50 and over. There was a total of 6,381 adults in the study, with a follow-up period of 18 years.
Specifically, the researchers investigated how low, medium, and high protein intake affected diabetes mortality, cardiovascular mortality, and cancer risk.
Participants were separated into three groups based on how much protein they consumed in a day:
- Low protein group: participants ate less than 10% of daily calories as protein
- Moderate protein group: participants ate between 10-19% of daily calories as protein
- High protein group: participants ate 20% of more of daily calories as protein
To put these numbers into perspective:
- The average American consumes approximately 16% of calories from protein (medium-protein group).
- Low-carbohydrate diets often range between 20-35% of calories from protein (high-protein group).
Results
According to the study:
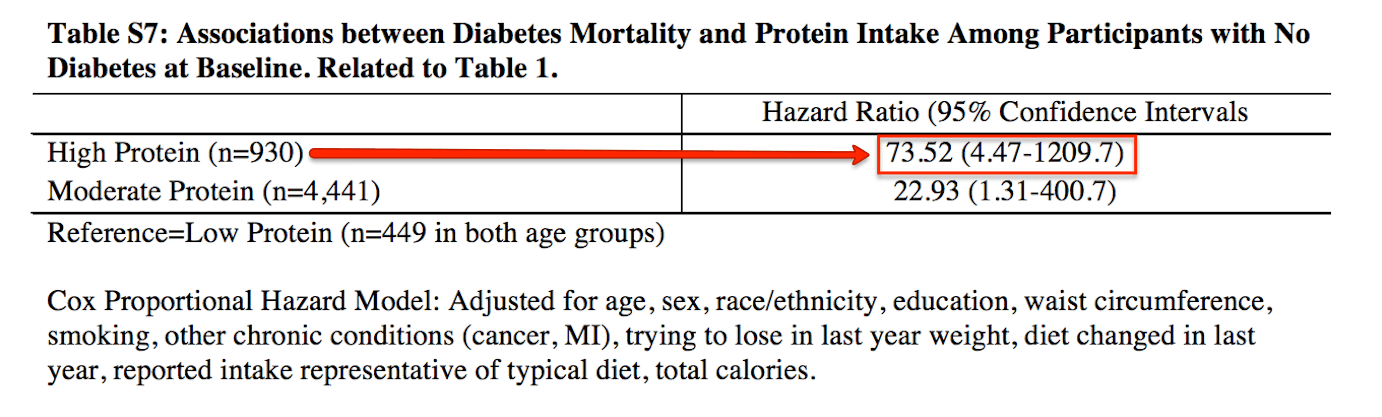
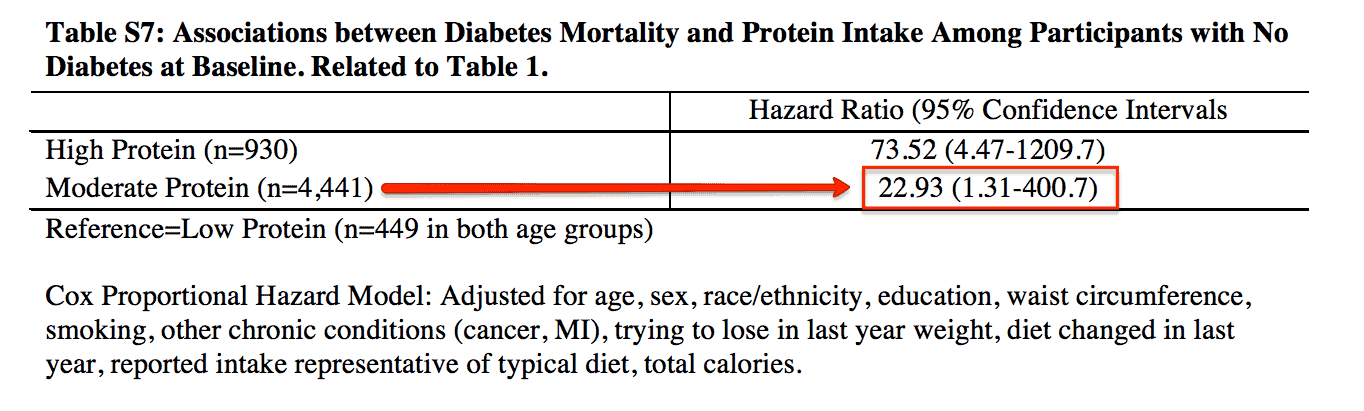
"Among subjects with no diabetes at baseline, those in the high protein group had a 73-fold increase in risk, while those in the moderate protein category had an almost 23-fold increase in the risk of diabetes mortality."
Let’s break those numbers down in more detail.
In comparison to those eating less than 10% of calories from protein, those who ate between 10-19% of daily calories from protein were 23 times more likely to die from diabetes.
For those eating more than 20% of daily calories from protein, the risk of dying from diabetes was 73 times higher.
These numbers are large. Very large.
To put things into perspective, high blood pressure increases your risk of developing diabetes by 60% (2). This study showed that eating a high-protein diet increases your risk of developing diabetes by 73-fold, or 7300%.
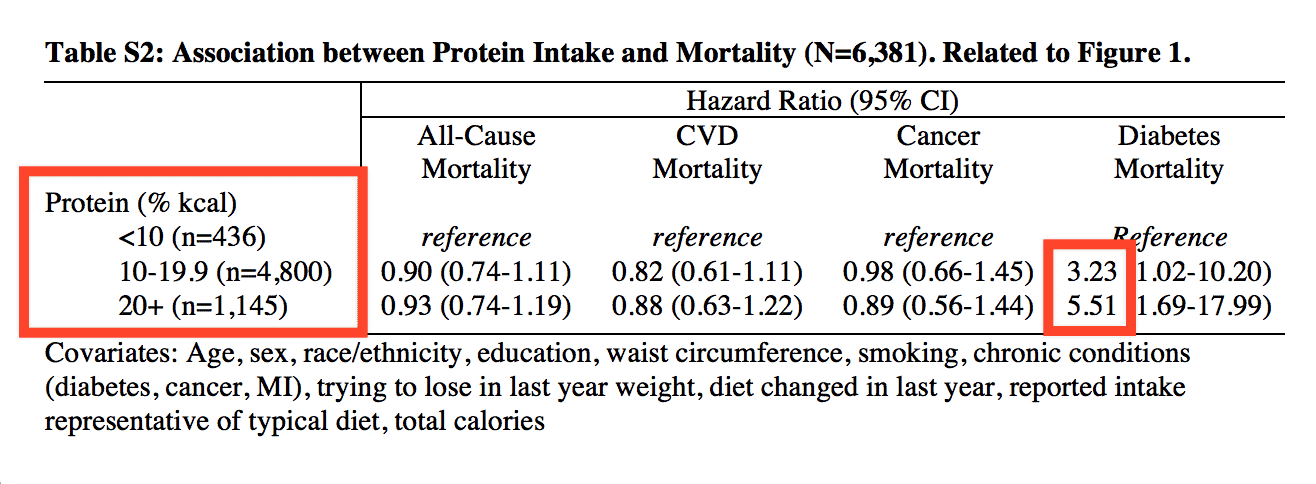
But it wasn’t just diabetes that was affected by a medium or high protein intake. For those age 50-65, eating a moderate or high protein diet increased both cancer mortality as well as all-cause mortality (premature death from any cause).
“In this age range, subjects in the high protein group had a 74% increase in their relative risk of all-cause mortality and were more than four times as likely to die of cancer when compared to those in the low protein group.”
Animal protein made up the majority of the protein consumed by people in this study, and the study authors theorized that this plays a major role in the extent to which high protein intake increases your risk for premature death.
They concluded that:
"...the risks may be somewhat decreased if protein does not come from an animal source."
Around age 65, the ideal amount of dietary protein changes.
For those age 65 and over, eating more protein decreased both cancer mortality and all-cause mortality for those eating a moderate protein or high protein diet.
Interestingly, the effect of protein intake on diabetes mortality stayed the same. The more protein study participants ate, the more their risk of dying from diabetes increased, as shown in the images below:
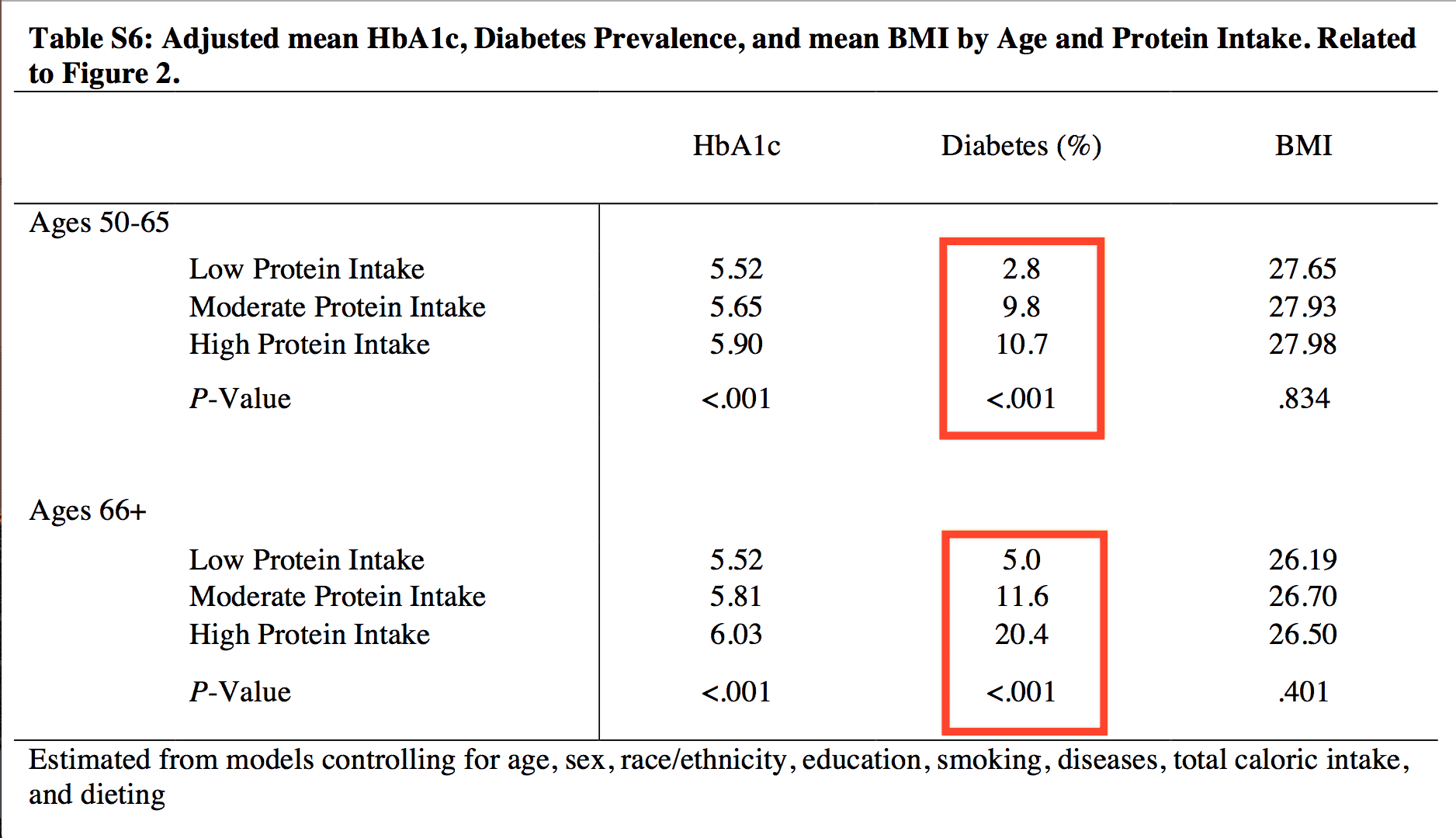
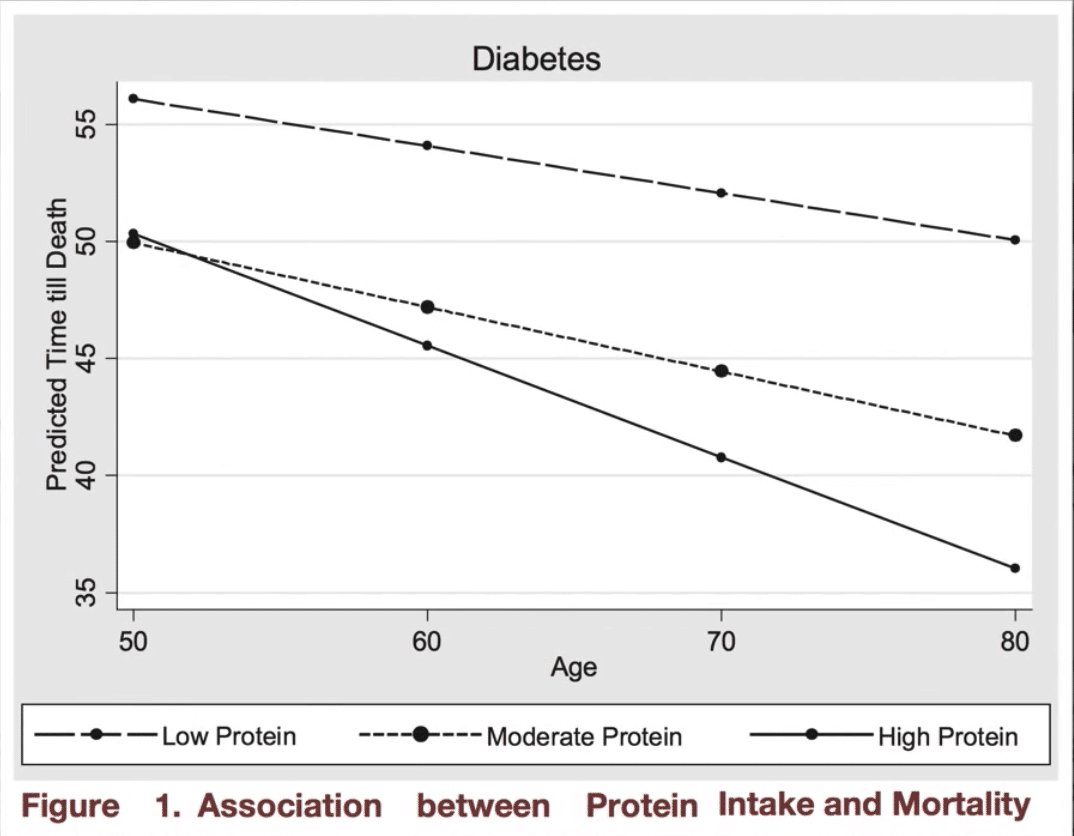
Age-Related Differences in Protein Requirements
Beyond the age of 65, the human body loses muscle mass up to six times faster than those aged less than 65 (3).
Given that falling is a leading cause of death for seniors, it is important to maintain muscle mass and protect against sarcopenia (muscle loss).
Researchers speculated that a higher protein intake may protect against muscle loss after the age of 65.
However, a much more effective way to preserve muscle mass is by performing resistance training or basic strength training exercise. The phrase “use it or lose it” is an increasingly important statement with age.
But if you increase your protein intake as you age, are you increasing your risk for diabetes mortality?
Not so fast.
Some studies indicate the increasing vegetable consumption can prevent loss of muscle mass (4). One study in particular found that eating the recommended 5 daily servings of vegetables cuts your risk of losing muscle essentially in half (by 48%) (5).
How Much Protein Do I Need?
We know, you’re still wondering, “How much protein do I need?"
It turns out that the most important aspect of your protein intake may not be the amount of protein, but the type of protein you consume.
As we discussed above, animal protein was responsible for the majority of the increased risk for diabetes, cancer, cardiovascular, and all-cause mortality presented in the study.

What this means is simple – for optimal metabolic health, focus on eating protein from plant sources rather than from animal products.
The authors conclude that:
"...[these] findings suggest that a diet in which plant-based nutrients represent the majority of the food intake is likely to maximize health benefits in all age groups."
Other studies have also shown a strong link between the consumption of animal products and the development of insulin resistance and diabetes, and some researchers believe that eating meat should be considered a risk factor for diabetes (6).
Is It Time to Stop Recommending High Protein Diets for Diabetes Control?
We certainly believe so.
This is not the first study to suggest that eating a high protein diet can be dangerous for long-term health.
Decades of research confirm that eating a high protein diet, especially when the protein comes primarily or exclusively from animal products, leads to an and puts you at risk for developing heart disease, cancer, hypertension, and obesity (7-13).
Based on the data that we currently have available, recommending a high-protein diet to those living with diabetes is not an evidence-based recommendation.
Thankfully, there is another option for minimizing your risk for diabetes mortality, and has myriad other health benefits such as increased insulin sensitivity, sustained weight loss, lower risk for all chronic diseases, and greater longevity (14-19).
This option is a low-fat, plant-based, whole-food diet. This lifestyle is naturally lower in protein, yet still easily meets and often exceeds the recommended daily amount (20-22).
All yes, ALL plant foods contain protein, and as long as you eat enough calories from whole foods, you will meet or exceed your daily protein needs.
Take Home Message
So, to finally answer your question, “How much protein do I need?” here’s what we conclude based on the best evidence currently available:
- If you less than 65 years old, eat less than 10% of your calories from protein.
- If you are 65 years or older, eat 10-15% of your calories from protein.
- Regardless of your age, eat plant-based sources of protein to keep your risk for premature death at a minimum.
Lower Your A1c and Get to Your Ideal Body Weight ... Guaranteed

Your results are guaranteed. Join more than 2,000 members today
Personalized coaching puts you in immediate control of your diabetes health, helps you gain energy, improves your quality of life, and reduces or eliminates your meds.

